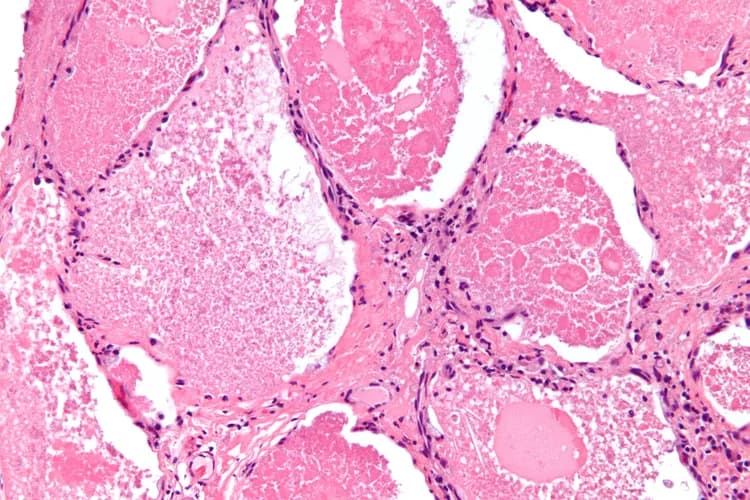
Pulmonary Alveolar Proteinosis
What are the other Names for this Condition? (Also known as/Synonyms)
- Alveolar Proteinosis
- PAP (Pulmonary Alveolar Proteinosis)
- Pulmonary Alveolar Phospholipoproteinosis
What is Pulmonary Alveolar Proteinosis? (Definition/Background Information)
- Pulmonary Alveolar Proteinosis (PAP) is a diffuse lung disease characterized by the deposition of a grainy substance (a type of protein and lipid) in the terminal air spaces of the lung
- The condition most commonly affects middle-aged males. The common signs and symptoms of Pulmonary Alveolar Proteinosis are cough, shortness of breath, fatigue, and fever. complications of the condition may include lung infections, lung fibrosis, and right-side heart failure
- In most cases, Pulmonary Alveolar Proteinosis is treated by whole-lung lavage (a bronchopulmonary procedure)
- There is no effective prevention of the condition, but the associated prognosis with suitable treatment is generally good
Who gets Pulmonary Alveolar Proteinosis? (Age and Sex Distribution)
- Pulmonary Alveolar Proteinosis affects both children (neonates) and adults; however, middle-aged adults are affected more commonly
- PAP more often affects males than females
What are the Risk Factors for Pulmonary Alveolar Proteinosis? (Predisposing Factors)
Risk factors associated with Pulmonary Alveolar Proteinosis include:
- Blood cancers
- HIV infection
- Infection with Nocardia organism
- Exposure to silica and aluminum dust
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Pulmonary Alveolar Proteinosis? (Etiology)
- In Pulmonary Alveolar Proteinosis, the alveoli are filled with a grainy substance that is composed of protein and phospholipid
- These same proteins and phospholipids are the key components of surfactants. A surfactant is a normal lung component that coats the alveoli and prevents a lung collapse
- In Pulmonary Alveolar Proteinosis, either there is an increased production of the surfactant or there is impaired removal of the surfactant by lung macrophages (lung cells)
There are 3 clinical forms of Pulmonary Alveolar Proteinosis (PAP):
- Primary (acquired or idiopathic) PAP is the most common form and is characterized by the increased production of antibodies, which target and neutralize GM-CSF (GM-CSF increases the effectiveness of alveolar macrophages)
- Secondary form of PAP is caused by another clinical condition that reduces the number or effectiveness of alveolar macrophages
- Congenital form of PAP is caused by a genetic defect that affects the production of normal surfactant
What are the Signs and Symptoms of Pulmonary Alveolar Proteinosis?
The signs and symptoms are general in nature and are mostly related to the lungs. The signs and symptoms associated with Pulmonary Alveolar Proteinosis may include:
- Cough
- Shortness of breath
- Fever
- Fatigue
- Weight loss
How is Pulmonary Alveolar Proteinosis Diagnosed?
Pulmonary Alveolar Proteinosis may be diagnosed through the following tests and procedures:
- Complete evaluation of medical history and thorough physical examination
- Blood tests: There may be increased levels of chemicals in blood such as SP-A, SP-D, or anti GM-CSF antibodies
- Chest x-ray: It is special image of the chest that reveals any abnormal lung opacity
- High resolution CT scan: This a special image of the chest using computers in which thin slices of chest cross sections are visible in high resolution (images are much better as compared to a simple x-ray)
- Sputum examination: In this exam, the changes generally observed are an increased protein called surfactant apo protein-A and the presence of cells that stain with a specific chemical called periodic acidic Schiff reagent
- Pulmonary function tests: In this test, the physician assesses the current status of lung function
- Bronchoalveolar lavage: It is a bronchoscopy procedure in which a thin tube is passed into the windpipe and lungs of the patient. A small amount of fluid is then removed using the vacuum in the tube; the fluid is examined then under a microscope by the pathologist
- Biopsy: A small amount of tissue is excised for examination from the lungs during a bronchoscopy or through a surgery (rare) in which the surgeon removes a small tissue of the lung for examination. The tissue is the examined under the microscope to look for changes specific to this condition. It is considered to be the best test to confirm a diagnosis of Pulmonary Alveolar Proteinosis
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Pulmonary Alveolar Proteinosis?
Complications of Pulmonary Alveolar Proteinosis may include:
- Lung infections
- Lung fibrosis
- Cor pulmonale (right-side heart failure)
How is Pulmonary Alveolar Proteinosis Treated?
The treatment of Pulmonary Alveolar Proteinosis depends upon the degree of impairment of lung function, progression of the condition, and associated infections (if any). PAP may be treated as follows:
- For the primary condition, the most common treatment modality used is whole-lung lavage. In this procedure, which is performed under general anesthesia, the whole lung is flooded with fluid (saline) from outside and then the fluid is removed by vacuum, causing the removal of the deposited grainy material
- Several other new experimental modalities may be used that include injection or inhalation of GM-CSF
- Another method that is used is plasmapheresis, in which the antibodies are removed from blood
- A lung transplant may be required in certain congenital cases or when the patient does not respond to the above-mentioned treatment measures
- In case of secondary form of PAP, it is important to treat the co-existing medical condition
How can Pulmonary Alveolar Proteinosis be Prevented?
Currently, there are no effective preventive measures available for Pulmonary Alveolar Proteinosis.
What is the Prognosis of Pulmonary Alveolar Proteinosis? (Outcomes/Resolutions)
- The prognosis of Pulmonary Alveolar Proteinosis is typically good. A majority of the patients respond to whole-lung lavage excellently
- In some patients who fail to improve with repeated whole-lung lavage, the outcome is poor and it can lead to pulmonary fibrosis
- For congenital form of PAP, a lung transplant can bring about a favorable outcome
Additional and Relevant Useful Information for Pulmonary Alveolar Proteinosis:
The following DoveMed website link is a useful resource for additional information:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.