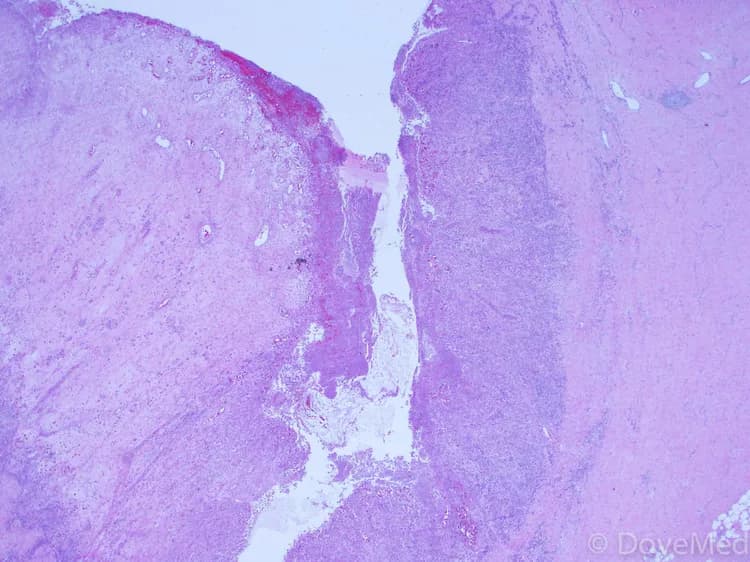
Diverticular Disease
What are the other Names for this Condition? (Also known as/Synonyms)
- Diverticulitis
- Diverticulosis
What is Diverticular Disease? (Definition/Background Information)
- Diverticular Disease is a condition that occurs in both the small and large intestine, when diverticula (sac-like protrusions) form on the intestinal walls. Generally, the large intestine (colon) is more affected than the small intestine
- Diverticula usually develop due to excessive muscle strain in the rectum, due to constipation; constipation usually occurring secondary to a low-fiber diet
- Obesity, lack of exercise, and an imbalanced diet can increase one’s risk of developing Diverticular Disease, which is typically observed in older adults
- The signs and symptoms of Diverticular Disease can include abdominal cramping and bloating, constipation, lower abdominal pain, rectal bleeding, and vomiting. A delay or lack of treatment could lead to severe complications that include intestinal perforation and abscess formation, which can destroy intestinal tissue
- Dietary modifications, lifestyle changes, surgery (for severe cases), and symptomatic treatment of Diverticular Disease can result in a good prognosis, when early diagnosis and treatment is provided
- Preventative measures to reduce the likelihood of developing Diverticular Disease include increasing the proportion of fiber in one’s diet, increasing fluid intake, regular exercise, and maintaining a proper weight
Who gets Diverticular Disease? (Age and Sex Distribution)
- Diverticular Disease can occur worldwide. The disease is most common in individuals above the age of 40. However, adults over the age of 80 years have the highest risk of developing the condition
- Prevalence by sex depends on the age:
- Age less than 50 years: Diverticular Disease is more common in males
- Age in between 50-70 years: It is slightly more common in females
- Age greater than 70 years: It is more common in females
What are the Risk Factors for Diverticular Disease? (Predisposing Factors)
Risk factors of Diverticular Disease include:
- Low-fiber diet and a diet that is high in red meat and fat content
- Lack of exercise
- Obesity
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Diverticular Disease? (Etiology)
Currently, the exact cause of Diverticular Disease is unknown. It is believed that a diet low in fiber can cause this condition.
- Fiber is found in many fruits and vegetables, and while it is not digestible by the body, it remains in the colon and absorbs water to provide bulk to the feces, making it easier to pass down
- Constipation is likely to occur, if a diet is low in fiber. Constipation causes the muscles to strain as the body attempts to pass stools, which can result in the formation of diverticula in the colon
- A diverticulum (plural diverticula) is a sac-like protrusion that develops in the colonic wall. If stool or bacteria get caught in these diverticula, diverticulitis (infection) can occur
- Diverticulosis is the presence of diverticula without inflammation, whereas diverticulitis is the presence of diverticula with accompanying inflammation. Often, diverticulitis leads to diverticulosis
What are the Signs and Symptoms of Diverticular Disease?
The signs and symptoms of Diverticular Disease can include, but are not limited to, the following:
- Abdominal cramps, bloating
- Constipation
- Blood in stool, rectal bleeding
- Pain in the lower abdomen, especially on the left side
- Fever
- Vomiting
- Changes in bowel habits
If Diverticular Disease is left untreated, many complications can arise including perforation (development of a hole in the colon) and peritonitis (infection in the abdominal cavity).
How is Diverticular Disease Diagnosed?
Diverticular Disease may be diagnosed using the following tools:
- Thorough evaluation of the individual’s medical history and a complete physical examination: An evaluation of medical history will determine, if there is the presence of predisposing factors such as lack of exercise, or a low fiber diet
- A digital rectal exam can be performed to feel for lumps and diverticula within the colon. In this procedure, a physician will insert a lubricated, gloved finger into the rectum
- A colonoscopy may be used to diagnose Diverticular Disease. During this procedure, a long, flexible tube with an attached video camera is inserted into the rectum and colon to image the insides of the body region. This can help determine if diverticula have formed
- Abdominal ultrasound and CT scan
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions in order to arrive at a definitive diagnosis.
What are the possible Complications of Diverticular Disease?
The complications associated with Diverticular Disease depend on the severity of the disease.
- Common complications include the formation of perforations (small tears) in the colon that can cause bleeding (and is a medical emergency)
- It is also possible for infections or blockages to develop in the colon, which can progress to cause serious illness or intestinal damage
- If the infection worsens, abscesses (localized collections of pus) formations may take place on the walls of the colon. These can swell and destroy colon tissue
- Recurrence of the condition on treatment
How is Diverticular Disease Treated?
Treatment options for Diverticular Disease depend on the severity of the disease.
- A common treatment option is to increase the amount of fiber in the diet. This may reduce symptoms of the disease and prevent complications from arising, as a high-fiber diet will help regulate bowel movements. It is recommended that one consume 20 to 35 grams of fiber each day
- Infections and inflammation can be treated using oral or IV antibiotics
- Percutaneous abscess drainage (PAD) can be done to drain small abscesses that are confined to a well-defined area
- In case of severe Diverticular Disease, a surgery may be recommended so that the abdomen can be cleaned and infections treated properly. If the condition occurs multiple times in an individual, then a portion of colon may be resected
Regardless of what treatment is received, follow-up care and regular screenings are important to ensure that Diverticular Disease does not progress or recur and cause acute complications.
How can Diverticular Disease be Prevented?
Preventive measures of Diverticular Disease can include:
- Increasing the proportion of fiber in one’s diet: It is recommended to increase the consumption of raw apples, peaches, pears, tangerines, broccoli, squash, carrots, Brussels sprouts, potatoes, kidney beans, whole-wheat bread, and brown rice
- Increasing fluid intake
- Exercising regularly and maintaining one’s weight
Despite the above, it is important to attend regular medical (and dental) checkups and screenings, so that Diverticular Disease can be detected early and properly treated.
What is the Prognosis of Diverticular Disease? (Outcomes/Resolutions)
- The prognosis of Diverticular Disease depends on the severity of the disease and how quickly a treatment plan is implemented. With suitable treatment, most individuals are able to fully recover from the condition
- When Diverticular Disease is not treated promptly, it could lead to more serious complications such as:
- Intestinal perforation: The development of a hole in the intestine when the diverticula burst
- Peritonitis: Infection of the abdominal cavity that can occur when perforation occurs and contents of the diverticula (feces) leak into the abdominal cavity
- It is estimated that approximately 50% of the individuals who develop Diverticular Disease will develop the condition again within a period of 7 years
Additional and Relevant Useful Information for Diverticular Disease:
Please visit our Digestive System Health Center for more physician-approved health information:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.