What are the other Names for this Condition? (Also known as/Synonyms)
- Body Crabs Infestation
- Body Lice Infestation
- Vagabond’s Disease
What is Pediculosis? (Definition/Background Information)
- Pediculosis is an infestation caused by lice that live on the hairy parts of the body. Lice are parasites (small insects) that live on human blood, in the clothing and bedding of affected humans, causing severe itching
- There are primarily three types of lice that reside and feed on blood at different locations of the human body. These include:
- Pediculus capitis or head louse that live in the hair on the head and feed on the human scalp
- Pediculus corporis or body louse found along the seams of infrequently changed and washed clothing
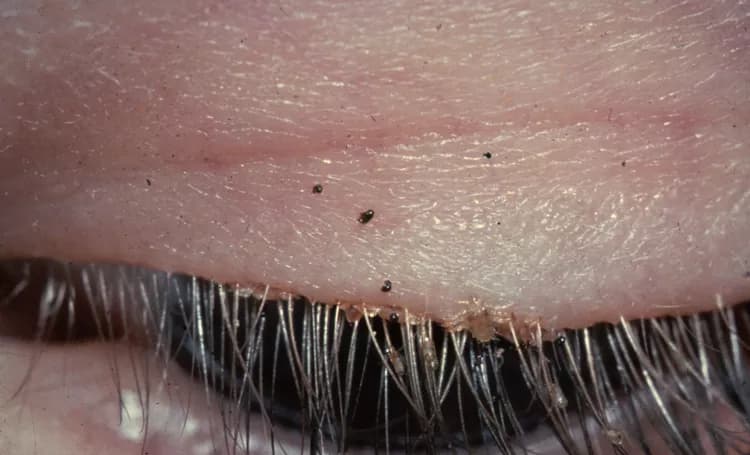
- Pediculus pubis (or pthirus pubis) which are pubic louse (or body crab) found in the pubic hair, but may also occur in the facial hair such as the eye lashes and eye brows, chests, armpits, and abdomen
- Pediculosis infestation can easily spread from one individual to another by close physical contact and through fomites (inanimate objects which are capable of spreading disease) such as combs, clothes, hats, and cosmetic applicators
- Pubic Lice Infestation can be transmitted without or during sexual activity. It can be associated with other STDs and serve as an indicator for the same
- Intense itching in the affected areas is the most common symptom of the condition. The constant scratching may make the skin raw and susceptible to secondary bacterial infections
- Medicated shampoos containing insecticidal compounds are used to treat head lice. Environmental control measures and personal hygiene can help treat and control Pediculosis affecting the body and pubic region. With proper treatment, Pediculosis is an entirely manageable condition
Who gets Pediculosis? (Age and Sex Distribution)
- Any individual regardless of their age, sex, race or ethnicity, and standards of personal hygiene are susceptible to Pediculosis, if they come in contact with an affected individual
- Head lice are usually common in school settings, college institutions, and childcare settings, indicating that they affect school children the most. Also, due to their generally longer hair, girls and women are more prone to this condition
- Pubic lice are generally prevalent among sexually-active individuals (age group 15-40 years)
- Body lice are mostly found among those with poor personal hygiene; those who do not have a chance to bathe regularly, change their clothes frequently. Adult populations are mostly affected by body lice
- Pediculosis is found worldwide; the condition is observed in both the developed and developing regions of the world
What are the Risk Factors for Pediculosis? (Predisposing Factors)
The following are the risk factors of Pediculosis:
- Being in overcrowded places such as schools, correctional facilities, etc.
- Poor standards of hygiene: Individuals with poor cleanliness standards, those who have little to no access to bathe regularly, change clothes frequently or wear clean clothes, are at a high risk
- Homeless: People who have no permanent place to stay and live, those who live on the streets, in shanty dwellings, can easily be affected by Pediculosis
- Transient populations: People moving from one place to another and not settling down in one place (such as refugees) are susceptible to Pediculosis
- Girls, and in general the female gender are at higher risk for head lice
- The infestation is more common during summers (warmer months)
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Pediculosis? (Etiology)
Pediculosis is an infestation caused by lice (singular ‘louse’) on various (hairy) parts of the body. Lice are blood-sucking ectoparasites (ectoparasites live outside the body, unlike internal parasites such as worms) that live on the body, clothing, and bedding of the affected individuals.
- Pediculosis Capitis or Head Louse Infestation is caused by Pediculus humanus var. capitis. It feeds on the scalp and spreads through close physical or ‘head-to-head’ contact, shared clothing, hats, combs, and hair brushes
- Pediculosis Corporis or Body Louse Infestation caused by Pediculus humanus var. corporis. It lives in the seams of the clothing and thrives when the same clothing is used for a prolonged time. Body lice spread through sharing of bed sheets and clothes, and is prevalent in places where overcrowding is common and very poor standards of personal hygiene exist
- A Pediculosis Pubis or Crab Louse Infestation is caused by Phthirus pubis. It lives in the pubic hair and spreads through sexual activity and intercourse, or when individuals come in direct contact with the clothes, bed sheets, and towels of infected individuals
What are the Signs and Symptoms of Pediculosis?
The very first sign that is common to all type of Pediculosis is intense itching sensation where the lice feed. This could include:
- Scratching at the back of the head or around the ears indicating the presence of head lice
- Itching sensation in the genital area indicating the presence of crab lice
The signs and symptoms vary and depend on the type of Lice Infestation, namely:
- Pediculus capitis or head lice
- Excoriations – deep scratch marks and sores on the skin
- Foul-smelling, dull, and lustreless hair
- Abnormal enlargement of the occipital and cervical lymph nodes
- Rashes on the trunk caused by sensitization
- Pediculus corporis or body lice:
- Appearance of small, red, inflammatory bumps on the shoulders, trunk, and buttocks
- Excoriations
- Dry, discolored, thick-crusted, scaly skin
- Secondary bacterial infections
- Scarring of skin
- In very severe cases, the accompanying symptoms may include headaches, fever, and malaise
- Pediculus pubis or crab lice:
- Skin irritation
- Small grey-blue spots, called maculae caeruleae, appear on the thighs and genitalia
How is Pediculosis Diagnosed?
A diagnosis of Pediculosis may include:
- Complete evaluation of medical history and thorough physical exam. Scalp hairs are examined carefully for nits, which are small white eggs attached to the hair shafts near the scalp. Sometimes, the lice may be visible moving about on the scalp
- During the physical examination:
- The genital areas are checked thoroughly for the presence of nits (white-colored eggs of lice) and adult lice, which may be attached to the hair shaft
- Pubic lice, when removed gently with a forceps, move more slowly than head or body lice
- The physician also shall examine for signs of an infection called impetigo
- The eye lashes of young children may be checked carefully with the help of a high-powered magnifying glass
- Teenagers and adults with pubic lice may be tested for other sexually-transmitted infections
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Pediculosis?
The constant itching and scratching caused by Pediculosis may make the skin raw and susceptible to secondary bacterial infections.
How is Pediculosis Treated?
The treatment of Pediculosis includes the use of medications and environmental control measures to maintain cleanliness and hygiene.
- Over-the-counter medicated-shampoos containing pyrethrins (natural insecticidal compounds found on marigolds) are used to treat those with head lice
- Lindane-based shampoos may also be used, though they have to be obtained only on the prescription of a physician. However, they are not recommended for infants, young children, pregnant, and lactating women
- Retreatment after 7 to 10 days is recommended to completely eliminate all the nits (eggs). Nit combs are helpful in removing the nits and dead lice from hair
- Some natural ‘home’ treatment for lice includes the use of cleanser oil, tea tree oil, and olive oil. Tea tree oil should not be used in the groin, or come into contact with the eyes, as it can cause a severe irritant reaction
- The clothing, towels, and bedding of the patients have to be washed in hot water and dried in a hot dryer for about 20 minutes. The combs and brushes used have to be also washed; the room of the affected individuals must be vacuum cleaned
- Hats, scarves, combs, and other cosmetic accessories used by the infected individual should be washed with hot water and dried in hot air
How can Pediculosis be Prevented?
The following preventive and safety measures can be adopted to reduce the incidence of Pediculosis. These may include:
- Avoiding close physical contact with the affected individuals
- Avoiding sharing of clothes, beds, combs, and hairbrushes of individuals with known infestations of Pediculosis
- Providing education regarding lice (background, types, spread, etc.), the treatment methods, and personal hygiene, can go a long way in preventing Pediculosis and its spread
- The importance of good hygiene standards of living and sanitary conditions should be stressed
- Regular screening tests to inspect the children for hair lice could be undertaken, especially in schools, college settings, institutions, nursing homes, and at summer camps
What is the Prognosis of Pediculosis? (Outcomes/Resolutions)
The prognosis of Pediculosis is excellent with adequate treatment and hygiene measures.
Additional and Relevant Useful Information for Pediculosis:
The following DoveMed website link is a useful resource for additional information:
https://www.dovemed.com/diseases-conditions/infection-center/
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.