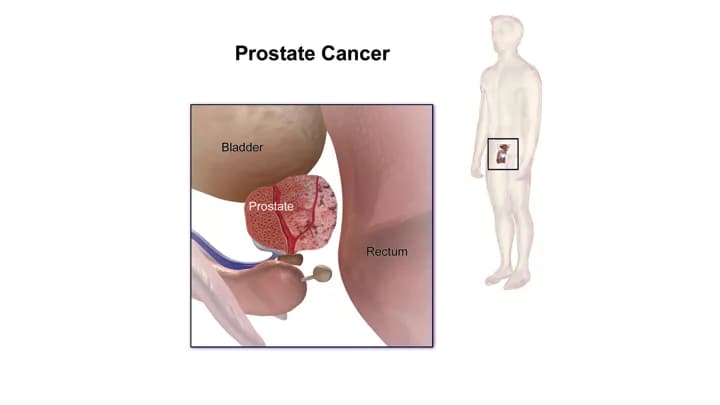
Prostate Cancer
What are the other Names for this Condition? (Also known as/Synonyms)
- Cancer of the Prostate
- Prostatic Adenocarcinoma
What is Prostate Cancer? (Definition/Background Information)
- Prostate Cancer is a type of cancer that develops within the tissues of the prostate gland. The prostate gland is a gland that encircles the urethra in males. It secretes a fluid, which forms a part of the semen
- Prostate Cancer is among the most prevalent types of cancers in men. Men over the age of 65 years have an increased risk of developing this type of malignancy, while men below 45 years are rarely diagnosed with Prostate Cancer
- If Prostate Cancer is detected and diagnosed early and is found confined within the prostate gland, then the prognosis following a successful treatment is usually good
The type of normal prostate cells that transform to malignancy defines the Prostate Cancer type. This helps determine the appropriate treatment course. There are many types of Prostate Cancers such as small cell carcinomas, transitional cell carcinomas, or sarcomas. Some of these include:
- Adenocarcinoma of the Prostate Gland: It is the most commonly diagnosed type of Prostate Cancer comprising approximately 95% of all cases. This type of cancer usually develops from the cells in the peripheral region of the prostate. There are two types of adenocarcinoma - acinar type and ductal type. Among these, the acinar type of adenocarcinoma is the most common kind
- Small Cell Carcinoma of the Prostate Gland (SCCP): It is also known as Oat-Cell Carcinoma. It is a very rare, aggressive and neoplastic type of Prostate Cancer comprising only 2% of all cases. These cancer cells are small, round and look like oats, when viewed under the microscope by a pathologist
According to the WHO Classification of Urinary and Male Genital Tumors (2019), 5th Ed., Vol. 8, benign and malignant tumors of the prostate are classified in the following manner:
Tumors of the prostate
Epithelial tumors of the prostate
- Glandular neoplasms of the prostate
- Prostatic cystadenoma
- High-grade prostatic intraepithelial neoplasia
- Intraductal carcinoma of the prostate
- Prostatic acinar adenocarcinoma
- Prostatic ductal adenocarcinoma
- Treatment-related neuroendocrine prostatic carcinoma
- Squamous neoplasms of the prostate
- Adenosquamous carcinoma of the prostate
- Squamous cell carcinoma of the prostate
- Adenoid cystic (basal cell) carcinoma of the prostate
Mesenchymal tumors unique to the prostate
- Stromal tumors of the prostate
- Prostatic stromal tumor of uncertain malignant potential
- Prostatic stromal sarcoma
Who gets Prostate Cancer? (Age and Sex Distribution)
- A majority of the cases are detected and diagnosed in men over the age of 65; over 60% of Prostate Cancers are diagnosed in this age group
- Men under the age of 40-45 years are rarely diagnosed with Prostate Cancer
- Worldwide, men of all races and ethnic groups are at risk for the malignancy. The prevalence of Prostate Cancer is lower in Central and South Americas, Asia, and Africa; while it is higher in Australia, the North American continent, and among northwestern European nations
In the United States, it is more prevalent among African Americans, and less noted among Asian Americans and Hispanics.
What are the Risk Factors for Prostate Cancer? (Predisposing Factors)
The underlying cause of Prostate Cancer is unknown at this time, although physicians believe that certain factors may increase an individual’s risk for the condition. The risk factors include:
- Advancing age: The chances of Prostate Cancer increases as one age, especially for men over 50 years or age. Most cases occur in adult men over 65 years old
- Race: African Americans are found to have a higher risk, than any other race
- Family history: Men with one or more immediate family members, such as brother or father, or relatives with a history of the cancer
- Personal history: Individuals with a history of Prostate Cancer have an increased threat for disease recurrence
- Obesity: Obese men may have an elevated risk for developing more aggressive forms of Prostate Cancer
- Lynch syndrome: In men with this condition, there is an increased risk for several cancers including Prostate Cancer
- Dietary factors: According to some research, those who consume a lot of milk-based (dairy) products or calcium foods and supplements, may have a slightly increased risk
Other factors being studied that may potentially influence the development of Prostate Cancer include smoking tobacco, exposure to chemicals, prostatitis, sexually-transmitted infections, and vasectomy.
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Prostate Cancer? (Etiology)
Currently, medical research is being conducted to determine the exact cause of Prostate Cancer. Healthcare providers believe that certain factors may increase one’s risk for the condition.
- Mutations in BRCA1 or BRCA2 genes are known to increase a man’s risk for Prostate Cancer
- Some researchers believe that the malignancy may develop from certain precancerous changes in the prostate gland, which may be revealed on a prostate biopsy
- Such changes, termed prostatic intraepithelial neoplasia (PIN), are further classified as low-grade and high-grade:
- Low-grade prostatic intraepithelial neoplasia: According to current research, low-grade PIN is not believed to contribute towards an increased for Prostate Cancer
- High-grade prostatic intraepithelial neoplasia: Individuals with high-grade PIN is stated to have an increased risk, and is potentially a precursor to Prostate Cancer
- Another contributing factor is termed proliferative inflammatory atrophy (PIA), another type of prostatic change that may potentially result in high-grade PIN
Per studies, prostatic intraepithelial neoplasia has even been reported in young adult men in their 20s and 30s. nevertheless, it is important to note that a majority of men with PIN may never develop Prostate Cancer.
What are the Signs and Symptoms of Prostate Cancer?
Early-stage Prostate Cancer may not present any significant signs and symptoms (during the initial stages). The condition may be difficult to diagnose initially because several of the primary symptoms could be the result of other medical conditions too. The overlapping signs and symptoms may cause a delayed diagnosis of Prostate Cancer.
Signs and symptoms are usually observed during the later stages of the disease and these include:
- Weak urinating stream resulting in frequent urination necessity
- Difficulty in emptying the bladder completely
- Frequent urination at night (nocturia)
- Pain when urinating
- Back and abnormal pain
- Hematuria (blood in urine)
- Erection issues during sex; pain while ejaculating
- Hematospermia (blood in semen)
- Numbness in the legs
How is Prostate Cancer Diagnosed?
There are a variety of tests to detect, locate, and diagnose Prostate Cancer and its potential spread. A surgical procedure called biopsy, usually performed by an urologist, is the only test a physician relies on, to make an accurate diagnosis of Prostate Cancer. However, if a physician is unable to perform a prostate gland biopsy due to the risk of damaging vital organs, additional tests may be recommended.
A few of the tests used to screen or diagnose Prostate Cancer include:
- Digital rectal exam (DRE): During a DRE exam, a physician uses their fingers (using lubricated rubber gloves) to physically detect any abnormalities within the prostate
- Computerized tomography (CT) scan: Also known as CAT scan, this radiological procedure creates detailed three-dimensional images of structures inside the body. CT scans are not a tool of preference to detect Prostate Cancer; though they may be helpful in detecting a recurrence, or if the cancer has metastasized to the pelvic lymph nodes or other body parts
- Prostate specific antigen (PSA) blood test: Prostate specific antigen is a glycoprotein produced by the prostate gland. Occasionally, tiny amounts of PSA may flow in the bloodstream. In a PSA test, a blood sample is drawn from the patient’s arm and checked for abnormal levels of PSA (if any)
- Magnetic resonance imaging (MRI) scan: An MRI uses a magnetic field to create high-quality pictures of certain parts of the body such as tissues, muscles, nerves, and bones. These high-quality pictures may reveal the presence of Prostate Cancer
- Bone scan: Bone scans are primarily used to detect if the cancerous tumor in the prostate gland has metastasized to a patient’s pelvis or other body parts. A bone scan is a nuclear imaging test that involves injecting a radioactive tracer into a patient’s vein
- Trans-rectal ultrasound (TRUS): In this diagnosis method, a tiny probe is inserted into the patient’s rectum to take pictures of the prostate gland through emission of sound waves
- Molecular genetic testing, if necessary
A biopsy refers to a medical procedure that involves the removal of cells or tissues, which are then examined by a pathologist. A biopsy procedure of the prostate gland would include:
- Trans-rectal biopsy: During a trans-rectal biopsy, a special biopsy forceps is used to pass through the rectal wall into the prostate in order to collect small tissue samples from within the gland. A pathologist examines these samples under a microscope, after processing the tissue in an anatomic pathology laboratory
- Lymph node biopsy, if needed
Some of the Prostate Cancer associated signs and symptoms may be caused by other health conditions too, such as benign prostatic hyperplasia (BPH), and a differential diagnosis may be undertaken to exclude them.
Many clinical conditions may have similar signs and symptoms to prostate cancer. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Prostate Cancer?
The complications of Prostate Cancer may include:
- Individuals with Prostate Cancer have an increased risk of the cancer metastasizing to other adjoining parts of the body such as the pelvis or bones (most frequent)
- Urinary incontinence is an embarrassing and distressing condition that causes the individual to have a loss of bladder function. It is commonly seen in patients who have endured normal treatments for Prostate Cancer
- Erectile dysfunction (impotence) is a sexual dysfunction resulting from the inability of men to develop, or hold an erection during sexual intercourse
How is Prostate Cancer Treated?
A treatment of Prostate Cancer depends on a number of factors that include:
- Histological type of the Prostate Cancer
- Stage of the cancer
- The overall health status of the individual
- Treatment preferences of the individual
Early-stage Prostate Cancer treatment: Active surveillance
- It is a choice given to patients who are diagnosed with early-stage Prostate Cancer, but do not desire to undergo an immediate surgery or radiation therapy
- Active surveillance is the process of monitoring the signs and symptoms of Prostate Cancer, which is undertaken by healthcare providers
- Occasionally, a PSA blood test and digital rectal exam may be administered, along with biopsies, in order to allow a physician, observe the progression of cancer
Surgery for Prostate Cancer: The recommended surgical treatment for men with Prostate Cancer involves surgical removal of the prostate gland. The surgical treatments a physician may recommend include:
- Radical retropubic prostatectomy: Radical retropubic prostatectomy is the surgical removal of the entire prostate gland, usually performed by a urologic oncologist. During this procedure, the surgeon removes the prostate gland, seminal vesicles, and the surrounding lymph nodes of the pelvis through a small incision in the abdomen. This surgery is used in cases where the cancerous tumor is still centralized within the prostate gland
- Radical perineal prostatectomy: It is also the surgical removal of the entire prostate gland, usually performed by a urologic oncologist. The prostate gland is removed through a small incision between the anus and scrotum. Like radical retropubic prostatectomy, a radical perineal prostatectomy surgery is used when the cancerous tumor is still contained within the prostate gland
- Laparoscopic radical prostatectomy (LRP): During an LRP, an incision is made in the abdomen, and using a laparoscope, the prostate gland is removed
- Cryosurgery: It is a cryosurgical treatment that is effective in treating early stages of Prostate Cancer. Cryosurgery involves the use of liquid nitrogen to freeze cancer cells by means of an instrument called a cryoprobe. The cryoprobe is inserted through a tiny incision between the scrotum and anus
- Transurethral resection of the prostate (TURP): It is a urological procedure that is frequently used to treat advanced cases of Prostate Cancer. A urologist performs this procedure during which a surgical instrument, called a resectoscope, is passed through the urethra and into the prostate. Excess tissue within the prostate causing obstruction of the urinary tract is removed. This procedure is also used to treat a condition called benign prostatic hyperplasia (BPH). TURP is performed rarely and on a small proportion of patients, those who are not candidates for extensive radical prostatectomy procedures
- High frequency ultrasound (HIFUS): During a high frequency ultrasound procedure, a tiny probe is inserted through the rectum and into the prostate, precisely targeting the cancerous cells using ultrasound waves. HIFUS employs an extremely accurate medical instrument, which uses ultrasound to heat and eliminate cancer cells within the prostate
Chemotherapy: Chemotherapy is a treatment method that employs drugs to kill cancer cells. For Prostate Cancer, a combination of two or more chemotherapy drugs, are generally used. These drugs are given intravenously through a vein in the arm, or by passing a tube through the rectal wall, thereby administering the drug directly into the prostate (called intravesical therapy).
Radiation therapy: Radiation therapy attempts to destroy cancer cells by aiming high-energy beams at them. It can be administered either by a machine placed outside the body (external beam radiation), or by a device positioned inside the prostate (brachytherapy). The therapy may be used either before a surgery is proposed, so as to decrease the size of the tumor allowing for its easier removal; or after the surgery is performed, in order to kill any remaining cancer cells.
Both radiation therapy and chemotherapy are sometimes used in a combined form during the course of treatment.
Hormone therapy: Hormonal therapy is a medical treatment used for men with advanced Prostate Cancer that has metastasized beyond the prostate gland. The treatment options include taking medications that affect hormone levels in the body.
- Luteinizing hormone (LH): Also called lutropin, this hormone therapy drug helps lower an individual’s testosterone level in the body or decreases the body’s ability to use the available testosterone. Prostate Cancer cells rely on androgens (male hormones such as testosterone) to proliferate; administering LH drugs, may cause the cancer cells to die out
- Anti-androgens: Anti-androgens are types of medications used to disrupt the possibility of testosterone reaching the cancerous cells in the prostate. A chemical reaction caused by these medications prevents the growth of cancerous tumor within the prostate. The types of anti-androgens medications used with this type of therapy include flutamide, bicalutamide, and nilutamide
- Bilateral orchiectomy: It is an irreversible and permanent surgical procedure in which both the testicles are removed. Bilateral orchiectomy has similar results as most hormone therapy treatments; the procedure may lower an individual’s testosterone level at a much faster rate
How can Prostate Cancer be Prevented?
Currently, there is no known and available method to prevent Prostate Cancer. Nonetheless, various steps may be taken to help decrease the incidence of the condition:
- Physical activity: Individuals with higher physical activity levels have a lesser risk for getting Prostate Cancer
- Consumption of fruits and vegetables: A healthy diet, low in saturated fats and rich in many fruits and vegetables, may help decrease the threat of Prostate Cancer. Consuming soy-based foods incorporated into a regular diet may decrease the risk
- Maintaining a healthy weight
- Certain medications, such as aspirin and 5-alpha reductase inhibitors, are known to have a positive effect on Prostate Cancer risk, but these are to be taken only per the advise of a healthcare professional
Prostate Cancer screening via PSA blood test for early detection of the condition may be beneficial in some men in the 55-69 years’ age group. According to the U.S. Preventive Services Task Force, the decision to have a PSA blood screening test is best decided by the individual himself based on discussions with their healthcare provider.
What is the Prognosis of Prostate Cancer? (Outcomes/Resolutions)
- The prognosis for Prostate Cancer depends on several factors as outlined below:
- Histological subtype and grade of the cancer
- Stage of tumor: With lower-stage tumors, when the tumor is confined to site of origin, the prognosis is usually excellent with appropriate therapy. In higher-stage tumors, such as tumors with metastasis, the prognosis is poor
- Overall health of the individual: Individuals with overall excellent health have better prognosis compared with those with poor health
- Age of the individual: Older individuals generally have poorer prognosis than younger individuals
- The size of the tumor: Individuals with small-sized tumors fare better than those with large-sized tumors
- Individuals with bulky disease have a poorer prognosis
- Involvement of vital organs may complicate the condition
- The surgical resectability of the tumor (meaning if the tumor can be removed completely) - it is a rare option
- Whether the tumor is occurring for the first time or is a recurrent tumor. Recurring tumors have worse prognosis compared to tumors that do not recur
- Response to treatment: Tumors that respond to treatment have better prognosis compared to tumors that do not respond to treatment
- Progression of the condition makes the outcome worse
- The earlier the stage and lower the grade of cancer, the better is the prognosis
- In general, individuals affected by Prostate Cancer have a survival rate of approximately 93% at 10 years, and 77% at 15 years (after the onset of cancer)
An early diagnosis and prompt treatment of Prostate Cancer generally yields better outcomes than a late diagnosis and delayed treatment.
Additional and Relevant Useful Information for Prostate Cancer:
The National Cancer Institute estimates that around 250,000 new cases would be diagnosed, and over 33,000 people die from Prostate Cancer in the United States, during the year 2011.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.