What are the other Names for this Condition? (Also known as/Synonyms)
- Bradycardia-Tachycardia Syndrome due to Sick Sinus Syndrome
- Sinus Node Dysfunction
- SSS (Sick Sinus Syndrome
What is Sick Sinus Syndrome? (Definition/Background Information)
- Sick Sinus Syndrome (SSS) is a term used to refer to a group of abnormal heart rhythm disorders, which are mainly characterized by malfunctioning of the sinus node. The sinus node is the natural pacemaker situated in the heart and it controls the rhythm of the heart
- Sick Sinus Syndrome may manifest in multiple ways including:
- Sinus bradycardia, which causes slowed heart rate
- Sinus pauses or arrest: In this condition the pacemaker of the heart stops working for a certain period of time
- Sinus tachycardia causing a faster heart rate
- Bradycardia-tachycardia: The heart rate alternatively decreases and then increases or vice versa
- Although there is no racial or ethnic group bias for this condition, Sick Sinus Syndrome is reported to be more prevalent in countries where people have long life expectancies. Thus, typically, individuals over the age of 70 years, are found to be more prone to Sick Sinus Syndrome
- Advanced age, certain medications for heart conditions, and having already had a heart attack are some known risk factors for this condition. Scarring and degeneration in the electrical system of the heart is the most common cause of Sick Sinus Syndrome
- The common signs and symptoms associated with Sick Sinus Syndrome include light-headedness, confusion, and palpitations. SSS may cause complications including fainting spells, intolerance to physical exertion, and even heart failure
- The implantation of a permanent pacemaker is the most effective treatment measure for Sick Sinus Syndrome with slowed heart rate. The disease is progressive in nature, but individuals with implanted permanent pacemakers have a generally good prognosis
Who gets Sick Sinus Syndrome? (Age and Sex Distribution)
- Sick Sinus Syndrome can occur at any age, but individuals above the age of 70 are generally more susceptible to this condition
- There is no gender, racial, or ethnicity predilection reported for this condition
- However, SSS is more prevalent in certain regions/countries of the world where individuals have longer life expectancies
What are the Risk Factors for Sick Sinus Syndrome? (Predisposing Factors)
The risk factors associated with Sick Sinus Syndrome include:
- Advancing age: The risk for Sick Sinus Syndrome increases with advancing age
- Previous heart attack/myocardial infarction
- Certain medications, used for blood pressure control and other heart diseases, which may suppress the function of the sinus node
- Hyperkalemia - a condition in which there is too much potassium in blood
- Thyroid disease
- Sleep apnea syndrome often associated with snoring and sleeping abnormalities
- Previous heart surgery
- Certain underlying medical conditions, such as muscular dystrophy, and other disorders that can have an impact on the functioning of the heart
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Sick Sinus Syndrome? (Etiology)
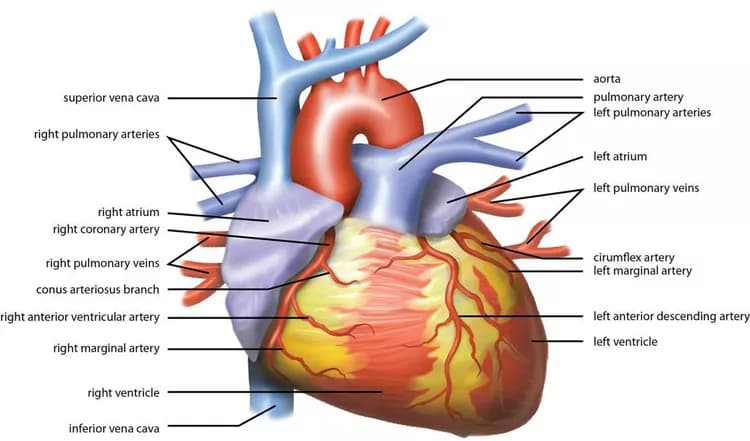
The heart is made of two upper chambers (atria) and two lower chambers (ventricles). The sinus node or the sinoatrial node, which controls the rhythm of the heart through the production of electrical impulses is located in the upper and outward portion of the right atrium. Electrical impulses are generated automatically in the sinus node, and these impulses travel from the sinus node to the atria and then to the ventricles. These impulses cause the heart muscles to contract and pump blood to the lungs and the entire body.
- When this sinus node malfunctions, it does not work properly, and the condition is called Sick Sinus Syndrome. Due to this, the heart rate is either too fast, too slow, or irregular
- Major causes that may lead to malfunction of the sinus node and consequently to Sick Sinus Syndrome include:
- Diseases that can damage the heart’s electrical system
- Scar tissues created as a result of previous heart surgeries or injury
- Use of medications such as calcium channel blockers, beta blockers, digitalis, and antiarrhythmics
- Wear and tear of the heart muscle electrical system resulting from old age (degeneration of the conduction system)
What are the Signs and Symptoms of Sick Sinus Syndrome?
The signs and symptoms of Sick Sinus Syndrome may include:
- Angina or chest pain
- Changes in the mental status, confusion
- Headache, nausea, and dizziness
- Fatigue
- Palpitations
- Shortness of breath
How is Sick Sinus Syndrome Diagnosed?
The diagnosis of Sick Sinus Syndrome may involve the following exams and procedures:
- Complete evaluation of medical history and a thorough physical examination
- Electrocardiogram to reveal any abnormality in the heartbeat and heart rhythm
- Holter monitoring to ascertain a slow heart rate, long pauses, and also atrial tachycardia. This device is carried on the patient, and it typically monitors the heart activity for a period of 24-48 hours
- Intracardiac electrophysiology study (EPS), in which catheters are introduced into the heart for an invasive study of the heart’s conduction system, is another method for diagnosing Sick Sinus Syndrome and may be used to complement the diagnostic modalities mentioned above
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Sick Sinus Syndrome?
Some possible complications associated with Sick Sinus Syndrome include:
- Exercise intolerance: Inability of an individual to tolerate cardiovascular exercises
- Syncope or fainting
- Fall injuries caused by fainting
- The pumping of the heart may become really slow and poor, resulting in inadequate blood supply to meet the demands of the body leading to heart failure (cardiac failure)
How is Sick Sinus Syndrome Treated?
Generally, no treatment is necessary for Sick Sinus Syndrome if no symptoms are observed. In case of any signs and symptoms, the following measures may be considered:
- A healthcare provider will review the current medications one is taking and evaluate if these medicines are responsible for the heart abnormality
- Permanent pacemakers may be implanted in individuals with bradycardia (slowed heart rate)
- Antiarrhythmic medications may be prescribed to control fast heart rates
- A surgical procedure called radiofrequency ablation may be recommended to treat tachycardia
How can Sick Sinus Syndrome be Prevented?
In a majority of cases, Sick Sinus Syndrome is not preventable. However, in order to have a healthy heart, one may consider the following steps:
- Eat a well-balanced diet
- Exercise regularly
- Avoid medications/drugs that may potentially cause the heart condition to deteriorate (after consultation with a healthcare provider)
What is the Prognosis of Sick Sinus Syndrome? (Outcomes/Resolutions)
Sick Sinus Syndrome is a progressive disease which worsens with the passage of time.
- Nevertheless, the prognosis is good with appropriate treatment in a majority of individuals
- Good outcomes have been reported in patients with permanently implanted pacemakers
Additional and Relevant Useful Information for Sick Sinus Syndrome:
- Pacemaker implantation is a procedure that involves temporarily or permanently placing a pacemaker within the chest wall, and in some cases, directly in the heart
The following article link will help you understand pacemaker implantation surgical procedure:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.