What are the other Names for this Condition? (Also known as/Synonyms)
- Convulsions
- Seizure Disorder
What is Epilepsy? (Definition/Background Information)
- Epilepsy is a temporary disruption of brain function, due to excessive, abnormal discharge of nerve cells (neurons). The main signs of Epilepsy are seizures, and hence, the condition is also termed a Seizure Disorder
- An epileptic seizure, or simply a seizure, is a sudden, abnormal, and uncontrolled electrical disturbance in the brain disrupting normal brain activity. This may last from a few seconds to even a few minutes
- The clinical manifestation of a seizure depends on the specific region and extent of brain involvement. It may include an alteration in alertness to complete loss of awareness and shaking movements. There are different types of seizures and individuals with Epilepsy may have more than a single type of seizures
- Epilepsy is the condition of recurrent (two or more), unprovoked seizures that take place in an interval of 24 hours or more. It is not a mental illness, but a physical problem that occurs in the brain affecting the central nervous system. It is a chronic neurological disorder that may be caused by a variety of factors such as brain injury, stroke, brain tumor, or genetic conditions
- It is important to note that not all individuals with seizures have Epilepsy. Seizures may be provoked due to other underlying conditions such as hypoglycemia, high fever, or substance withdrawal
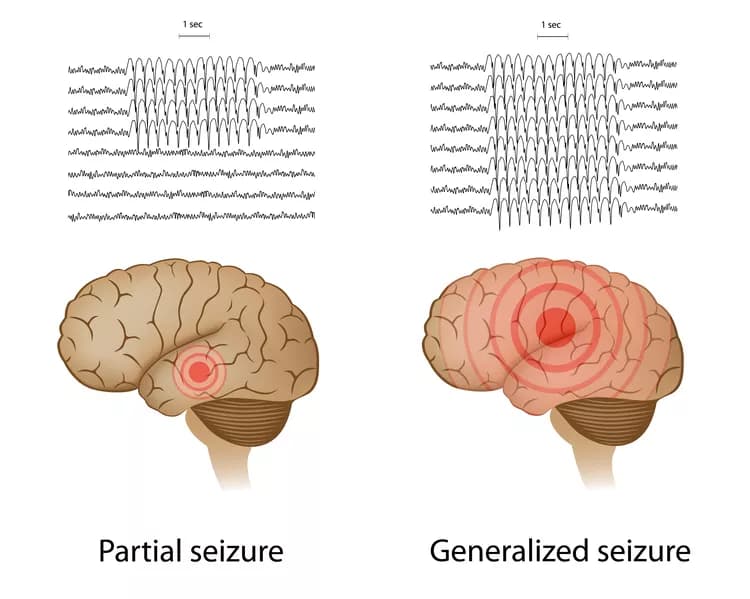
Epilepsy is classified as generalized and focal.
- Primary generalized seizure or idiopathic Epilepsy (cause unknown) is an Epilepsy type, where the whole brain is involved and there is a loss of consciousness. There is no focal point where epileptic discharge begins. It may consists of the following:
- Childhood absence Epilepsy
- Juvenile myoclonic Epilepsy
- Tonic-clonic seizures
- Atonic seizures
- Clonic seizures
- Focal seizures or partial seizures: As the name implies, this is a seizure that is focal to one part of the body. For instance, an individual may have a seizure that is limited to just to an arm or a leg. Partial seizures can either be simple (intact consciousness) or complex (loss or alteration of consciousness)
Tonic-clonic seizure is a generalized seizure with varying phases of muscle rigidity, followed by jerking of the body muscles for several minutes.
Absence seizure: This type of seizures occurs in children. Here, consciousness is only briefly impaired, the individual often remains upright, gives a normal appearance, or would appear to be staring into vacant space.
Who gets Epilepsy? (Age and Sex Distribution)
- According to current information, about 60 million people around the world have Epilepsy, at any one time. Every year, there are 30-50 new cases of Epilepsy per 100,000 people
- Epilepsy is more likely to occur during childhood and after the age of 55 years. However, Epilepsy may occur at any age. It is a very common condition affecting the brain
- Per medical literature, the current gender breakdown with respect to occurrence of the condition is 48% female and 52% male
What are the Risk Factors for Epilepsy? (Predisposing Factors)
Common risk factors of Epilepsy include:
- Age: The most frequent onset of Epilepsy is during early childhood and in the elderly adult phase. During neonatal period and early infancy, the most common causes include congenital brain abnormalities, brain infections, trauma, and metabolic disorders
- Head trauma: Any deep injury to the brain puts one at a risk for Epilepsy. Older adults have an increased risk due to falls
- Brain stroke: A medical condition that occurs when blood supply to the brain is reduced or blocked, resulting in oxygen deprivation to the brain tissue. Two major categories of brain stroke based on cause include, those caused by blood blockages (ischemic), and those caused by bleeding into the brain (hemorrhagic)
- Dementia: It is a type of brain disorder accompanied by a collection of symptoms that indicate brain impairment and loss of brain function. It leads to a progressive decline of all cognitive aspects, such as behavior, memory, attention, analytical ability, thinking, language skills, etc. It can increase the risk of Epilepsy in older adults
- Brain infections: A brain abscess is a collection of infected material within the brain tissue acting as a space-occupying lesion. It can cause fever, vomiting, seizures. Encephalitis leads to brain inflammation; serious symptoms of which include, confusion and seizures
- Degenerative brain diseases are caused by the decline of the nerve cells of the nervous system. It is commonly seen in the elderly group. Genetics play an important role in the development of degenerative brain disease
- Congenital conditions: Children with Down syndrome, Angelman's syndrome, or tuberous sclerosis can present with seizures
- Family history: The risk of Epilepsy increases if there is a history of the condition in the family. Childhood Epilepsies, like childhood absence Epilepsy and juvenile myoclonic Epilepsy may be passed on from a parent to a child
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Epilepsy? (Etiology)
- In adulthood, causes are more likely to be secondary to any brain lesion. Actually, some Epilepsies may develop slowly over time, in reaction to a trauma, illness, or some other occurrence, much earlier in life
- In older adults brain tumors, head trauma, and degenerative diseases, like dementia can cause seizures
- Illness and stress are just a few of the triggers that can set-off Epileptic seizures
- It is reported that in nearly 65% of the cases, the cause of Epilepsy may be unknown (idiopathic Epilepsy)
Common causes of Epilepsy include:
- Stroke or a transient ischemic attack (TIA)
- Degenerative brain diseases, such as Alzheimer's disease and Lewy body dementia
- Traumatic brain injury (TBI)
- Infections such as brain abscess, meningitis, encephalitis, Zika virus infection, HIV infection and AIDS
- Brain-related disorders that are present at birth
- Brain injury that occurs during or around the time of birth
- Metabolism disorders present at birth such as phenylketonuria
- Brain tumors (benign or malignant)
- Abnormal blood vessels in the brain (including vascular malformations)
- Use of certain medications, such as antidepressants, cocaine, and amphetamines
- Congenital (genetic) disorders such as Down syndrome
- Complications during pregnancy from a lack of nutrition, deficient oxygen to the fetus, or infections affecting the mother
- Developmental disorders such as autism
What are the Signs and Symptoms of Epilepsy?
The signs and symptoms of Epilepsy vary from one individual to another and may be mild or severe. It depends on the part of the brain that is affected. These include:
- Some individuals may have brief unresponsive, staring spells or temporary confusion, while others may have violent shaking and loss of consciousness
- Some individuals observe strange sensations of ringing, machine-like sounds, unpleasant odor (such as burning rubber or sulfur), without the loss of consciousness. This is called an aura, the mildest kind of seizure. Usually, an aura is a warning sign that another type of seizure, is about to follow
- Stiff or jerking-like movements or unnatural posturing of the body, arms, or the legs; stiff muscles
- Body disturbances: These can include pallor, increased blood pressure, increased heartbeats, goose bumps, excess secretion of tears, dilated pupils, or even vomiting
- Amnesia, when individuals experience impaired consciousness during seizures , but are unaware of it afterwards, or are unable to recall activities that occurred during or shortly after the seizure occurred
- Febrile seizures are commonly observed during early childhood
- Fear and anxiety
How is Epilepsy Diagnosed?
Whenever an individual experiences symptoms of an Epileptic seizure, physicians try to evaluate the cause. Sometimes, the seizure is a sentinel event, pointing toward serious underlying conditions, such as brain tumor or stroke that requires immediate attention. In some cases, the causal factor can be treated; and if the cause is found and fixed/controlled, the Epilepsy may disappear.
- Physical exam with a comprehensive evaluation of medical history
- Neurological and cognitive assessment: Checking intellectual ability, memory, mental health and function, language skills, judgment and reasoning, coordination and balance, reflexes, sensory perceptions (space, sight, hearing, touch)
- Psychiatric examination; neuropsychological tests
- Blood tests, like total blood count, blood chemistry, glucose, ammonia, blood gas analysis, electrolytes, vitamin levels, to check for signs of infections, genetic conditions, etc.
- Electroencephalogram (EEG) has become the preeminent tool in the diagnostic evaluation of Epileptic patients. It records the electrical activities of the brain
- Computerized tomography (CT) scan of the head
- MRI of the brain
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Epilepsy?
Complications due to Epilepsy could include:
- Trauma/injury: Seizures can lead to accidents and fall injuries affecting the head, cause bone fractures, or result in drowning
- Status Epilepticus is a seizure that lasts longer than normal. A time duration of 30-60 minutes is generally considered a minimum requirement for usage of the term Status Epilepticus, to describe the condition. It is considered a serious life-threatening condition and is a medical emergency
- Psychological issues, especially depression, anxiety, and in some cases, suicidal tendencies are noted. The overall quality of life may be affected
- Social stigma and discrimination, observed in some parts of the world
- Complications during pregnancy: There is a potential for reduction in fertility. Seizure episodes may also adversely affect the mother and child. Certain anti-epileptic medications can increase the risk for birth defects
- Sudden unexplained death in Epilepsy (SUDEP): This phenomenon is not well understood but could be related to disturbances in the heart's rhythm from a seizure or due to breathing problems. SUDEP may be noted in those with major and uncontrolled seizures
How is Epilepsy Treated?
The objective of Epilepsy drug therapy is the ‘daily’ prevention of symptoms. Medications are not known to cure Epilepsy but helps to suppress the symptoms so that individuals may go about their regular/normal life.
- A number of medications are effective; the choice of medication is based on the healthcare provider’s assessment of the condition. Drugs that may be prescribed include phenytoin, valproic acid, and carbamazepine
- The choice of antiseizure drugs and the way they are prescribed/used differs in children and adults. Often, a child's first seizure is not treated with medication, since the seizure may be an isolated event that may not repeat
- Ethosuximide is the best therapy for absence seizures.
- Febrile seizures or benign focal seizures are low-risk and do not call for drug intervention
- Antiepileptic drugs usage is not initiated in case of single seizures. Exceptions to this include:
- Status Epilepticus
- The presence of focal neurological signs, like limb paralysis, memory loss, confusion, deafness, loss of vision, etc.
- Abnormal EEG or lesion on CT scan of head
- Family history of seizures
Sometimes, medications are started, right after the first seizure. In other cases, the physician may recommend a wait and watch approach, before prescribing drug therapy. Generally, the use of medication is indicated, when Epilepsy is present and seizures are recurring. The physician determines the right drug, or combination of drugs, for each individual.
- If seizures are not controlled with a single agent, the use of alternatives (medications) may be resorted to. If seizures are still not controlled, a second drug may be administered
- Vagus nerve stimulation can assist in interrupting a potential seizure. It calls for the implantation (under general anesthesia) of a small generator in the upper left area of the chest. Patients, who experience warning signs before seizures occur, can initiate the generator's action themselves, by waving a magnet over the area where the generator is implanted
- Surgery: If multiple medications do not control the seizure, surgical correction of a seizure focus may lead to resolution of recurrences. If a patient’s seizure symptoms, EEG, and MRI tests, do not indicate focal epilepsy, then in such cases, the use of surgery may not be beneficial
Some individuals may be recommended a ketogenic diet, a low carbohydrate high fat diet, where fats instead of carbohydrates are burned for energy purposes, as part of Epilepsy treatment.
How can Epilepsy be Prevented?
The following measures may be considered towards preventing or lowering one’s risk for an Epilepsy:
- Lead a healthy life to minimize the risk for cardiovascular disease and stroke; avoid smoking and excess drinking
- Wear seat belts and helmets to prevent head injuries from accidents or participation in sports, which is a common cause of Epilepsy
- Avoid the use of illegal drugs
- Always talk to your physician, if you have any concerns about medication side effects, or dosages. Do not attempt to make any changes to your drug regimen without speaking first with your doctor
- Pregnant women are advised proper prenatal and postnatal medical care
- Take all necessary vaccinations
- Take adequate precautions to lower brain infection risks such as via proper handwashing and avoiding contact with individuals having infections
- Individuals with Epilepsy are advised to take their medications regularly, lower stress, get adequate rest, and recognize their seizure triggers (also maintain a record of seizures)
What is the Prognosis of Epilepsy? (Outcomes/Resolutions)
- The cause of Epilepsy may not be often well-understood. However, it is believed that with prompt identification and treatment of the condition, the outcome is better/improved
- According to the World Health Organization, nearly 70% of the epileptic individuals can become seizure-free if treated appropriately using antiseizure medications
- If the seizures are caused by other medical conditions/disorders, then treatment of the primary cause is key to its prevention
- Most women with Epilepsy have normal pregnancies. It is always important to supplement one’s diet with multivitamins and folic acid, long before planning for a child
- Previously, when seizures occurred, there was often fear, embarrassment, and helplessness. However, presently there are various treatment medications that help individuals cope with Epilepsy
It is noted that the risk for premature mortality is increased by a factor of 3 in individuals with Epilepsy when compared to the general population.
Additional and Relevant Useful Information for Epilepsy:
There are voluntary organizations and support groups that provide help, encouragement, and understanding, to the individuals (and their families) affected by Epilepsy.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.