What are the other Names for this Condition? (Also known as/Synonyms)
- Dermal Epithelial Inclusion Cysts
- Squamous Epithelial Dermal Inclusion Cysts
- Squamous Inclusion Cysts of Skin
What is Epithelial Inclusion Cysts of Skin? (Definition/Background Information)
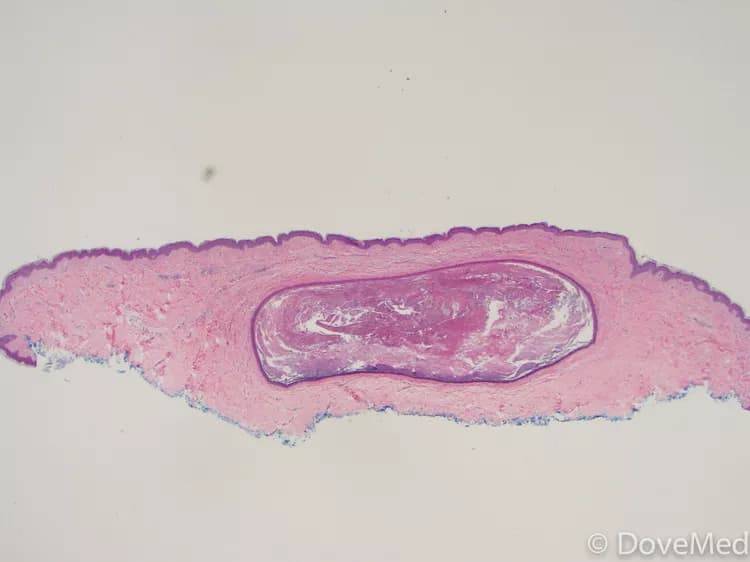
- Epithelial Inclusion Cysts of Skin is a type of dermal or skin cyst that forms due to entrapment of the surrounding epithelial tissue. It is a benign cyst that is lined by stratified (non-keratinizing) squamous epithelium, when observed under a microscope by a pathologist
- There are no clearly established risk factors, but Epithelial Inclusion Cysts of Skin are known to form due to trauma to the skin (such as due to an accident or a surgery). Hence, these are also known as Traumatic Epithelial Inclusion Cysts of Skin
- Most of the cysts appear as solitary mucin-filled lesions and are painless. No significant signs and symptoms or complications are typically noted. However, in some cases, Epithelial Inclusion Cyst of Skin may cause tenderness, pain, and discomfort
- Treatment course includes close observation of the tumor in asymptomatic cases and surgical management, if necessary. In general, the prognosis of Epithelial Inclusion Cyst of Skin is excellent with adequate treatment
Who gets Epithelial Inclusion Cysts of Skin? (Age and Sex Distribution)
- Epithelial Inclusion Cysts of Skin are observed in wide age range of individuals. They may be observed in both adults and children
- There is no known geographical, ethnic, or racial preference
What are the Risk Factors for Epithelial Inclusion Cysts of Skin? (Predisposing Factors)
No definitive risk factors have been identified for Epithelial Inclusion Cysts of Skin. However, they may occur due to the following factors:
- Trauma to the skin due to an injury, cut, bruise, or wound
- Any invasive procedure (such as a minor surgery or piercing)
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Epithelial Inclusion Cysts of Skin? (Etiology)
- Epithelial Inclusion Cysts of Skin are caused by displaced epithelium that occurs due to variety of factors including trauma and abnormal congenital epithelial remnants during fetal growth and development
- Surgical trauma is also an important causative factor
What are the Signs and Symptoms of Epithelial Inclusion Cysts of Skin?
A majority of the cysts may be asymptomatic, presenting no significant signs and symptoms. In some cases, the following signs and symptoms of Epithelial Inclusion Cysts of Skin may be noted:
- Presence of a single cyst that is normally filled with fluid (usually mucin or keratin); the cysts may be also sometimes filled with pus, air, or other cell remnants
- The cyst is soft and usually well-defined; it may occur as a polyp on the skin
- Any part of the body may be affected; the cyst usually forms at the site of skin injury
- The cysts may be of varying sizes; most cysts are small (less than 1 cm), while some may grow to larger sizes
- An area of redness and inflammation may be observed; there may be an absence of pain
- Large sizes may cause discomfort and pain
How is Epithelial Inclusion Cysts of Skin Diagnosed?
A diagnosis of Epithelial Inclusion Cysts of Skin may involve the following steps:
- Evaluation of the individual’s medical history and a thorough physical examination. Usually, a visual exam by the healthcare provider is sufficient to ensure a diagnosis of the condition
- Dermoscopy: It is a diagnostic tool where a dermatologist examines the skin using a special magnified lens
- Wood’s lamp examination: In this procedure, the healthcare provider examines the skin using ultraviolet light. It is performed to examine the change in skin pigmentation
- Additional tests may be necessary to rule out any underlying condition, if any
- Skin biopsy: A skin biopsy is performed and sent to a laboratory for a pathological examination. The pathologist examines the biopsy under a microscope. After putting together clinical findings, special studies on tissues (if needed) and with microscope findings, the pathologist arrives at a definitive diagnosis
Note: In a majority of cases, a tissue biopsy is necessary only to rule out other conditions presenting similar signs and symptoms.
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Epithelial Inclusion Cysts of Skin?
No significant complications of Epithelial Inclusion Cysts of Skin are noted, because it is a benign condition. However, the following may be observed in some cases:
- Cosmetic concerns, especially if the cysts are present on the face, neck, or at other prominent locations
- Abscess formation resulting in infections; this may result in associated signs and symptoms including fever
- The cysts may rupture and bleed resulting in secondary infections; this may also result in scar formation
- Damage to the muscles, vital nerves, and blood vessels, during surgery
- Post-surgical infection at the wound site is a potential complication
- Recurrence of the cyst
How is Epithelial Inclusion Cysts of Skin Treated?
Treatment measures for Epithelial Inclusion Cysts of Skin may include the following:
- Some cysts are known to subside and spontaneously regress on their own
- If there are no symptoms, then the healthcare provider may advise a ‘wait and watch’ approach, following the diagnosis of a epithelial inclusion cyst
- Application of topical creams and gels, to bring relief from the symptoms and to provide a measure of comfort
- Stoppage of soaps and body creams that have strong chemicals in them; use of milder alternatives
- Avoidance of synthetic and tight-fitting clothes for a period of time
- Maintain proper personal hygiene
- In some cases, the cysts may get secondarily infected. If bacteria is the cause of infection, it may be treated through antibiotics
- If the antibiotics does not clear the infection, then an abscess drainage through a surgical procedure may be performed
- Surgical intervention with complete excision can result in a complete cure and address any cosmetic concerns
- Post-operative care is important: Minimum activity level is to be ensured until the surgical wound heals
- Follow-up care with regular screening and check-ups are important
How can Epithelial Inclusion Cysts of Skin be Prevented?
Current medical research has not established a method of preventing Epithelial Inclusion Cysts of Skin.
- Ensure good personal hygiene
- Avoid picking, scratching, or popping the blisters/cysts
- Avoid tight-fitting dress and dress made of synthetic material until the cysts heal
What is the Prognosis of Epithelial Inclusion Cysts of Skin? (Outcomes/Resolutions)
The prognosis of Epithelial Inclusion Cysts of Skin is excellent with surgical intervention (surgical removal through simple excision), since these are benign lesions.
Additional and Relevant Useful Information for Epithelial Inclusion Cysts of Skin:
- Dermal Epithelial Inclusion Cyst is not an infectious condition and it does not spread from one individual to another
- There is no definitive proof that certain types of diet may influence its development
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.