What are the other Names for this Condition? (Also known as/Synonyms)
- Age-Related Macular Degeneration
- SMD (Senile Macular Degeneration)
- Wet Macular Degeneration
What is Macular Degeneration? (Definition/Background Information)
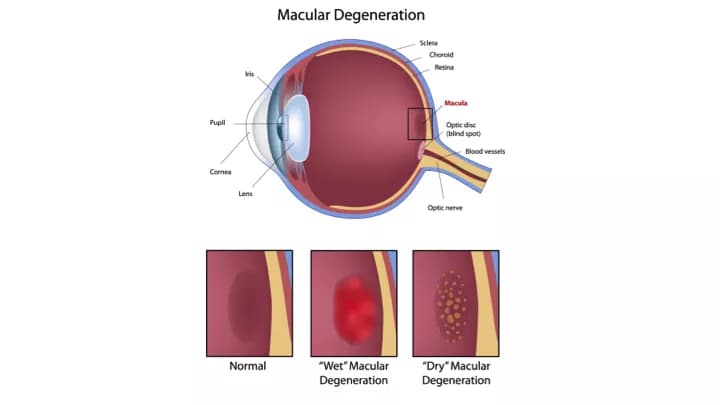
- Macular Degeneration is a disease of the eye that affects the macula, which is at the centre of the retina (behind the eyeball)
- This leads to slow deterioration of the central sharp vision, which is needed to read or drive. It most commonly occurs in older adults and hence, it is also called Age-Related Macular Degeneration (AMD) or Senile Macular Degeneration
- There are two types of Macular Degeneration:
- Wet Macular Degeneration: It is an advanced form of AMD characterized by abnormal blood vessel growth beneath the macula, leading to fluid leakage and rapid central vision loss. It can cause sudden and severe vision changes if left untreated
- Dry Macular Degeneration: It is a common eye disorder that causes blurred central vision due to the deterioration of the macula, the part of the retina responsible for sharp, central vision. This form progresses more slowly than the wet form and is characterized by the presence of yellow deposits known as drusen in the macula
- Both passive measures (such as healthy food habits, nutrition supplementation) and active treatment measures (medications, surgery, laser therapy) are available for Macular Degeneration. The prognosis of this eye disorder depends on whether it is a dry type or a wet type of Macular Degeneration
Who gets Macular Degeneration? (Age and Sex Distribution)
- Individuals aged over 55-60 years are prone to Macular Degeneration
- Females are more likely to be affected by the condition, than males
- Individuals of all races and ethnic groups can be affected, though Caucasians have a higher risk
What are the Risk Factors for Macular Degeneration? (Predisposing Factors)
The risk factors for Macular Degeneration are grouped into 2 types, uncontrollable and controllable risk factors.
Uncontrollable risk factors for Macular Degeneration include:
- Advancing age: As age increases, the risk for Macular Degeneration also increases
- Race: Caucasians are affected more than individuals of other races
- Gender: Females are more likely to develop this eye disorder
- Color of the eyes: Macular Degeneration affects individuals with blue eyes more, due to the decreased level of protective pigment in their eyes
- Eye disorders: Severe farsightedness and nearsightedness can increase the risk of Macular Degeneration
- Family history: Anyone with a family history of Macular Degeneration is at an increased risk
Controllable risk factors for Macular Degeneration include:
- Cigarette smoking
- High blood pressure
- Obesity
- High cholesterol levels
- Diet: Diet rich in fat and less in fruits and vegetables can contribute to AMD. This is due to the decreased level of antioxidants, which protects the retina
- Exposure to sunlight: Those living near the equator and in high altitudes and those with outdoor occupations may be affected more
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Macular Degeneration? (Etiology)
The exact cause of Macular Degeneration is not known.
- The dry type of Macular Degeneration is characterized by the presence of yellow deposits (drusen) in the macula (the centre of the retina, at the back of the eyeball). As these deposits increase in number, the vision is decreased
- The wet type of Macular Degeneration is characterized by the growth of abnormal blood vessels underneath the macula. These blood vessels leak blood and fluid in the back of the eye and cause vision loss
What are the Signs and Symptoms of Macular Degeneration?
The signs and symptoms of Macular Degeneration include:
- Straight lines look wavy and irregular, blurred vision
- Decreased vision, leading to difficulty in reading, watching T.V, difficulty seeing road signs, etc.
- Darkening or whitening out of the center of the field of vision
- Difficulty in recognizing faces
- Objects appear further away or smaller than usual
- Requiring more light, when doing work up close
- Colors appear less bright than usual
How is Macular Degeneration Diagnosed?
Many individuals do not recognize that they have Macular Degeneration, until their blurred vision becomes very obvious. An eye specialist can help detect the condition during its early stages using the following tests and exams:
- Amsler grid test: It is a simple vision test in which one has to look at a chart that looks like a graph paper, called the Amsler grid. If the straight lines look wavy or if some of the lines seem to be missing, then it is indicative of Macular Degeneration
- An examination of the back of the eyeball is done by dilating the eye and then examined using special lenses
- Fluorescein angiography: In this procedure, a special illuminating fluorescein dye is injected into the arm blood vessel and pictures are taken, as the dye passes through the blood vessels at the back of the eye
- Optical coherence tomography (OCT): OCT is an imaging test that is used to look for areas where the retina may be thin, or if there is fluid under the retina
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Macular Degeneration?
The complication due to untreated Macular Degeneration may include:
- Blindness
- Emotional impact leading to depression and anxiety: Adjusting to changes eyesight can be frustrating. A simple everyday activity, like reading and driving, becomes more difficult. This can affect an individual’s independence and thus affect their mental health, leading to depression and anxiety
- Central vision is very important for driving; Age-Related Macular Degeneration affects the ability to drive
- Charles Bonnet syndrome:
- As Macular Degeneration can prevent the brain from receiving visual stimulation, the brain can sometimes compensate by creating fantasy images. This is known as hallucination
- The hallucinations may include unusual patterns or shapes, animals, faces, or even an entire scene
- They may be either in black and white or in color, and may last from a few minutes to several hours. They images are usually pleasant; although in some cases, they may be scary to experience
- Individuals with Charles Bonnet syndrome may not report these experiences to their physicians, because they worry that it may be a sign of some sort of a mental disorder
- However, the hallucinations associated with this syndrome are the result of a vision problem and are not a reflection of one’s mental state
How is Macular Degeneration Treated?
Following are the treatment measures for Macular Degeneration:
- Progression of this disease can be prevented by taking dietary supplements, rich in antioxidants (vitamins A and C, copper, and zinc). A variety of colorful fruits and vegetables may be included into one’s diet. Also, the use of healthy fat in food, like olive oil, and the avoidance of bad fat (like butter) is beneficial
- Consuming foods rich in omega 3 fatty acids that are protective for the eyes. These are found in fishes like salmon, tuna, and in walnuts
- Smoking cessation is advised in order to prevent progression of the disease
- Individuals with Age Related Macular Degeneration may benefit from the use of low vision aids, like hand held magnifiers for reading, and specially designed glasses with telescopes incorporated into it, to view distant objects. Also, telescopic lens implantation into one of the eye is an option for the affected individual
- Medications, such as anti VEGF (vascular endothelial growth factor) drugs: These are medications that block VEGF (vascular endothelial growth factor), which is responsible for the growth of abnormal blood vessels into the eye. Such medications include pegaptanib (macugen), Bevacizumab (Avastin), Ranibizumab (Lucentis, formerly RhuFab), etc.
- Laser therapy: A laser beam is used to destroy abnormal blood vessels in the back of the eye. However, it can produce scarring of that part of the eye, as a side effect, which can even lead to a permanent loss of vision in that eye part. Even though there is a side effect to laser therapy, it can help save vision in other eye parts
- Photodynamic therapy: A light-activated drug, called verteporfin (Visudyne), is given through a blood vessel and a specially-designed laser is used to close the abnormal vessels, while leaving the retina intact
How can Macular Degeneration be Prevented?
The following factors can prevent or slow the progression of Macular Degeneration:
- Stopping smoking
- Multivitamin supplementation
- Intake of fish or fish oil supplement
- Including fruits and nuts in one’s diet
- Intake of a diet rich in green leafy vegetables and fresh fruits, which is less in carbohydrates and ‘bad’ fat
- Having a regular eye checkup, especially after the age of 40 years
- Wearing sunglasses and wide-brimmed hats, while outdoors, to protect from the sun’s UV rays
- Undertake regular exercising and weight control, to manage high blood pressure and cholesterol
What is the Prognosis of Macular Degeneration? (Outcomes/Resolutions)
The prognosis depends on the type of Macular Degeneration.
- Generally, the dry type of Macular Degeneration has a good prognosis, because the disease progression is slow and it may take years to worsen. However, the dry type can gradually progress and later become the wet type
- Wet type of Macular Degeneration has poor prognosis, since it is associated with the sudden loss of vision. If an individual has Macular Degeneration in one eye, then it is more likely to affect the other eye too
Additional and Relevant Useful Information for Macular Degeneration:
The United States has a support group for Macular Degeneration in every state. It is known as the American Macular Degeneration Foundation (AMDF).
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.