What are the other Names for this Condition? (Also known as/Synonyms)
- Diabetes - Type 1
- Insulin-Dependent Diabetes
- Juvenile Onset Diabetes
What is Type 1 Diabetes? (Definition/Background Information)
- Type 1 Diabetes is a chronic disease characterized by high levels of sugar (glucose) in the blood.
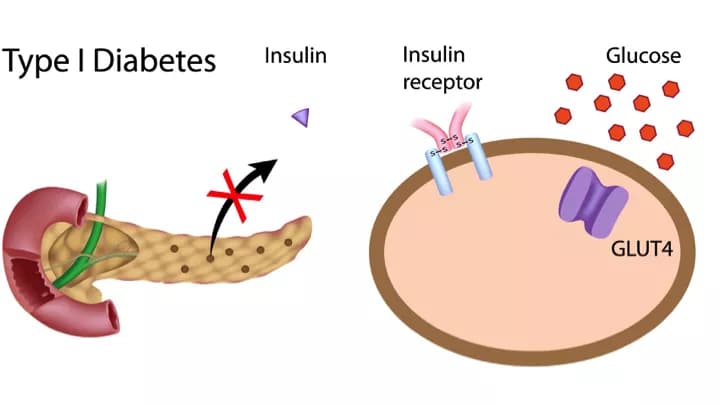
- With Type 1 Diabetes, the pancreas produces little or no insulin, a hormone necessary for sugar (glucose) to enter cells (where it is stored for later energy use).
- There is no cure for this disorder; however, it can be managed with proper treatment.
Who gets Type 1 Diabetes? (Age and Sex Distribution)
- Type 1 Diabetes can occur at any age in both males and females. However, it is most often diagnosed in children, adolescents, or young adults.
- All races and ethnic groups are affected by this condition.
What are the Risk Factors for Type 1 Diabetes? (Predisposing Factors)
Following are the risk factors for Type 1 Diabetes:
- Genetics: The incidence of certain genes indicates a higher risk for the development of Type 1 Diabetes
- Age: Children, adolescents, and young adults, are more likely to develop the condition
- Family history: Having a parent or sibling with Type 1 Diabetes increases an individual’s risk of developing the condition
- Geography: The incidence of Type 1 Diabetes is seen to increase as an individual travels away from the equator
- Viral exposure: Exposure to Epstein-Barr virus, Coxsackievirus, mumps virus, or cytomegalovirus, can trigger an autoimmune destruction of the islet cells, or directly infect them
- “Early vitamin D”: Early (when the child is very young) drinking of cow’s milk has been linked to an increased risk
- Dietary factors: Drinking water containing nitrates may increase risk. The timing of the introduction of cereal into a baby’s diet is seen to contribute to the risk
- Children, whose mothers were younger than 25 years, when they were born
- Having a mother who had preeclampsia during pregnancy
- Being born with jaundice
- Having a respiratory infection following birth
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Type 1 Diabetes? (Etiology)
- The exact cause of Type 1 Diabetes remains unknown. It is suspected to be an autoimmune disorder. A trigger, such as an infection, may cause the body to inaccurately attack pancreatic cells that produce insulin.
- Insulin, a hormone produced by beta cells in the pancreas, is necessary to move blood sugar into cells, where it is stored for later energy use. In Type 1 Diabetes, these beta cells produce little to no insulin.
- With a lack of insulin, glucose has the potential to build up in the bloodstream, instead of being redistributed to the cells. Without the body’s ability to utilize this glucose for energy, there is a build-up of glucose, which results in Type 1 Diabetes
What are the Signs and Symptoms of Type 1 Diabetes?
Several symptoms may be the first signs of Type 1 Diabetes, or they may occur with high blood sugar. These include:
- Extreme thirst
- Increased appetite
- Fatigue and lethargy
- Blurry eyesight
- Losing a sense of ‘feeling’ in feet, or tingling in feet
- Losing weight
- Frequent urination
- Sudden vision changes
- Heavy, labored breathing
Other individuals may experience the following warning symptoms as the first indications of Type 1 Diabetes, or which may occur when the blood sugar is very high (diabetic ketoacidosis):
- Deep and rapid breathing
- Dry skin
- Dry mouth
- Flushing in the face
- Fruity breath odor
- Nausea or vomiting
- Stomach pain
- Stupor, unconsciousness
Low blood sugar (hypoglycemia) can develop in individuals with Diabetes who are administered insulin. These symptoms appear most often when the blood sugar levels drop below 70 mg/dL:
- Headache
- Hunger
- Nervousness
- Rapid heartbeat
- Shaking
- Sweating
- Weakness
How is Type 1 Diabetes Diagnosed?
Type 1 Diabetes is diagnosed with the following blood tests:
- Fasting blood glucose level: If higher than 126 mg/dL, two times
- Random (non-fasting) blood glucose level: Higher than 200 mg/dL in conjunction with symptoms, such as increased thirst, urination, and fatigue, is indicative of Type 1 Diabetes
- Oral glucose tolerance test: If the glucose level exceeds 200 mg/dL after 2 hours
Hemoglobin A1c test, with values as noted below:
- Normal: Below 5.7%
- Pre-diabetes: Between 5.7% and 6.4%
- Diabetes: 6.5% or above
Other methods of testing include ketone testing, which is done using a urine or blood sample. Ketone testing can be performed:
- When blood sugar exceeds 240 mg/dL
- During illness, such as pneumonia, heart attack, or stroke
- When nausea or vomiting occur
- During pregnancy
A physician can perform several examinations in order to monitor the state of Diabetes and prevent medical issues associated with Diabetes, such as the following:
- Check the skin and bones on the feet and legs; check the feet to see if they are becoming numb.
- Check blood pressure at least annually, which should be 130/80 mm/Hg or below.
- Have hemoglobin A1c test (HbA1c) completed bi-yearly, if diabetes is well-controlled, or otherwise every three months
- Have cholesterol and triglyceride levels checked annually; a desirable level for LDL cholesterol levels is below 70-100 mg/dL.
- Have yearly tests to examine kidney function, which include micro-albuminuria and serum creatinine.
- Have eyes checked at least annually for signs of diabetic eye disease.
- Visit a dentist bi-yearly, for a thorough dental exam and cleaning.
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Type 1 Diabetes?
After several years, Diabetes can lead to serious complications, such as:
- Eye problems, which include lessened eyesight, particularly at night, and sensitivity to light. Diabetic retinopathy, a condition in which blood vessels of the retina are damaged, is caused by Type 1 Diabetes. This condition could potentially cause blindness. Type 1 Diabetes also increases the risk for other vision disorders, such as cataracts and glaucoma.
- Nerve damage, also known as neuropathy, is a common complication with Type 1 Diabetes. Excess sugar builds up in the blood vessels causing pain, tingling, and loss of feeling to the affected limbs.
- Nerve damage in the feet increases the risk of certain food complications. Feet and skin can acquire sores and infections, causing pain and itching. In severe cases, the foot or leg may need to be removed.
- Nerve damage can cause weakness or problems with urination. It may also make it more difficult for men to have an erection.
- Diabetes makes it difficult for one to control their blood pressure and cholesterol, leading to possible heart attacks, stroke, and other complications.
- Elevated blood sugar has the potential to lead to kidney damage, also known as nephropathy. It can damage the filtering system of the kidneys, leading to kidney failure or kidney disease.
- An individual may be more susceptible to bacterial and fungal infections of the skin.
- Diabetes may cause one’s bone mineral density to lower, increasing the risk for developing osteoporosis.
- Pregnancy complications: Elevated blood sugar levels can be threatening for both the baby and the mother. Risk of miscarriage, stillbirth, and birth defects is heightened when diabetes is not well controlled.
- Type 1 Diabetes may cause an individual’s hearing to become impaired.
- When an individual has Diabetes, their risk of heart attack is equivalent to an individual who has already experienced a heart attack. Both women and men with Diabetes are at equal risk.
How is Type 1 Diabetes Treated?
- Due to the quick onset and possible severe symptoms of Type 1 Diabetes, individuals who are initially diagnosed with the condition may need to stay in the hospital for further evaluation/treatment.
- It is recommended that after diagnosis, an individual should have a check-up each week until a steady control of blood sugar is established. Physicians routinely suggest home blood sugar monitoring and urine testing.
Any individual with Type 1 Diabetes should be aware of the following ways to help manage their diabetic condition:
- How to identify and treat low blood sugar (or hypoglycemia)
- How to identify and treat high blood sugar (or hyperglycemia)
- Meal planning for diabetes
- Insulin administration
- How to test blood glucose and urine ketones
- How to alter amounts of insulin through food and exercises
- How to deal with sick days
- Where to purchase diabetes (medical) equipment and their proper storage and handling
Insulin-related:
- Insulin lowers blood sugar by permitting it to leave the bloodstream and enter the cells of the body. Insulin must be administered every day in Type 1 Diabetes patients. Insulin shots may be necessary, between one to four times a day.
- Insulin is often injected under the skin. In other cases, a pump can deliver insulin all the time.
- Various insulin types are available, which differ in how fast-acting they are, and their duration of action in the body. Types of insulin include rapid-acting insulin, long-acting insulin, and intermediate options.
- Your physician will determine the correct/best type of insulin for you, and the time that is best suited for its administration. More than one type of insulin can be combined for the most optimal blood glucose control.
Diet and exercise:
- Individuals with Diabetes should eat similar foods at relativity the same time each day, which helps in maintaining the proper blood sugar level.
- The American Diabetes Association and the American Dietetic Association provide information on how to plan healthy meals.
- Constant and consistent exercising is recommended to control blood sugar, as well as burn extra calories and fat, in order to maintain a healthy weight.
- A doctor may prescribe pramlintide (Symlin), which is injected before a meal to slow the movement of food through the stomach. This helps curb the sharp upsurge in blood sugar levels following meals.
Oral medications:
- High blood pressure medications: A physician may prescribe angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs). These medications help keep the kidneys in good condition.
- Aspirin: Aspirin may be recommended daily (by a physician) to protect one’s health.
- Cholesterol-lowering drugs: Cholesterol guidelines are stricter for individuals suffering from Diabetes, due to the elevated risk of heart disease. A physician may not choose to wait until a diabetic patient has elevated cholesterol, before prescribing cholesterol-lowering agents (statins).
Blood sugar management:
- Monitoring blood sugar levels at home and keeping a record of the results is indicative of how an individual is managing Type 1 Diabetes. A physician will provide information on how frequently one should check their blood glucose levels.
- A glucometer device can be used to read blood sugar levels. In most cases, a small droplet of blood is produced by pricking ones finger with a small needle or lancet, which is then placed on a test strip, which is transferred to the device. Most results are recorded in 30-45 seconds.
- Physicians recommend keeping a record of blood sugar levels. A target goal for blood sugar levels should be set at different times throughout the day. A plan should be set in place for what to do when blood sugar exceeds or drops below normal levels.
Foot care:
Diabetes damages the nerves and blood vessels, making it difficult to feel pressure on one's feet. Often, a foot injury may go unnoticed until a severe infection sets in. Small sores in the skin may develop into deeper skin sores or ulcers. If the ulcers do not heal or become significantly larger, the affected limb may need to be amputated.
In order to prevent problems of the foot, one should:
- Stop smoking
- Improve regulation of blood sugar
- Get semi-annual foot exams
- Check feet each day, especially if there is a known episode of nerve or blood vessel damage
- Wear proper shoes
How can Type 1 Diabetes be Prevented?
- There are currently no known preventive measures for Type 1 Diabetes. There is also no screening exam for the condition, in individuals who do not exhibit any symptoms.
- Once diagnosed, an individual with Type 1 Diabetes can manage the condition by exercising regularly and eating healthy foods. Foods should be low in fat and calories, with an emphasis on fruits, vegetables, and whole grains.
- One should aim to exercise for about 30 minutes a day. In doing so, blood glucose levels can be normalized, thereby reducing the varied medical issues and complications associated with Type 1 Diabetes.
What is the Prognosis of Type 1 Diabetes? (Outcomes/Resolutions)
- Type 1 Diabetes lasts throughout an individual’s lifetime and no cure exists currently.
- The outcome for patients with Diabetes varies from one individual to another and is dependent upon many factors and health issues.
- With constant control and maintenance of blood glucose levels, one can prevent or delay the onset of problems, which may affect the eyes, kidneys, nervous system, and heart.
Additional and Relevant Useful Information for Type 1 Diabetes:
Omega-3 fatty acids may possibly offer some protection against Type 1 Diabetes.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.