What are the other Names for this Condition? (Also known as/Synonyms)
- Allergic Esophagitis
- EoE (Eosinophilic Esophagitis)
- Non-Reflux Esophagitis
What is Eosinophilic Esophagitis? (Definition/Background Information)
- Eosinophilic Esophagitis (EoE) is a specific form of inflammation of the food pipe (esophagus) that is not an infection and is not related to acid reflux (Gastroesophageal Reflux Disease, or GERD).
- The condition derives its name from a certain type of inflammatory cell (eosinophil) that is markedly increased in the esophageal inner lining (mucosa).
- The reason why, such an inflammation occurs is not clearly known; but, it is suspected to be an allergy (or sensitivity), because eosinophils are often associated with allergies.
- It is suspected that the allergy may be towards certain foods; with different individuals having differing food allergies
- Eosinophilic Esophagitis is a relatively recent disorder (mid-1990s).
Who gets Eosinophilic Esophagitis? (Age and Sex Distribution)
- Although it may be seen at any age, young adults (late teens, individuals in their 20s and 30s) are most often affected
- In most studies, Eosinophilic Esophagitis occurred more commonly in males, than in females
- All races and ethnic groups seem to be equally affected by this disorder. There is also no worldwide geographical restriction observed, for this disorder
What are the Risk Factors for Eosinophilic Esophagitis? (Predisposing Factors)
There are no definitely known risk factors for Eosinophilic Esophagitis, but the following are suspected:
- A history of allergies in general (atopy)
- A known food allergy
- A history of choking on food (food impaction)
- A history of difficulty in swallowing (dysphagia)
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Eosinophilic Esophagitis? (Etiology)
- The cause of Eosinophilic Esophagitis occurrence is unknown
- Most likely, it is due to an allergic reaction to certain food(s), which takes place in the esophagus
What are the Signs and Symptoms of Eosinophilic Esophagitis?
Signs and symptoms of Eosinophilic Esophagitis include:
- The most consistent symptom is difficulty in swallowing (dysphagia)
- The food may get stuck in the esophagus (food impaction) and the patient may need emergency medical aid, to have it removed
- Sometimes, swallowing difficulties may be associated with nasal (sinusitis) and respiratory (asthma) allergies
- There may be weight loss due to less food intake, related to dysphagia
- Failure to thrive in children
- Occasionally, there are no symptoms at all. In such cases, the condition is diagnosed by incidental endoscopic findings and pathological diagnosis, on a biopsied tissue. The esophagus also looks abnormal on endoscopic examination
- Narrowing of the esophagus (stricture), particularly in the middle of its length
How is Eosinophilic Esophagitis Diagnosed?
An Eosinophilic Esophagitis diagnosis is made by combined clinical, endoscopic, and pathological findings. Patients with symptoms of dysphagia or food impaction undergo further examination.
- This may include radiographic imaging (barium x-ray), to demonstrate narrowing of the esophagus
- Endoscopic examination of the esophagus shows one or more of the following abnormalities: Rings, furrows, stricture, white spots or plaques
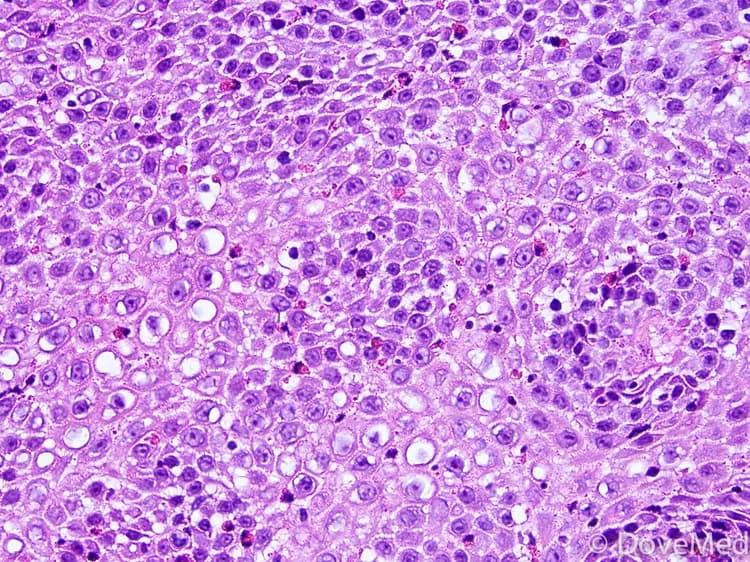
- Biopsy samples from the esophagus show the following abnormalities when examined by a pathologist under a microscope. The pathologist will find a marked increase in eosinophils (>20/hpf); the eosinophils are more toward the lumen, including eosinophil clusters or aggregates (micro-abscesses), and marked basal zone hyperplasia
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Eosinophilic Esophagitis?
Complications due to Eosinophilic Esophagitis could include:
- Choking on food, or food impaction may create an emergency, necessitating an endoscopy for removal
- The esophagus also becomes more prone to tearing or rupture, when dilatation (expansion or stretching) of the strictured (narrow) portion is attempted
How is Eosinophilic Esophagitis Treated?
Treatment of Eosinophilic Esophagitis includes dietary manipulations (exclusions or eliminations of certain foods), and/or the administration of topical steroids.
How can Eosinophilic Esophagitis be Prevented?
Preventive measures for Eosinophilic Esophagitis include:
- Adherence to dietary exclusions that are effective
- Management of allergies, in general
What is the Prognosis of Eosinophilic Esophagitis? (Outcomes/Resolutions)
- The majority of patients with Eosinophilic Esophagitis respond to dietary exclusions and topical steroids
- In such patients, the prognosis is excellent with a complete resolution of the prior endoscopic and pathological abnormalities
- A small number of patients do not respond and may require more aggressive management, including dilatation of the narrow esophagus
Additional and Relevant Useful Information for Eosinophilic Esophagitis:
- Earlier Eosinophilic Esophagitis was misdiagnosed as a form of severe gastroesophageal reflux disease (GERD), which did not respond to (GERD-specific) treatment. Now EoE is considered to be a separate disease process and not a severe form of GERD
- Some cases (having fewer eosinophils) may still be confused for GERD. In these, the diagnosis is often made by analyzing the signs, symptoms, and endoscopic findings
- Occasionally, both diseases (EoE and GERD) may co-exist, creating both diagnosis and treatment challenges
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.