What are the other Names for this Condition? (Also known as/Synonyms)
- Body Tinea Infection
- Fungal Infection - Body
- Ringworm Infection of the Body
What is Tinea Corporis Infection? (Definition/Background Information)
- Tinea Corporis Infection (or Ringworm Infection of the Body) is a fungal infection that affects the body skin surface, especially the arms and legs
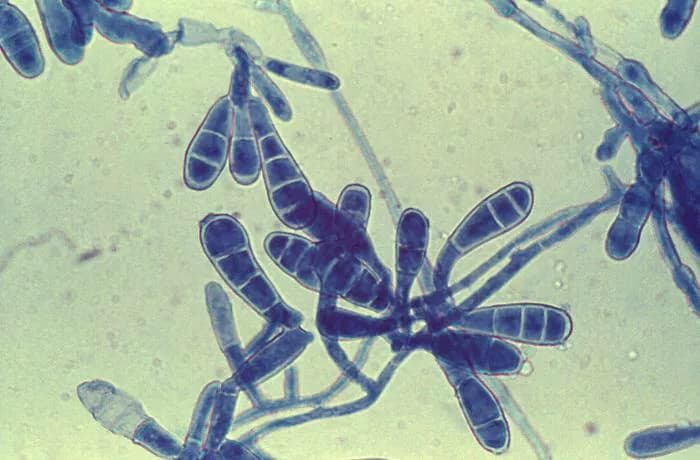
- The group of fungus causing the infection of skin are called dermatophytes (specifically belonging to the genus Trichophyton, Microsporum, or Epidermophyton)
- The infection causes itching sensations that are felt on the skin, with the appearance of small, round, and elevated red rashes (giving a ring-like form), with scaly textured surface
- This highly contagious fungal infection develops, due to poor hygiene and prolonged periods of warm moist conditions. It can affect any individual and is common throughout the world (both in urban and rural areas), spreading mostly through contact
- The condition is treated using antifungal medications and by maintaining proper hygiene
Who gets Tinea Corporis Infection? (Age and Sex Distribution)
- Tinea Corporis Infection may infect individuals of any age, gender, race, or ethnicity, if factors for fungus growth on the body are favorable
- It is more commonly seen in children, mainly those in their pre-adolescent stage
- Women, those who have a higher degree of contact and interaction with children (who are infected), have a higher risk for infection
- Individuals, working in close contact with children by virtue of their profession or work, are more prone to contracting Tinea Corporis Infection
What are the Risk Factors for Tinea Corporis Infection? (Predisposing Factors)
The potential risk factors for Tinea Corporis Infection include:
- Children, who are exposed to other infected children, particularly at schools, daycare centers for children, theme parks, play areas, etc.
- Playing contact sports, such as football, basketball, judo, or participating in any such activities that brings one in direct physical contact with other infected individuals
- Individuals residing in overcrowded neighborhoods (that are warm and humid) with poor living conditions
- Those with sweaty (wet) body conditions
- Individuals having superficial (on the surface) and minor skin or nail injuries
- Wearing tightfitting clothes regularly, particularly made of synthetic materials
- Sharing bathrooms, toilets, kitchen sinks
- Sharing contaminated items, like clothes, beds, linens, towels
- Playing with infected pets, coming into close contact with farm animals
- Neglecting fungal infection at other locations of the body
- If the individual has a weak immune system or diabetes, there is a greater susceptibility to fungal infections such as Tinea Corporis Infection
- Those, who were infected with fungal infections in the past, have an elevated risk
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Tinea Corporis Infection? (Etiology)
Tinea Corporis Infection (or Ringworm Infection of the Body) is caused by a fungus.
- Normally, there is fungus present in healthy individuals. The fungus is present in the dead skin cells that cover the body. A dry and clean skin does not allow the growth of the fungus. However, damp and warm conditions increase their growth and proliferation, which results in an infection
- Mold-like fungi, belonging to any of the genus Trichophyton, Microsporum, or Epidermophyton transmitted in wet, warm areas causes this body infection
- Tinea Infection of the Body spreads through:
- Direct contact with an infected individual
- An infected pet or other infected animals
- By using shared items
- In rare cases, from highly infected soils too
What are the Signs and Symptoms of Tinea Corporis Infection?
Tinea Corporis Infection signs and symptoms include:
- The fungus typically affects the epidermis (outer skin surface) causing circular ring-like rashes that appear normal and healthy, inside the circles; hence, the term ringworm infection
- These occur at various locations on the body, such as the trunk, arms, and legs
- When the affected area has hair, the hair shafts themselves can be infected. This leads to small papules and pustules at the skin surface. The hairs become weakened by the fungal organisms digesting them, and these then break off at the surface.
- Skin lesions have burning or itchy sensations. The enlarging red and inflamed skin rings project out of the surface and may form to become fluid-filled lesions
- Sometimes, there is excessive redness accompanied by fever
- With time, the skin appears flaky and dry with hair loss
- The incubation period for the symptoms to develop after an infection, may be from anywhere between 7-21 days
Often, infections caused through the soil or animal-route has a severe or higher degree of signs and symptoms.
How is Tinea Corporis Infection Diagnosed?
A Tinea Corporis Infection is visually recognizable, due to its characteristic annular (ring-like) formations on the skin. The physician may conclude the diagnosis based on a simple physical examination of the condition. However, the infection is normally confirmed by the following diagnostic tests:
- Performing a biopsy of the affected skin
- Potassium hydroxide test (KOH test): A sample of the skin scraping is examined microscopically, to detect the presence of fungus
- A fungus culture may be performed - however, it may take weeks to obtain the results
- A differential diagnosis may need to be considered in order to eliminate other skin infections/conditions
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Tinea Corporis Infection?
Complication due to Tinea Corporis Infections may include:
- The infection may spread to other regions, like the groin, scalp, feet, etc.
- Permanent scars and patches may be caused, due to a worsening of the skin condition. This may lead to intensely painful inflammation, drainage of the lesions, etc.
- Recurrence of the infection
- Risk of other opportunistic skin disorders, or other bacterial infections affecting the body, like cellulitis, pyoderma
- The lymph nodes may become infected by bacteria leading to conditions, like lymphadenitis or lymphangitis
- Side effects of the (oral) medications used
How is Tinea Corporis Infection Treated?
The treatment measures for Tinea Corporis Infection include:
Most skin-related fungal infections respond extremely well to treatment, with over-the-counter antifungal medications and dry powder applications
- Oral medications are necessary, if topical medications do not relieve the symptoms, or if the infection is quite severe. The common, inexpensive, and trusted oral medication most commonly recommended is terbinafine. All antifungal drugs may have some side effects, and hence, they are prescribed with caution. Most are well tolerated in the short courses that work in tinea corporis
- Self-care is essential, which also helps shorten the recovery period. Certain basic steps to be followed include:
- Regular washing and cleaning of the skin surface to prevent spread of the infection to other regions
- Using clean and disinfected towels, combs, and hairbrushes
- Disinfecting common shared spaces, such as toilets and shower areas, bathtubs, kitchens, bedrooms
- Applying the prescribed creams and taking the prescribed oral medications regularly
- If bacterial infections complicate the condition, then antibiotics are prescribed
- In order to avoid recurrence of the infection, the antifungal treatment measures have to be continued for an extended period of time (per advice of the physician); even after the condition has been controlled
How can Tinea Corporis Infection be Prevented?
Some basic steps to ensure the prevention of Tinea Corporis Infection, especially if the risk factors are high, include:
- Keep the body (especially the groin region, armpits), clean and dry regularly. It is also important to ensure that individual’s habitually wash their hands
- Avoid wearing tightfitting, thick clothing and dress made of synthetic material, which might induce excess sweating (for longer time periods), unless there is a real necessity
- Areas frequented by children/adults (or common spaces used by them), have to be maintained in good, sanitary, and hygienic condition
- Fungal infections transmit through contact and hence, avoid sharing common personal items, like combs, towels, beddings, etc.
- Tinea Corporis Infection can spread from infected animals and pets. Such animals may show signs of hairless skin patches on their body, or sometimes they may be asymptomatic
- Always clean yourself up after walking or working in fields and on farmlands. Also, clean up after performing any activity that involves touching the soil, like gardening, watering plants, outdoor camping, etc.
- Treat any fungal infection immediately, and prevent them from spreading to other regions of the body
- Teach the children or keep them informed about fungal infections and tell them how to recognize certain early signs
What is the Prognosis of Tinea Corporis Infection? (Outcomes/Resolutions)
The prognosis of Tinea Corporis Infection with appropriate treatment is excellent.
- Irrespective of the severity of the infection and active treatment measures followed, Ringworm Infection of the Body may last for a few months, but results in a complete cure
- It responds very well to antifungal treatment and good self-care
- In order to prevent its recurrence, the treatment has to be continued for a few weeks, even after all the signs of infection have ceased
- If the infection spreads to other parts of the body (scalp, feet), or other secondary bacterial infections arise, then an extended course of treatment with antibiotics may be required
Additional and Relevant Useful Information for Tinea Corporis Infection:
- Individuals with diabetes or other immunodeficiency-related diseases should seek immediate medical advice, if they develop Tinea Corporis or other locations of fungal Infection
- If any one individual member in a family contracts the disease, then the risk of transmission to other members in the house is high. Hence, every precaution has to be taken to maintain a hygienic environment
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.