What are the other Names for this Condition? (Also known as/Synonyms)
- Clinical Hemoglobin C
- Haemoglobin C-C Disease
- Homozygous for Hb C
What is Hemoglobin C Disease? (Definition/Background Information)
- Hemoglobin C Disease, or Hb C Disease, is an inherited blood disorder that is marked by the presence of an abnormal hemoglobin type, known as hemoglobin C
- Hemoglobins are iron-rich, oxygen transporting proteins, found in the red blood cells. Those with Hb C may suffer from mild hemolytic anemia. Hemolysis means a breakdown of red blood cells. This leads to a depletion of red blood cells in the blood, causing anemia
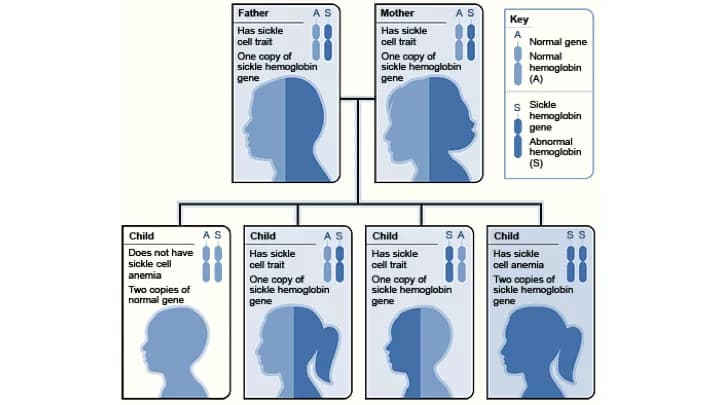
- The disorder is an autosomal recessive condition; implying that the defective genes are transferred to the child by both the parents
- Management of the condition involves treating anemia (if required); otherwise no specific treatment is required
Who gets Hemoglobin C Disease? (Age and Sex Distribution)
- Hemoglobin C Disease affects the newborn child. It is present at birth, but sometimes not discovered until a much later period, usually adulthood
- No male-female gender inequality is observed
- The disease is endemic to some ethnic groups and found in certain geographical regions of the world, like African-Americans (in the US), Hispanics, few regions of North Africa, and individuals of Italian, Greek, and Caribbean ancestry
What are the Risk Factors for Hemoglobin C Disease? (Predisposing Factors)
The risk factors for Hemoglobin C Disease include:
- Hb C Disease runs in the families and hence, children born in families with a medical history of the condition are at risk
- Individuals having consanguineous partners/spouses have the greatest risk
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Hemoglobin C Disease? (Etiology)
- Genetic mutations are said to cause Hemoglobin C Disease. The reason behind the mutations and the exact mechanism of how hemoglobins are affected, is under study research
- Both parents have to be affected with, or be carriers of the defective genes, for their offspring to be affected with Hb C Disease. This feature is known as autosomal recessive
What are the Signs and Symptoms of Hemoglobin C Disease?
Hemoglobin C Disease is a generally mild condition and most individuals are asymptomatic. Nevertheless, the following signs and symptoms may be noted, in some individuals:
- Mild hemolytic anemia; usually aggravated during infection/illness
- Yellowing of the eyes, jaundice (rare)
- Streaks in the eye, due to retinal damage
- A few individuals may develop gallstones, which may have to be treated
- Enlarged spleen (splenomegaly)
- Pain in the bones and muscles (sometimes)
- Dental tissue impairment
- Reduced red blood cells could render the body vulnerable for opportunistic infections
How is Hemoglobin C Disease Diagnosed?
Diagnosis of Hemoglobin C Disease is made by:
- Physical exam with evaluation of family medical history of the newborn/child
- Blood test; total blood count
- Hemoglobin analysis
- Genetic mutation testing
- Oral, eye examination
- Abdominal ultrasound
- Differential diagnosis to eliminate other conditions, since there are several causes for anemia
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Hemoglobin C Disease?
A few complications caused by Hemoglobin C Disease include:
- Gallbladder disease; formation of gallstones
- Spleen enlargement
- Severe anemia due to parvovirus infection
- Acute damage of the retina
How is Hemoglobin C Disease Treated?
Mild symptoms are generally the norm with Hemoglobin C Disease; severe conditions resulting in severe complications are infrequent. The management measures include:
- Most individuals do not require any treatment for the disease; they lead a normal life
- To treat anemia; folic acid, or other suitable supplementations are used
- Cholecystectomy (removal of gallbladder) is performed, if necessary
- Laser treatment for eye problems
- Dental support and treatment, if required
- Partial or complete removal of spleen (splenectomy); this procedure is performed only in rare cases
How can Hemoglobin C Disease be Prevented?
- Currently there are no specific methods or guidelines to prevent Hemoglobin C Disease genetic condition
- Genetic testing of the expecting parents (and related family members) and prenatal diagnosis (molecular testing of the fetus during pregnancy) may help in understanding the risks better during pregnancy
- If there is a family history of the condition, then genetic counseling will help assess risks, before planning for a child
- Active research is currently being performed to explore the possibilities for treatment and prevention of inherited and acquired genetic disorders
What is the Prognosis of Hemoglobin C Disease? (Outcomes/Resolutions)
- Hemoglobin C Disease is one of the mildest forms of hemoglobin-related disorders. Most individuals lead a normal life, with full life expectancy
- Symptomatic treatment (with surgical intervention) is required for those with acute conditions of anemia, gallstones, eye, dental health, and spleen problems. Despite these problems, the prognosis is generally good
- Hb C Disease may lower the red blood cell count and make the body susceptible to opportunistic infections, which could further lead to more severe hemolytic anemia
Additional and Relevant Useful Information for Hemoglobin C Disease:
- Hemoglobin C Disease occurs sometimes, together with Hemoglobin SC Disease (Sickle Cell Hemoglobin Disease). The combined effect of these two disorders may increase the intensity of the symptoms
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.