Pulmonary Hypertension (PH)
What are the other Names for this Condition? (Also known as/Synonyms)
- Lung Hypertension
- PH (Pulmonary Hypertension)
What is Pulmonary Hypertension? (Definition/Background Information)
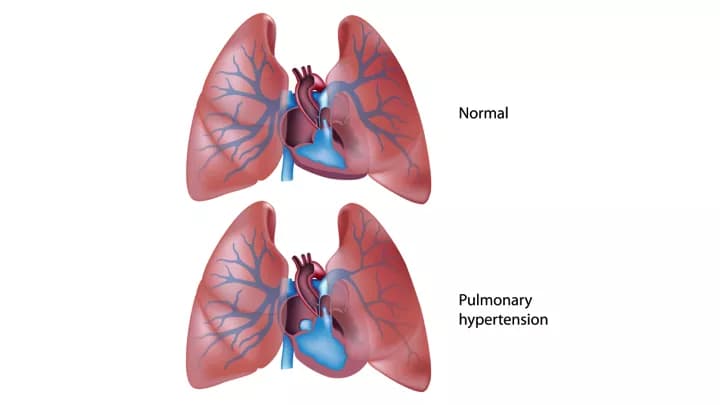
- Pulmonary Hypertension (PH) means a high blood pressure in the (main artery of the) lungs. This should not to be confused with systemic hypertension, otherwise known as ‘high blood pressure’
- Pulmonary Hypertension is a progressive disorder characterized by very high blood pressure (above normal) in the pulmonary arteries. The pulmonary blood vessels are usually a “low pressure” system
- This elevated pulmonary arterial pressure causes the right side of the heart to work harder, placing an increased burden on the heart
- Pulmonary Hypertension is often caused due to various lung and heart diseases; but, can sometimes result from a large number of chronic diseases, or even from direct diseases of the blood vessels
There are 5 types of Pulmonary Hypertension:
- Pulmonary Arterial Hypertension
- Pulmonary Hypertension due to left heart disease
- Pulmonary Hypertension due to chronic hypoxemic disease
- Pulmonary Hypertension due to embolic disease
- Pulmonary Hypertension due to miscellaneous causes
Who gets Pulmonary Hypertension? (Age and Sex Distribution)
- Pulmonary Hypertension is found among all age groups
- 6% of PH cases are familial, which means that there is a family history of the condition. The remainder of the cases (94% majority) are sporadic, meaning that it occurs without a family history of the condition
- Women are more susceptible to this disorder than men
- No special racial or geographical restriction is noted
What are the Risk Factors for Pulmonary Hypertension? (Predisposing Factors)
The risk factors for Pulmonary Hypertension include:
- Genetic factors (family history of Pulmonary Hypertension)
- Heart disease
- Chronic hypoxemic disease, such as COPD, chronic bronchitis, emphysema, etc.
- Embolic disease, where blood clots settle in the lungs, having originated in other parts of the body
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Pulmonary Hypertension? (Etiology)
Following are the possible cause factors for Pulmonary Hypertension:
- Alterations/changes (mutations) that occur in the BMPR2 gene, which is inherited in an autosomal dominant pattern
- Changes in the cells that line the lung arteries, which include:
- Tightening of the arterial walls, which increases the pressure as the blood flow through them
- Walls of the arteries are stiff by birth
- Or, the walls of the arteries stiffen due to an overgrowth of cells (endothelial proliferation). This causes a narrowing of the blood vessel (lumen) that in turn causes an increase in pressure, as the blood flows through them
- Clotting of blood in the arteries, causing narrowing of the blood vessel (lumen) that in turn causes an increase in pressure, as the blood flows through them
Due to the above changes it becomes difficult for the heart to pump blood through the blood vessels; hence, pressure builds up causing Pulmonary Hypertension.
What are the Signs and Symptoms of Pulmonary Hypertension?
The common signs and symptoms exhibited by individuals with Pulmonary Hypertension include:
- Progressive shortness of breath (especially while exercising), is the most common symptom
- Fatigue (frequent tiredness)
- Chest pain
- Dizziness, fainting
- Swelling of the ankles/legs
- Palpitations
- Bluish lips and skin, observed during the later stages
- Irregular heartbeat (arrhythmias)
- Fluid in the abdomen (ascites)
Note: Signs and symptoms of medical conditions associated with Pulmonary Hypertension are often present, and can help direct testing.
How is Pulmonary Hypertension Diagnosed?
Diagnostic procedures for Pulmonary Hypertension will involve:
- A complete physical examination of the patient
- A thorough checking of the patient’s medical history
- A detailed checking on the family history of the patient
- Echocardiography: An ultrasound of the heart is the ‘best’ initial test to assess for Pulmonary Hypertension
- Chest x-ray
- VQ scan (Lung ventilation/Perfusion scan), to look for chronic blood clots in the lungs
- CT scan of the chest
- EKG cardiac catheterization
- Oxygen saturation; at rest and with exertion (6 minute walk)
- A sleep study; if there is a possibility of sleep apnea
- Pulmonary function tests: A breathing test to check functioning of the lungs
- Blood tests to rule out other diseases like HIV, liver disease, rheumatoid arthritis
- Exercise testing: To measure the patient’s ability to exercise
- Consultation with a pulmonary or a cardiology specialist; when the initial evaluation does not diagnose a cause for the symptoms
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Pulmonary Hypertension?
Following are the possible complications that may arise due to Pulmonary Hypertension:
- Right-sided heart failure with hepatic congestion (due to deposition of stones in the liver)
- Pedal edema: Swelling of the leg or ankle
- Pleural effusions: Building-up of excess fluid around the lungs
- Worsening dyspnea (shortness of breath) upon exertion
How is Pulmonary Hypertension Treated?
Pulmonary Hypertension is a rare condition and is best treated at a center with appropriate expertise. An appropriate treatment depends on identifying the cause of the disorder; and the treatment is usually focused on the underlying condition.
- Treat underlying diseases or conditions such as lung disease, heart disease, HIV, chronic hypoxemia, connective tissue disease, chronic thromboembolic disease, and others.
- The appropriate treatment for one form of Pulmonary Hypertension may be unsafe/unsuitable with other forms of Pulmonary Hypertension
- Supplemental oxygen may help an individual meet the ‘oxygen needs’ for normal daily activities
- Diuretics, salt limitation, weight monitoring, blood thinners, calcium channel antagonists may be prescribed/advised by healthcare providers
- Lifestyle modifications are helpful (such as nutrition, exercise, avoiding tobacco, and limiting alcohol consumption)
- Other treatments, depending on the etiology (cause) of Pulmonary Hypertension, may include various cardiothoracic procedures
- Other medications that may be helpful in some forms of Pulmonary Hypertension includes prostacycline analogues, phosphodiesterasre-5 (PDE5) inhibitors, and endothelin antagonists
- Lung transplantation may be required with advanced forms of the disorder
- Judicious exercising may be effective in limiting deconditioning (by building stamina), improving the quality of life, and exercising capacities. Isometric exercises, such as heavy weight lifting should be avoided
How can Pulmonary Hypertension be Prevented?
- Early and effective treatment of disorders that can lead to Pulmonary Hypertension is imperative/absolutely necessary
- Avoidance of recreational drugs, various toxic agents, and inappropriate weight loss drugs is important
- Unlike systemic hypertension, screening for Pulmonary Hypertension is only recommended in those with a strong family history, in organ transplant protocols (lung), and in some conditions such as systemic sclerosis
What is the Prognosis of Pulmonary Hypertension? (Outcomes/Resolutions)
- Prognosis will differ depending on the severity and form of Pulmonary Hypertension. The disorder has no cure, but earlier and focused treatment can improve outcomes
- Pulmonary Hypertension is a negative prognostic sign in many medical conditions, meaning that the presence of Pulmonary Hypertension makes the overall health outcomes worse (such as COPD or heart failure)
- Prognosis is worse with advanced heart disease, a suboptimal 6 minute walk test, and with conditions, such as advanced liver disease and connective tissue disease
- According to CDC: “Prior to 1995, people with Pulmonary Hypertension lived on average less than 3 years after diagnosis. Now, new treatments have improved survival rates and quality of life for those living with this condition”
Additional and Relevant Useful Information for Pulmonary Hypertension:
- The historical terms “primary” and “secondary” hypertension are now discouraged
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.