What are the other Names for this Condition? (Also known as/Synonyms)
- Hallux Limitus
- Stiff Big Toe (due to Hallux Rigidus)
- Stiff Great Toe (due to Hallux Rigidus)
What is Hallux Rigidus? (Definition/Background Information)
- Hallux Rigidus (or Stiff Big Toe) is a degenerative form of arthritis that can cause pain and stiffness to the joint; chiefly the metatarsophalangeal (MTP) joint, at the base of the big toe
- Individuals, who develop Hallux Rigidus may begin to experience severe pain, while performing certain daily activities, such as walking, climbing, and standing
- Studies have indicated that Hallux Rigidus may have a genetic component. Overall, adult men are more likely to develop the condition, than adult women
- Treatment associated with the condition includes both nonsurgical and surgical methods.
Who gets Hallux Rigidus? (Age and Sex Distribution)
- Hallux Rigidus may occur in individuals of all ages, races, ethnic groups, or gender
- Overall, adult males between the ages of 30-60 years, have the highest rate of occurrence
What are the Risk Factors for Hallux Rigidus? (Predisposing Factors)
Common risk factors associated with Hallux Rigidus include:
- A previous injury to the big toe
- Individuals, who participate in sports that cause a repetitive stress on the big toe, such as running
- Individuals, who have a family history of Hallux Rigidus, may have an increased risk of the condition
- Gout
- Flatfeet
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Hallux Rigidus? (Etiology)
Causes of Hallux Rigidus include:
- Any activity that causes a repetitive stress on the big toe, such as running
- Abnormal muscle imbalance in the foot: There are multiple muscles in the foot that are involved in their proper function. If one of the muscles is weakened or injured, then it causes an imbalance in functioning of rest of the muscles
- Presence of flatfeet
- Inflammatory or autoimmune disorder (such as rheumatoid arthritis)
- Degenerative joint disease (osteoarthritis)
- Gout: A medical condition caused by a high level of uric acid in blood
- Individuals with a family history of Hallux Rigidus
What are the Signs and Symptoms of Hallux Rigidus?
Signs and symptoms of Hallux Rigidus include:
- Pain and stiffness of the big toe, while running, walking, standing, or climbing stairs; pain that is enhanced by cold weather
- Difficulty bending the big toe
- Decreased range of motion of the big toe
- Swelling and inflammation in the first metatarsophalangeal joint
How is Hallux Rigidus Diagnosed?
Diagnostic methods that a physician may use to help diagnose Hallux Rigidus include:
- Physical examination: A physician can usually diagnose Hallux Rigidus after performing a thorough physical examination of the big toe. The physician examines the foot for evidence of bone spurs and may test the range of motion of the MTP joint. In addition to this, a complete medical history can aid in arriving at a definitive diagnosis
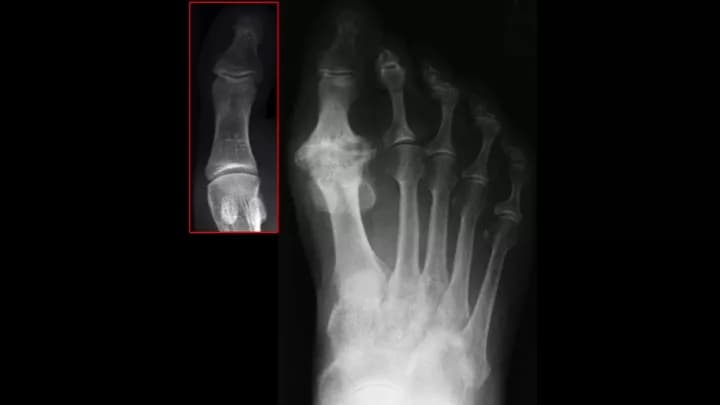
- X-ray of foot: X-rays use radiation to produce images of the big toe. It can also help the physician rule out other possible causes for discomfort, such as the presence of arthritis, and the location of any bone spurs
- MRI of the foot: To detect soft tissue abnormalities
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Hallux Rigidus?
Complications associated with Hallux Rigidus include:
- Bunions of the big toe
- Prolonged stiffness of the big toe
- Fibrosis, due to severe degenerative arthritis, which can cause a frozen metatarsophalangeal joint
How is Hallux Rigidus Treated?
Treatments for Hallux Rigidus include both nonsurgical and surgical methods.
Nonsurgical treatments methods for Hallux Rigidus include:
- Applying ice to the foot can help reduce pain, inflammation, and control symptoms
- Use of well-padded custom-made shoe inserts, to relieve pain and help reduce pressure on the toe. A physician may recommend shoe modifications to help decrease stresses on the big toe
- Non-steroidal anti-inflammatory oral medications, such as indomethacin and naproxen, may be used to treat Hallux Rigidus. These medications can help decrease the pain and swelling
- Corticosteroid injections into the metatarsophalangeal joint space help provide temporary relief of symptoms and in improving the range of motion. It is important to note that corticosteroid injections only give temporary relief. Prolonged episodes of such injections, may injure the joints in the long-run
- Individuals are likely to need physical therapy exercises, after the cast is removed. The goal of these exercises is to strengthen the muscles within the foot, improve flexibility, and decrease stiffness
Surgical intervention methods for Hallux Rigidus include:
- Cheilectomy for Hallux Rigidus: Cheilectomy is a surgical procedure that involves removing bone spurs from the base of the big toe
- Arthrodesis of the foot for Hallux Rigidus: Arthrodesis is a surgical technique that involves the removal of the damaged cartilage surrounding the metatarsophalangeal joint, within the big toe. After the damaged cartilage is removed, the two surrounding bones are fused together. Surgical hardware (such as plates, screws, or rods) is then used to stabilize the bones into a permanent position
- Total foot arthroplasty for Hallux Rigidus: Total foot arthroplasty involves the complete removal of the cartilage within the joint. The metatarsophalangeal joint at the base of the big toe is then removed and replaced by a metal and plastic prosthetic implant. This procedure is recommended, if Hallux Rigidus affects the entire joint
How can Hallux Rigidus be Prevented?
Common recommendations to help prevent Hallux Rigidus include:
- Individuals, who participate in any high-risk sports, such as football, should wear appropriate safety equipment to help prevent a serious injury
- Minimize any physical activity that causes a repetitive stress on the foot, especially if it starts hurting the great toe joint
What is the Prognosis of Hallux Rigidus? (Outcomes/Resolutions)
The long-term prognosis of Hallux Rigidus depends on the severity of the degenerative disorder.
- If Hallux Rigidus is treated early and aggressively, the prognosis is good in a majority of the individuals
- In general, without treatment measures, a high percentage of individuals, who develop Hallux Rigidus may experience a lifetime of gradual degeneration associated with this debilitating disorder. In such individuals, prognosis for Hallux Rigidus is poor.
Additional and Relevant Useful Information for Hallux Rigidus:
Active research is being undertaken to understand the processes involved in the development of Hallux Rigidus. This includes specific studies to understand, why some individuals continue to have severe Hallux Rigidus, in spite of treatment.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.