What are the other Names for this Condition? (Also known as/Synonyms)
- Chronic Obliterative Cholangitis
- Fibrosing Cholangitis
- Stenosing Cholangitis
What is Primary Sclerosing Cholangitis? (Definition/Background Information)
- Primary Sclerosing Cholangitis (PSC) is considered to be an autoimmune disease that is characterized by inflammation of the biliary duct (duct that carries bile from the liver to the small intestine), which ultimately results in scarring
- When scarring of the bile duct occurs, bile cannot be properly carried from the liver to the gut. As a result, bile builds up in the liver (cholestasis) and becomes toxic. PSC is a rare disorder that most commonly affects young and middle-aged male adults
- The condition is more common in developing nations, likely due to limited access to ERCP (endoscopic retrograde cholangiopancreatography) to make a diagnosis. ERCP is a diagnostic tool that visualizes the stomach, duodenum, and biliary tree (bile duct)
- Even though the exact mechanism of Primary Sclerosing Cholangitis is mostly unknown, researchers believe it may be due to multiple factors such as autoimmune mechanisms, genetic predisposition, and unknown mechanisms. A family history of PSC can increase one’s risk of developing the condition
- The common signs and symptoms of PSC include jaundice, itching, indigestion, anorexia, fatigue, diarrhea, dark urine, and yellowing of the eyes
- The disorder is generally treated through nutritional supplements, balloon dilation or stent insertion, and liver transplantation (if necessary for progressive cases)
- If Primary Sclerosing Cholangitis is left untreated or if it progresses despite treatment, liver failure and cirrhosis may occur. This can progress to cholangiocarcinoma (cancer of the bile duct). PSC is also frequently associated with ulcerative colitis (causing digestive tract inflammation and ulcers) and can result in colon cancer
Who gets Primary Sclerosing Cholangitis? (Age and Sex Distribution)
- Primary Sclerosing Cholangitis usually affects adults, but it can also occur rarely in children. The typical age of onset is between 25 and 45 years
- This condition is more common in males (approximately 65% of the cases) than in females
- PSC can be seen worldwide; nevertheless, it is more commonly diagnosed in the developed nations, due to better access to advanced healthcare facilities
- It is more common in Scandinavian countries and amongst Jewish populations
What are the Risk Factors for Primary Sclerosing Cholangitis? (Predisposing Factors)
Risk factors of Primary Sclerosing Cholangitis include:
- Males are more likely to develop PSC than females
- Genetic abnormalities that can be passed through families are believed to contribute to its development
- Individuals diagnosed with inflammatory bowel disease (such as ulcerative colitis) are at higher risk of PSC
- Jews and Caucasians have an increased risk of developing Primary Sclerosing Cholangitis, when compared to African Americans, Hispanics, or Asians
- Smoking is a risk factor
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Primary Sclerosing Cholangitis? (Etiology)
The exact cause and mechanism of Primary Sclerosing Cholangitis is currently unknown. Scientists believe that it may be caused due to the presence of multiple factors (multifactorial).
- It is associated with histocompatible leucocyte antigens (HLA) such as B8, DR3, and DR4. HLAs are antigen molecules that are found on the surface of cells and are used to identify a cell as self or non-self. When the body identifies these HLAs are non-self, it leads to an autoimmune response
- It is believed that genetic abnormalities or other unknown factors may be the causative factors in stimulating one’s immunity to act against specific tissues in the body (autoimmune mechanism)
What are the Signs and Symptoms of Primary Sclerosing Cholangitis?
The signs and symptoms of Primary Sclerosing Cholangitis can include:
- Itching, which is one of the earliest symptoms of Primary Sclerosing Cholangitis
- Icterus or yellowing of the eyes can be caused by obstructive jaundice, which results in blockage of bile flow from the liver. As a result, bile (bilirubin) is redirected into blood causing yellowing of the eyes and skin.
- Dark urine, as a result of excretion of bile by-products into urine
- Anorexia, fatigue, malaise (general discomfort or unease), and abdominal pain
- Nutritional deficiencies, especially in vitamins A, D, E, and K, due to the lack of bile in the intestine to absorb these vitamins
- Ascending cholangitis (inflammation and infection of the bile duct), which can cause fever and sepsis (toxins and bacteria within the tissues and blood)
- Diarrhea, which results from an inability to digest fats, due to lack of bile
- Liver cirrhosis can also occur as an end result of Primary Sclerosing Cholangitis. This may result in signs of portal hypertension, such as blood in the stool, enlargement of the spleen, development of ascites (fluid accumulation in the peritoneal cavity), and hepatic encephalopathy (confusion or forgetfulness as a result of liver dysfunction)
How is Primary Sclerosing Cholangitis Diagnosed?
Primary Sclerosing Cholangitis is diagnosed using the following tools:
- Thorough evaluation of the individual’s medical history and a complete physical examination. An evaluation of medical history can help determine, if there is a presence of predisposing factors such as family history or history of inflammatory bowel disease. Physical examination and clinical workup may uncover findings such as jaundice
- Liver function tests are blood tests which provide information about the state of the individual’s liver. They check the levels of albumin, bilirubin, liver transaminases (AST and ALT), and alkaline phosphatases
- Other blood tests that may be undertaken in an individual suspected of Primary Sclerosing Cholangitis are antineutrophil cytoplasmic antibodies (ANCA), antinuclear antibody (ANA), anticardiolipin, rheumatoid factor, anti-Saccharomcyes cerevisiae antibodies, etc.
- Endoscopic retrograde cholangiopancreatography (ERCP) and magnetic resonance cholangiopancreatography (MRCP) are non-invasive diagnostic tools that can be used to visualize bile ducts, which may be narrowed, dilated, or lost. ERCP is considered to be a gold-standard tool in PSC diagnosis
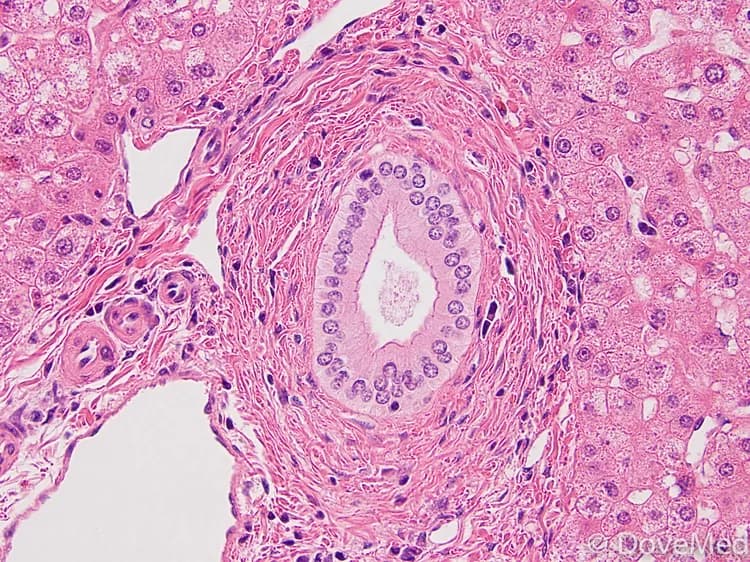
- Liver biopsy is one of the definitive diagnostic tools to establish Primary Sclerosing Cholangitis, especially for small bile duct disease. Small bile ducts affected by PSC may be difficult to visualize through ERCP or MRCP. During liver biopsy, the physician removes a sample of the liver tissue and sends it to the laboratory for a histopathological examination. The pathologist examines the biopsy under a microscope and arrives at a definitive diagnosis after a thorough evaluation of the clinical and microscopic findings, as well as by correlating the results of special studies on tissues (if required). Biopsy may identify inflammation surrounding the bile ducts, narrowing of the bile duct lumen, loss of bile ducts, “onion skin fibrosis” around the bile duct, and cirrhotic nodules
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions in order to arrive at a definitive diagnosis.
What are the possible Complications of Primary Sclerosing Cholangitis?
Complications associated with Primary Sclerosing Cholangitis depend on the severity of the disease and can include:
- Liver failure arising due to cirrhosis
- Development of osteoporosis in individuals with PSC, due to their inability to absorb vitamin D
- Scarring of the bile ducts leads to obstruction of bile flow from liver to the gut. As a result of this obstruction, bacteria from the gut ascends up the bile duct causing infection
- Esophageal varices: Enlarged veins in the bottom portion of the esophagus that connects the throat and stomach
- Cholangiocarcinoma (bile duct cancer) can occur if PSC is left untreated, or if it progresses
- If Primary Sclerosing Cholangitis is associated with ulcerative colitis, there is an increased risk for colon cancer
How is Primary Sclerosing Cholangitis Treated?
A typical treatment plan for an individual with Primary Sclerosing Cholangitis can include:
- Antihistamines to treat itching
- Vitamins to supplement nutritional deficiencies
- Antibiotics to prevent infection and sepsis
- Stenting (placement of a hollow tube at the blocked site) in the bile duct to treat bile duct blockage
- Balloon dilation (insertion of a balloon catheter through an endoscope into the bile duct). Once the balloon is at the blocked site, it is inflated to widen the bile duct for removal of the blockages
- Liver transplant may be required if PSC progresses and liver cirrhosis or cholangiocarcinoma occur
Regardless of what treatment is received, follow-up care and regular screenings are important to ensure that Primary Sclerosing Cholangitis does not progress and cause further complications.
How can Primary Sclerosing Cholangitis be Prevented?
- Currently, no preventative measures are known for Primary Sclerosing Cholangitis
- However, it is important to undergo regular medical screenings so that PSC does not advance and cause more complications
What is the Prognosis of Primary Sclerosing Cholangitis? (Outcomes/Resolutions)
- Primary Sclerosing Cholangitis is a progressive disease. Individuals with the condition may on an average survive for 12-17 years
- Factors that worsen the prognosis are hepatosplenomegaly, increased levels of bilirubin and AST, lower levels of albumin, esophageal variceal bleeding, large dominant duct scarring, and other underlying conditions
- PSC can recur, even with liver transplantation
Additional and Relevant Useful Information of Primary Sclerosing Cholangitis:
Liver transplantation is a procedure that involves the surgical removal of a damaged or diseased liver and replacement with a healthy liver, from a suitable and compatible donor
The following article link will help you understand liver transplantation surgical procedure:
http://www.dovemed.com/common-procedures/procedures-surgical/liver-transplantation/
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.