What are the other Names for this Condition? (Also known as/Synonyms)
- Medial Tibial Stress Syndrome (MTSS)
- MTSS (Medial Tibial Stress Syndrome)
What are Shin Splints? (Definition/Background Information)
- Shin Splints are common injuries that refer to pain in the connective tissue along or behind the shinbone (or tibia). It may occur on the inside of the leg (called Medial Shin Splints) or outside of the leg (called Anterior Shin Splints)
- Shin Splints are usually caused by any physical activity, such as an athletic sport, which results in repetitive stress on the shinbone and connective tissue that attaches the muscle to the bone
- Overall, there is a high rate of incidence of this condition among young athletes and sportspersons
- Rest, ice, and stretching are usually recommended measures to treat Shin Splints. However, surgery is an option, in rare cases, when an individual does not respond to nonsurgical treatment methods
- The prognosis of Shin Splints is usually excellent with appropriate treatment
Who gets Shin Splints? (Age and Sex Distribution)
- Shin Splints may occur in individuals of all ages, races, ethnic groups, and genders
- However, it is more commonly observed in women than men
- Overall, this condition predominately occurs in individuals who participate in sports activities that require repetitive stress on the shinbone and connective tissue, such as during running
What are the Risk Factors for Shin Splints? (Predisposing Factors)
Some of the common risk factors for Shin Splints include:
- Participating in certain sports such as track and field events
- Any sport that involves a lot of jumping such as basketball, gymnastics
- The presence of physical abnormalities or defects such as flat feet
- Individuals with a high-arched foot
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Shin Splints? (Etiology)
Currently, the underlying cause of Shin Splints is unknown. However, researchers believe Shin Splints develop when the muscle and bone tissue (periosteum) in the leg are overworked due to repetitive physical activity.
Additional causes of Shin Splints may include:
- Participation in activities that require repetitive overuse of the shinbone such as running
- Individuals with flatfeet
- Structural abnormalities such as having a high-arched feet
- Muscle weakness or reduced flexibility of the quadriceps muscles
- Low bone mineral density
- Hormonal imbalances
- Exercising on hard surfaces such as concrete sidewalks or roads
- Exercising in poor quality or with ill-fitting shoes
- Improper training techniques
What are the Signs and Symptoms of Shin Splints?
The signs and symptoms of Shin Splints include:
- Pain and tenderness in the lower leg that occurs before or after exercising
- Swelling in the lower leg
How is Shin Splints Diagnosed?
Diagnostic methods that a physician may use to help diagnose Shin Splints include:
- Physical examination: Physicians can usually diagnose Shin Splints by thoroughly examining an individual’s leg. In addition to this, a complete medical history can aid in arriving at a definitive diagnosis
- X-ray of the foot: X-rays use radiation to produce images of the shin. It can also help the physician rule out other possible causes of shin pain such as fractures, tendinitis, and chronic exertional compartment syndrome
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Shin Splints?
Complications of Shin Splints may include:
- Stress may develop in the muscles and tendons of the foot. This can occur if the pain associated with Shin Splints forces an individual to walk by putting weight, on the outside of the foot
- Strain in the back due to abnormal gait
- The development of inflammation and arthritis of the surrounding joints, such as back, hip, knee, and ankle, due to changes in posture
- Permanent disability
How are Shin Splints Treated?
Shin Splints can usually be treated with nonsurgical interventions. However, in rare cases, surgery is an option when the individual is non-responsive to nonsurgical treatments.
Nonsurgical treatment for Shin Splints may include:
- Any activity that further aggravates the condition should be avoided. The physician usually recommends refraining from all such activities, until the symptoms improve
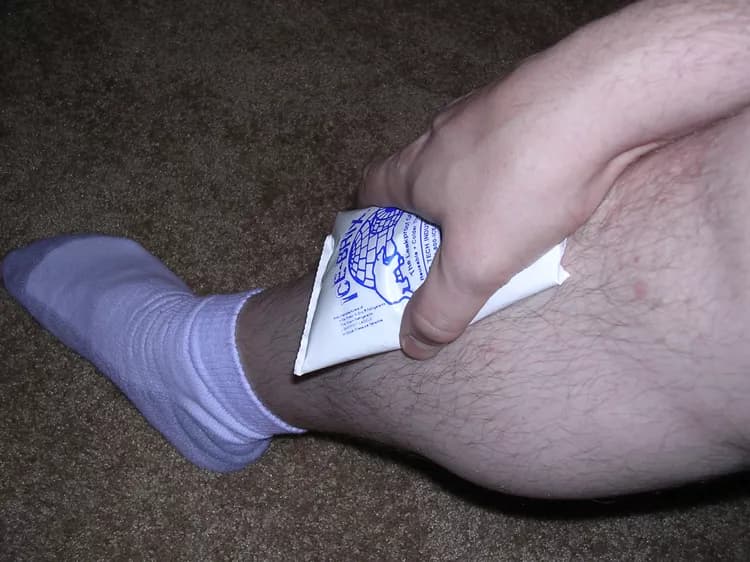
- Applying ice to the shinbone can help reduce pain and swelling
- Wearing an elastic compression bandage can help stop additional swelling and loss of blood
- Shoe orthotics may also be prescribed for individuals with flatfeet or recurring Shin Splints to help relieve pain. Shoe orthotics can help align and stabilize the foot and ankle, which takes the stresses off the lower leg
- Extracorporeal shock wave therapy (ESWT) is an increasingly popular (US FDA-approved) therapeutic approach in which high-energy sound waves are sent to the shin. However, this therapy is usually used for more severe cases that have not responded well to conservative treatment
- Physical therapy that includes flexibility exercises to stretch the lower leg muscles may help restore strength and decrease pain
If an individual does not respond to nonsurgical methods or, if multiple recurrences of Shin Splints occur, then surgical procedures, such as fasciotomy, may be required.
How can Shin Splints be Prevented?
Some of the common recommendations to help prevent Shin Splints include:
- Warming-up prior to exercising
- Correct stretching techniques are recommended before and after an athletic event
- Wearing appropriate footwear such as the proper shoe size
- Gradually increasing the intensity, frequency, and duration of workouts
- Maintaining strength in the calf muscles through exercise
- Adding cross-training to exercise regimen, such as swimming or cycling, which can decrease the impact on the shins
It is important to note that understanding the causal factors of Shin Splints is essential to helping prevent recurrence of the condition.
What is the Prognosis of Shin Splints? (Outcomes/Resolutions)
- The majority of individuals with Shin Splints are successfully treated without surgery. The long-term prognosis is usually good after treatment
- When properly treated, a high percentage of individuals regain their full strength and range of motion in their knees
- In rare cases, individuals may be permanently disabled, if they do not respond to conservative treatment and are not suitable candidates for surgical intervention too
Additional and Relevant Useful Information for Shin Splints:
- Shin Splints are the most common type of lower leg injury, accounting for approximately 60% of all overuse injuries to the leg
- The rate of Shin Splints in high school age runners is approximately 13%; in aerobic dancers it is approximately 22%; and in military personnel undergoing basic training it is between 4% to 8%
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.