What are the other Names for this Condition? (Also known as/Synonyms)
- Melanoma of the Eye
- Uveal Melanoma
What is Ocular Melanoma? (Definition/Background Information)
- A melanoma is a type of cancer that develops from cells, called melanocytes. Melanocytes are cells that produce melanin; the pigment that gives skin its color
- Melanocytes are also present within the eyes. When melanomas form from melanocytes in the eye they are called Ocular Melanomas (or Uveal Melanomas)
- They represent about 5% of all melanomas. In adults, this is the most common primary cancer of the eye
- This aggressive cancer can involve any of the 3 parts of the eye:
- Choroid: A layer rich in blood supply located between the retina (visual screen of the eye, where images are formed) and sclera (white part of the eye). Melanoma of the choroid is the most common form of Ocular Melanoma
- Iris: The colored part of the eye
- Ciliary body: A layer of tissue that produces fluid inside the eye
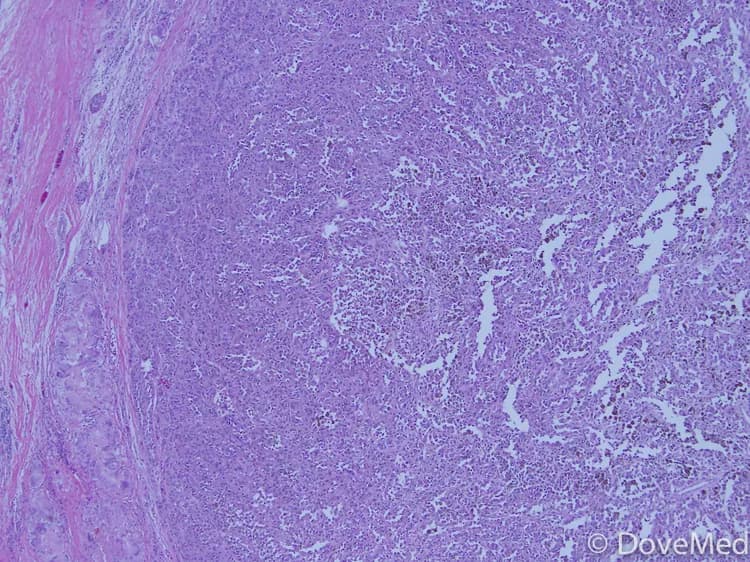
- The tumor can be composed of 2 different types of cells, when looked at under a microscope:
- Spindle-shaped cells
- Epithelioid cells: Epithelioid tumors are more capable of spreading (metastasis)
- Ocular Melanomas may be diagnosed with an eye exam by an ophthalmologist. The condition is managed using treatments, such as radiation or surgery, as determined by the physician
- Melanomas that occur in the iris have better outcomes after treatment, in comparison to those arising from the ciliary body
Who gets Ocular Melanoma? (Age and Sex Distribution)
- Ocular Melanomas can occur in any age group. In the United States, it often occurs in individuals with a median (average) age of 55 years
- These melanomas are slightly more common in men than women
What are the Risk Factors for Ocular Melanoma? (Predisposing Factors)
The risk factors for Ocular Melanoma include:
- Fair skinned individuals with light-colored eyes are more susceptible
- Those with many abnormal looking moles on their skin (a condition called dysplastic nevus syndrome) are at higher risk
- People having abnormal brown spots on the uvea (a condition called oculodermal melanocytosis or nevus of Ota)
- An inherited condition called BAP1 cancer syndrome, increases the risk for melanoma of skin and Melanoma of the Eye, as well
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Ocular Melanoma? (Etiology)
The exact cause of Ocular Melanoma is unknown. No direct linkage between sun-exposure and Ocular Melanoma has been established. However, they have been found to involve certain gene changes, most of which are thought to occur during the course of life, rather than at birth. This includes:
- Changes involving GNA11 and GNAQ oncogenes (rogue genes that cause uncontrolled cell growth and division)
- Mutations of BAP1 tumor suppressor gene (a gene that normally keeps cell growth and division in check). This factor may be inherited
What are the Signs and Symptoms of Ocular Melanoma?
Most often, Ocular Melanomas remain symptom-less, unless they grow in certain regions of the eye, or until the disease has advanced. They may be detected incidentally on a routine eye examination.
Sometimes, primary Ocular Melanomas may produce symptoms such as:
- Vision disturbances; blurred vision, shadows, or loss of vision
- Flashes of light
- A spot on the iris (colored part of the eye) that appears to grow
- Bulging of the eyeball, change in position or movement of the eyeball
How is Ocular Melanoma Diagnosed?
Ocular Melanomas can be diagnosed by an eye examination using a device called an ophthalmoscope (an instrument used to look inside the eye), and with a thorough medical history.
Other tests that are performed include:
- Ultrasound scan of the eye: High frequency sounds waves are sent through the eye and the reflected waves picked-up and converted into an image on a computer screen
- Colour fundus photography: The fundus is located behind the lens, in the back of the eye. This is photographed after dilating the pupil with eye drops
- Fluorescein angiography: A dye is injected into the arm, and as it travels into the blood vessels inside the eye, images of the back of the eye are taken using a special light that makes the dye glow (fluoresce)
- MRI (magnetic resonance imaging) scans may also be used to check for any spread of disease and tumor growth. This uses high-powered magnetic coils. MRI of the head, or any other areas suspected of having metastatic disease, may be carried out
- CT (computerized tomography) scan: This uses x-rays to take multiple pictures and produce cross-sectional images of the body part under study. This is used to check for growth of the tumor and if the melanoma has spread to other structures, outside the eye
- Blood tests to check liver function may be performed, since the liver is commonly affected by a cancer spread
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Ocular Melanoma?
The most important complication of Ocular Melanoma is spread/metastasis of the cancer. Approximately, half of the patients diagnosed with Ocular Melanoma will develop metastases (spread of cancer), within 10-15 years after diagnosis. The liver is commonly involved in metastasis. Metastatic disease most often results in death.
How is Ocular Melanoma Treated?
The choice of treatment for the primary disease (tumor inside the eye) is mainly guided by the size of the tumor. This is according to a system proposed by the Collaborative Ocular Melanoma Study (COMS) group; the tumor is classified as small, medium, or large, based on the size.
The treatment options for the primary Ocular Melanoma include:
Radiation:
- This uses high energy beams to kill cancer cells
- Eye appearance may be better preserved using radiation therapy, as compared to surgery
- Types of radiation therapy include
- Brachytherapy ("plaque therapy"): Pellets of radioactive material are surgically placed in proximity to the cancer, and left in place for 4-7 days
- External beam radiation therapy: High energy beams are focused on the cancer from outside the body
- Possible side effects include, inflammation of the eyelids, and due to any damage incurred inside the eye - development of cataract, retinal detachment, glaucoma (raised pressures inside the eyeball), or bleeding into the eye
Surgery:
- Surgical options include:
- Resection of the tumor (a complete or partial removal)
- Enucleation (removal of the entire eyeball followed by an orbital implant to take its place)
- Complications of surgery include, anesthetic complications (due to the anesthetic drug used), bleeding, and infections
- For a disease that has spread, treatment options include:
- Chemotherapy: Use of drugs to kill cancer cells
- Immunotherapy: Involves the use of drugs that boost the immune system
- Since the liver is the most commonly involved site, in order to treat the liver, the liver is isolated and infused with chemo- or immuno- therapeutic agents or radioactive beads
- Regular follow-up visits after treatment, is needed to check for any possible recurrence or spread of the cancer
How can Ocular Melanoma be Prevented?
Currently, the predisposing factors for Ocular Melanoma remain unknown; hence, the exact steps for prevention of the condition have not been determined. Some measures that may be followed include:
- Usage of UV (ultraviolet) protective sunglasses is advised, even though prolonged UV ray exposure has not been conclusively proven to cause melanoma
- Regular visits to the ophthalmologist, especially for individuals over the age of 40 years
What is the Prognosis of Ocular Melanoma? (Outcomes/Resolutions)
- Among Ocular Melanomas, melanomas of the iris have the best prognosis, while those that involve the ciliary bodies have the worst outcomes
- Once metastasis has occurred, the prognosis is poor. Without treatment, median survival time after metastasis of the cancer is around 2-8 months
However, the prognosis depends upon a set of several factors, which include:
- Stage of tumor: With lower-stage tumors, when the melanoma is confined to site of origin, the prognosis is usually excellent with appropriate therapy. In higher-stage cancers, such as those with metastasis, the prognosis is poor
- Overall health of the individual: Individuals with overall excellent health have better prognosis compared with those with poor health
- Age of the individual: Older individuals generally have poorer prognosis than younger individuals
- The size of the melanoma: Individuals with small-sized melanomas fare better than those with large-sized ones
- Individuals with bulky disease have a poorer prognosis
- Involvement of vital organs may complicate the condition
- The surgical resectability of Ocular Melanoma (meaning if the melanoma can be removed completely)
- Whether the cancer is occurring for the first time or is recurrent. Recurring cancers have worse prognosis compared to those that do not recur
- Response to treatment: Melanomas that respond well to treatment have better prognosis compared to melanomas that do not respond to treatment
- Progression of the condition makes the outcome worse (progressive Melanoma of the Eye)
An early diagnosis and prompt treatment of the condition generally yields better outcomes than a late diagnosis and delayed treatment.
Additional and Relevant Useful Information for Ocular Melanoma:
Factors that increase the risk of developing metastatic Ocular Melanomas include:
- Large tumor size
- Epithelioid tumor cells, as seen under a microscope
- Ciliary body involvement
- Orange pigment overlying the tumor
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.