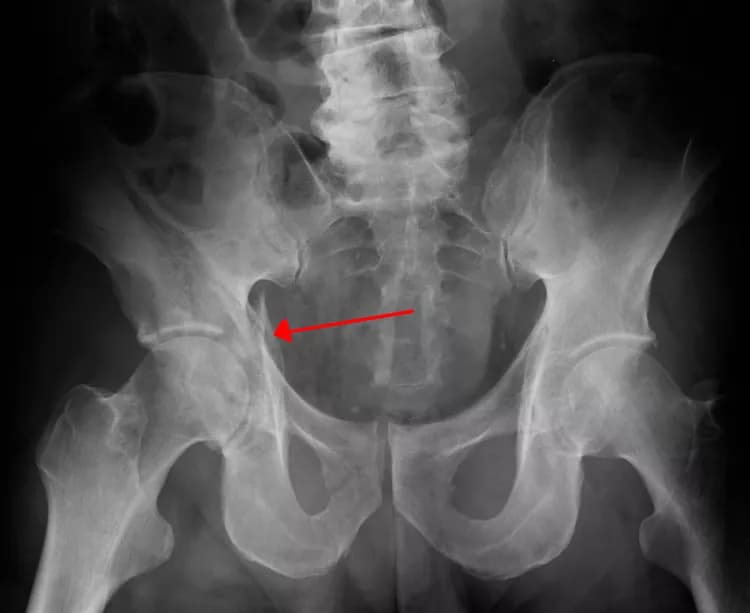
Pelvic Fracture
What are the other Names for this Condition? (Also known as/Synonyms)
- Fracture of the Pelvis
- Fractured Pelvis
What is Pelvic Fracture? (Definition/Background Information)
- The pelvis consists of 3 bones, called ischium, ilium, and pubis. These 3 bones join to form a bowl-like structure, in the lower abdomen
- The pelvis houses vital organs, such as the reproductive organs, digestive organs, and genitourinary organs. They are positioned within this pelvic cavity bowl
- A Pelvic Fracture is a serious injury that occurs, when one or more bones within the pelvis, breaks/fractures. This may lead to damaging consequences, to these critical organs, located within the pelvis
Who gets Pelvic Fracture? (Age and Sex Distribution)
- Pelvic Fractures are non-specific fractures, and as such, may occur in individuals of any age, race, ethnic group, and gender
- Individuals over the age of 65 years, have the highest rate of occurrence
What are the Risk Factors for Pelvic Fracture? (Predisposing Factors)
Common risk factors associated with a Pelvic Fracture include:
- Participation in high-risk contact sports, such as football
- Degenerative bone disease (osteoporosis)
- An advanced age (elderly adults are higher prone to such fractures)
- Reduced muscle strength
- Prior history of falls
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Pelvic Fracture? (Etiology)
Some of the causes associated with a Pelvic Fracture include:
- Direct trauma to the pelvis due to an automobile accident
- Taking part in any rough or high-impact sport
- Falling from a significant height; especially landing on one’s pelvis (or the fracture occurring since the individual is overweight)
- Prolonged use of steroidal medication, such as prednisone, may weaken the bones
What are the Signs and Symptoms of Pelvic Fracture?
Signs and symptoms of a Pelvic Fracture include:
- Lower back, abdomen pain; may be excessive pain
- Noticeable abdominal discoloration due to internal bleeding
- Difficulty walking, altered gait when walking
- Blood in urine
- Feeling of dizziness
- Weakness and numbness felt in the lower extremities
- Bruising around the pelvic joint
- Inability to control stools (incontinence)
How is Pelvic Fracture Diagnosed?
Diagnostic methods that a physician may use to help diagnose a Pelvic Fracture include:
- Physical examination: A thorough physical examination is important in identifying any noticeable deformities, swelling, contusions, within the pelvis. Individuals are also expected to provide an explanation of the circumstances that caused the injury. In addition to this, a complete medical history can aid in arriving at a definitive diagnosis
- X-ray of the pelvis: X-rays are the most common method in evaluating a fracture, if the bone has been displaced. This diagnostic test helps provide a clear image of the bone, identify the exact location of the injury, and determine the extent of the fracture.
- Computerized tomography (CT) scan: A CT scan takes a series of X-ray images from several different angles, which are then merged to create cross-sectional images of bones and soft tissues of the body. This allows a physician to examine the pelvic region and surrounding structures
- Magnetic resonance imaging (MRI): An MRI is a more detailed scan that uses radio waves and a magnetic field to generate thorough images of the interior bones and soft tissues
- General ultrasound imaging: An ultrasound produces high-frequency sound waves that are used to generate clearer images of the pelvis
- Urinalysis: Urinalysis is a collection of tests that analyze a sample of the patient’s urine
- Kidney function test: A kidney function test is a common laboratory test used to determine if the kidneys are functioning properly
- Complete blood count (CBC): CBC is a blood test that helps evaluate an individual’s overall health. This test also helps identify a collection of diseases, such as anemia, infections, and leukemia
What are the possible Complications of Pelvic Fracture?
A Pelvic Fracture is a serious but treatable injury. However, some complications associated with this fracture could include:
- Sexual and bowel dysfunction
- Pressure ulcers
- Muscle atrophy
- Unstable gait
- Fracture of the hip
- Deep vein thrombosis (blood clots in the legs)
How is Pelvic Fracture Treated?
The treatment of Pelvic Fractures usually depends on the extent and severity of the injury.Nonsurgical treatment methods include:
- Any activity that aggravates the pelvic condition should be avoided. The physician may advise the individual to refrain from participating in any physical activities, till the pain or symptoms get better
- Applying ice to the pelvic region can help reduce pain and swelling
- Complete immobilization of the pelvis with a cast, may be required to restrict movement
- Non-steroidal anti-inflammatory oral medications, such as indomethacin and naproxen, may be used to treat a Pelvic Fracture. These medications can help decrease the pain and swelling
- Individuals are likely to need physical therapy exercises after the cast is removed. The goals of these exercises are to strengthen the pelvic muscles, improve flexibility, and decrease stiffness. It may take several months for an individual to complete the physical therapy program and regain full strength and functionality
Surgical treatment methods are:
- Open reduction and internal fixation (ORIF): Open reduction is a surgical procedure to realign the fractured bone, to its original position. Surgical hardware (such as plates, screws, or rods) is then used to stabilize the fractured bone under the skin
How can Pelvic Fracture be Prevented?
To prevent a Pelvic Fracture, individuals should be careful and consciously aware, while performing any physical activities, such as sports, or even some normal daily activities that could lead to situations involving accidents. Children must be provided a safe environment to work, study, or play. Any possible dangers should also be anticipated and appropriate safety measures adopted.
A few ways to further help prevent unwanted injuries or a Pelvic Fracture include:
- Individuals who participate in any high-risk sports, should wear appropriate safety equipment to help prevent the possibility of such fractures
- Wearing appropriate footwear (such as the proper shoe size) may help prevent accidents
- Consuming foods rich in calcium, such as milk, yogurt, and cheese, help build bone strength. Regular diet with appropriate calcium-intake is recommended, even after a Fracture of the Pelvis. For women, the recommended amount of calcium, increases with age and menopause
- Perform weight-bearing exercises to strengthen bones
What is the Prognosis of Pelvic Fracture? (Outcomes/Resolutions)
- A Pelvic Fracture is a serious injury; it may cause permanent disabilities. It has been observed that 50% of all serious (compound) Pelvic Fracture injuries, result in life-threatening complications
- When properly treated and rehabilitated, usually under the guidance of a physiotherapist/specialist, a high percentage of individuals regain their full strength and range of motion in the injured pelvis
Additional and Relevant Useful Information for Pelvic Fracture:
A hip fracture is a fracture of the proximal end of the femoral shaft (fracture in the thighbone, nearer to the hip).
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.