What are the other Names for this Condition? (Also known as/Synonyms)
- Acute Febrile Neutrophilic Dermatosis
- Drug-Induced Sweet’s Syndrome
- Sweet Syndrome
What is Sweet’s Syndrome? (Definition/Background Information)
- Sweet’s Syndrome is a rare, benign skin disease, with a sudden onset of fever and painful red, inflamed skin lesions, infiltrated by neutrophils (a type of white blood cell)
- There are 3 main groupings of Sweet’s Syndrome:
- Classical or Idiopathic Sweet’s Syndrome
- Malignancy-Associated Sweet’s Syndrome
- Drug-Induced Sweet’s Syndrome
- The cause of classical/idiopathic and malignancy-associated types of Sweet’s Syndrome is unknown, while there are a variety of medications that are associated with the drug-induced type
- This skin condition is usually treated with steroids and medications. The prognosis of Sweet’s Syndrome is usually excellent with appropriate treatment
Who gets Sweet’s Syndrome? (Age and Sex Distribution)
Idiopathic Sweet’s Syndrome:
- The syndrome is usually present in adults between the ages 30-60 years
- Women are more likely to develop the condition, than men (in a 4:1 ratio)
- Idiopathic Sweet’s Syndrome recurs in one-third of the patients
Malignancy-Associated Sweet’s Syndrome:
- The skin findings may signal cancer recurrence or an undiagnosed cancer
- It is seen with equal incidence in men and women
Drug-Induced Sweet’s Syndrome:
- Individuals, who are exposed to certain drugs that may cause the syndrome
- Both males and females of all ages are equally affected
What are the Risk Factors for Sweet’s Syndrome? (Predisposing Factors)
The risk factors of Sweet’s Syndrome include:
- Being female, between the ages of 30-60 years, and previously having Idiopathic Sweet’s Syndrome are risk factors to developing an episode
- Malignancy-Associated Sweet’s Syndrome is often associated with solid cancers or cancers of the blood (usually acute myeloblastic leukemia)
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Sweet’s Syndrome? (Etiology)
- The cause of Idiopathic Sweet’s Syndrome and Malignancy-Associated Sweet’s Syndrome is unknown
- The drugs associated with Drug-Induced Sweet’s Syndrome include the following anticancer drugs:
- Granulocyte colony-stimulating factor (G-CSF): It is most commonly associated with the condition
- Bortezomib
- Azacitidine
- Decitabine
- Imatinib mesylate
- Lenalidomide
- All-trans retinoic acid (ATRA)
What are the Signs and Symptoms of Sweet’s Syndrome?
Signs and symptoms of Sweet’s Syndrome include:
- Fever (that may be high or moderate), tiredness, headache, aches in the joints, skin sores
- Idiopathic Sweet’s Syndrome is characterized by the rapid onset of painful, red, inflamed skin lesions, infiltrated by neutrophils (a type of white blood cell), without inflammation of blood vessels
- 75-90% of patients with Idiopathic Sweet’s Syndrome report an upper respiratory infection prior to the presentation of Sweet’s Syndrome, while only 20% of patients with Malignancy-Associated Sweet’s Syndrome report such an infection
How is Sweet’s Syndrome Diagnosed?
Presence of both the major criteria and four of the minor criteria (below) must be present, to diagnose the condition:
- Sweet’s Syndrome is associated with the following major criteria:
- Rapid onset of painful skin lesions (papules, nodules, and plaques) that are red and inflamed
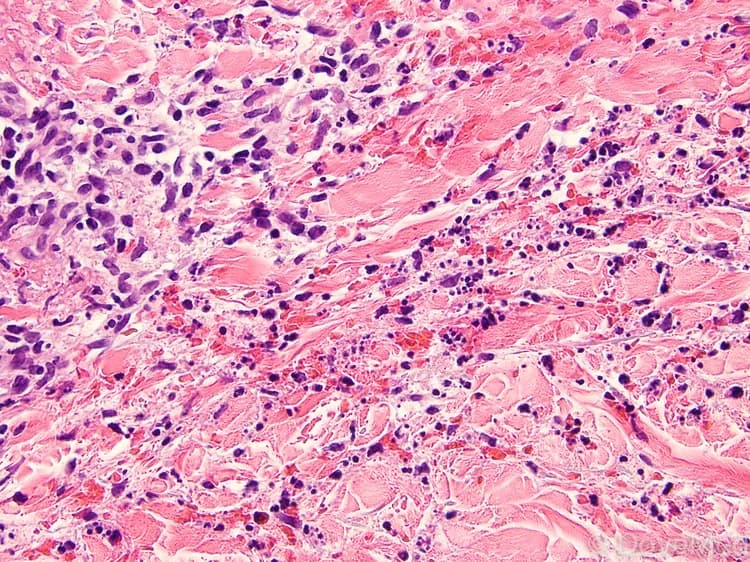
- Skin biopsy shows histopathologic features of neutrophilic (a type of white blood cell) infiltration, without inflammation of blood vessels caused by white blood cell destruction, that is usually present in the upper dermis skin layer
- Sweet’s Syndrome is associated with the following minor criteria:
- Fever (>38° C, or 100.4° F)
- Prior upper gastrointestinal infection
- Presence of tumor, inflammatory disorders, or pregnancy
- Response to corticosteroid or potassium iodide treatment
- Elevated white blood cell count (leukocytosis)
- Elevated sedimentation rate (ESR)
- Elevated neutrophils in peripheral blood
- High C-reactive protein
To diagnose Drug-Induced Sweet’s Syndrome, the above criteria must be met, as well as a temporal relationship established between drug-ingestion and the clinical features observed; with a temporal resolution, after drug withdrawal or on treatment.
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Sweet’s Syndrome?
The possible complications of Sweet’s Syndrome include:
- Sweet’s Syndrome can lead to recurring episodes of the described inflammatory skin lesions. There is a risk that the skin lesions may become infected
- Some of the skin lesions may occur in other parts of the body, including the ears, eyes, heart, and lung, and may have organ-specific complications
- Anemia is seen to commonly occur in patients with Malignancy-Associated Sweet’s Syndrome and Drug-Induced Sweet’s Syndrome
How is Sweet’s Syndrome Treated?
A treatment of Sweet’s Syndrome may involve the following:
- Sweet’s Syndrome is often treated by 4-6 weeks of intravenous, oral, or topical corticosteroids, depending on the extensiveness of the skin findings. The length of treatment depends on the condition and may vary
- Other medications prescribed may include potassium iodide, colchicine, dapsone, and cyclosporine
- In Malignancy-Associated Sweet’s Syndrome, the treatment of the underlying malignancy may treat the disease
- In Drug-Induced Sweet’s Syndrome, stopping or temporary discontinuation of the causative drug may treat the disease
- Antibiotics may be necessary, if the skin lesions are large and if skin infection is observed
How can Sweet’s Syndrome be Prevented?
- Idiopathic Sweet’s Syndrome and Malignancy-Associated Sweet’s Syndrome are complex conditions with no particular preventative measures, at this time
- Drug-Induced Sweet’s Syndrome can be prevented by avoiding the drugs (if possible) that may cause the disease
What is the Prognosis of Sweet’s Syndrome? (Outcomes/Resolutions)
- Treatment with the medications often leads to resolution of the symptoms of Sweet’s Syndrome, but recurring episodes may occur
- The prognosis of Sweet’s Syndrome is usually excellent
Additional and Relevant Useful Information for Sweet’s Syndrome:
- Sweet’s Syndrome was first described by Robert Douglas Sweet in 1964
- Dr. Sweet originally named the disease ‘Gomm-Button Disease’, in honor of his first two patients with the disease. But, ‘Sweet’s Syndrome’ became the commonly known name of the condition
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.