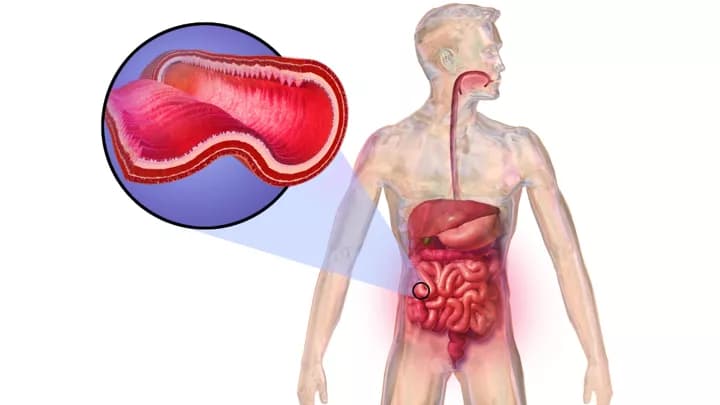
Crohn’s Disease
What are the other Names for this Condition? (Also known as/Synonyms)
- Granulomatous Colitis
- Regional Enteritis
- Terminal Ileitis
What is Crohn’s Disease? (Definition/Background Information)
- Crohn’s Disease is a condition in which there is chronic, long-standing inflammation of the gastrointestinal tract (gut). It is one of the two inflammatory bowel diseases (IBD), the other being ulcerative colitis
- This condition can affect any region in the gastrointestinal tract, but it most commonly (first) affects the ileum (ileitis)
- The gastrointestinal (GI) tract begins from the mouth, esophagus (food pipe), stomach, small intestine (that includes duodenum, jejunum, and ileum), large intestine, rectum, and ends in the anus
- The other sites that are involved in Crohn’s disease in decreasing order of frequency are the jejunum, duodenum, colon, esophagus, stomach, mouth, etc.
- It affects only the small intestine in 30% of the individuals, large intestine only in 20% of the individuals, and in the remaining individuals, it may affect multiple areas of the GI tract
- Currently, the exact cause and mechanism of Crohn’s Disease is unknown. It is a chronic long-standing illness that is associated with frequent flare-ups and symptom-free periods (remission). There is no cure for the condition
- However, the affected individuals can lead relatively normal lives with prompt treatment of flare-ups and frequent follow-up with the healthcare provider
Who gets Crohn’s Disease? (Age and Sex Distribution)
- Crohn’s Disease begins to manifest in older adolescents and younger adults. It is slightly more common in females
- It is more common in North America and Europe compared to other parts of the world
- It is more common in Caucasians, Jews, and individuals of African descent, than other races
What are the Risk Factors for Crohn’s Disease? (Predisposing Factors)
The risk factors of Crohn’s Disease include:
- Positive family history is seen in approximately 15% of the individuals
- Individuals living in temperate climates
- Studies show that individuals who have had their appendix removed are at a higher risk to get Crohn’s Disease
- Smoking
- Intake of high dietary fat
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Crohn’s Disease? (Etiology)
Currently, the exact cause and mechanism of Crohn’s Disease development is unknown. It is a chronic (long-standing) and relapsing (flaring up after symptom-free periods) condition.
However, the following factors may play a role, or there may be an interaction between these factors in the development of Crohn’s disease:
- Immune factors: Abnormal immune response to harmless microorganisms or unknown environmental factors triggers chronic inflammation of the gastrointestinal tract. The body’s own immune response considers the bowel as a foreign body
- Genetic factors: Scientists have identified a few genotypes (characteristic genetic make-up) responsible for the development of Crohn’s Disease in individuals with a family history, and in certain races such as Jews
- Environmental factors: Smoking, NSAIDs, oral contraceptive pills, bacteria, and other unknown factors have been implicated in the development of this condition
- In Crohn’s Disease, the body reacts inappropriately to harmless microorganisms or other unknown factors by sending inflammatory cells (white blood cells) to kill them. In the process, white blood cells also attack the lining of the gastrointestinal tract by producing harmful substances that injure the tract and also set-off chronic inflammation
All the above-mentioned factors ultimately lead to the activation of T-cell (type of white blood cell lymphocyte), which leads to chronic inflammation and destruction through the production of substances such as TNF alpha and interleukin-12
- This chronic process leads to ulcer formation, scarring, perforation (hole), and fistula formation (tunneling between GI tract and other organs including the skin)
- The characteristic features of Crohn’s Disease are the presence of normal bowel in between the affected bowel (skip lesion) and involvement of the entire thickness of the bowel wall (from the innermost lining of the hollow gastrointestinal tract to the outermost layer)
- Scar formation narrows the size of the hollow gastrointestinal tract, which leads to slowing of the passage of food and even cause obstruction, producing symptoms such as abdominal pain, cramps, or diarrhea
- Ulcer formation exposes the blood vessels and causes bleeding into the gastrointestinal tract that manifests as bloody diarrhea
What are the Signs and Symptoms of Crohn’s Disease?
The signs and symptoms vary from one individual to another. The signs and symptoms of Crohn’s Disease include:
- The most common symptom is diarrhea. The diarrhea stool can be mixed with pus and/or blood
- Feeling of illness due to fatigue, decreased appetite, nausea, etc.
- Abdominal cramps /pain may be felt in the region where the bowel is affected. The pain is most common in the right lower abdomen, since the ileum is the most commonly involved site
- Mouth ulcers
- Vomiting, if there is obstruction of the gastrointestinal tract
- Rectal bleeding or bloody diarrhea
- Fever
- Weight loss due to decreased appetite and or decreased absorption of nutrients
- Fistula formation: It is the abnormal tunneling between two bowel loops, between the bowel and vagina, urinary bladder, or skin. Mucus may pass through this abnormal tract to the skin. Also, bowel contents may leak through the vagina or urine
- The abnormal immune response in the body may also affect other organs and produce symptoms such as pain in the eye (uveitis), joint pain, etc.
How is Crohn’s Disease Diagnosed?
The following procedures may be used in the diagnosis of Crohn’s Disease:
- Thorough evaluation of the individual’s medical history and a thorough physical examination including abdomen, pelvis, skin, eyes, joints, etc.
- During history taking, the healthcare provider may want to know the following:
- When the symptoms began and whether they are becoming worse
- List of prescription and over-the-counter medications currently being taken
- About one’s personal and family history of Crohn’s Disease, travel history, similar problems in the family, diet history, etc.
- A gastroenterologist consultation is often necessary, as they are the experts in dealing with bowel disorders
The diagnostic tests undertaken will depend on the particular segment involved by Crohn’s Disease and may include:
- Complete blood count (CBC) may show anemia, increased white blood cell count, etc.
- Other blood tests may be performed to assess overall health (well-being)
- Stool tests are done to rule out bacterial and other parasitic diseases
- Upper GI series (barium meal): Barium, a contrast agent, is given to swallow and it is followed by a series of abdominal X-rays to examine the bowel contour. This test is mostly performed in individuals with symptoms pointing to the small intestine
- Lower GI series (barium meal): Barium is given through enema and it is followed by a series of abdominal X-rays to assess the bowel contour. This test is performed in individuals with symptoms referring to the large intestine
- Colonoscopy and sigmoidoscopy: A lighted tube is inserted through the anus to visualize the bowel directly and take tissue biopsy samples for examination. With colonoscopy, it is possible to visualize the entire large intestine; whereas with sigmoidoscopy, only a partial segment of the large intestine can be visualized
- Upper GI endoscopy is done to visualize the esophagus, stomach, and duodenum
- Imaging procedures, such as CT or MRI scans may be undertaken to visualize the entire abdomen and to check for any complications
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Crohn’s Disease?
The complications of Crohn’s Disease may include:
- Intestinal obstruction: The food and stool does not move in the bowel due to scar tissue formation secondary to chronic inflammation
- Intestinal ulcer formation that may penetrate the bowel wall and cause bleeding or fistula formation
- Bowel perforation (hole through the bowel wall) can lead to life-threatening abdominal infection
- Emotional distress during flare-ups
- Nutrition deficiency of protein, vitamins, minerals, etc., due to chronic inflammation, decrease absorption, decreased appetite, and nausea
- There is a slight risk of developing cancer, when compared to the general population
- Side effects of medications used for Crohn’s Disease can cause weak bones (osteoporosis due to corticosteroids), immune deficiency (due to corticosteroids), etc.
How is Crohn’s Disease Treated?
The treatment options of Crohn’s Disease depend on various factors, such as the age of the patient, severity of the condition, whether the condition is newly-diagnosed, or whether flare-ups are being addressed, the location of Crohn’s Disease in the gastrointestinal tract, and many other factors.
- Having no treatment is an option in individuals with minimal symptoms
- Lifestyle changes, such as exercise, following dietician-approved diet, eating small meals, avoiding certain medications (e.g. oral contraceptive pills) that can trigger a flare-up, etc. can help improve the quality of life
- Hospitalization may be recommended for severe cases
- Medications that are prescribed for the symptoms during flare-ups include
- Codeine for diarrhea
- Intravenous fluids, in individuals who are dehydrated
- Total parenteral nutrition (nutrition through the veins), for malnourished individuals
- Painkillers
- Antibiotics, such as metronidazole, may be given in case of an associated infection
- Oral iron may be given in individuals with anemia
- Nutritional supplements may be given in individuals who are present with nutritional deficiency
- Crohn’s Disease specific medications can be given for flare-ups or to prevent a flare-up from occurring, which include:
- Corticosteroids (oral, intravenous, or enema) are very effective in controlling the inflammation quickly in a flare-up. However, it should not be given for longer durations because of long-term side-effects
- Anti-inflammatory medications, such as mesalazine, may be given in a flare-up or to prevent a flare-up
- Immunomodulators, such as azathioprine and methotrexate, is useful in acute flare-ups and in situations where corticosteroids were not helpful. These medications modulate the abnormal immune response in an affected individual
- Biological therapies, such as adalimumab or infliximab, are very effective in decreasing inflammation. These medications also help control abnormal immune response by directly acting on the harmful immune products. Both immunomodulators and biological therapies can help avoid long-term corticosteroid use
- Surgery is indicated when symptoms are not responding to medications. It is also needed for treating complications such as intestinal obstruction, fistulas, stricture, etc.
The healthcare provider may recommend the best treatment options based upon the individual’s specific health condition and circumstances.
How can Crohn’s Disease be Prevented?
Currently, there are no known methods to prevent the occurrence of Crohn’s Disease. However, once the condition is diagnosed, flare-ups (exacerbation) can be prevented through:
- Understanding the illness and its symptoms
- Avoiding diet or medications that could trigger it
- Consuming adequate and proper nutrition
- Following an active and healthy lifestyle
- Frequently following-up with your healthcare provider
What is the Prognosis of Crohn’s Disease? (Outcomes/Resolutions)
- Crohn’s Disease is an incurable, chronic, and long-standing illness associated with frequent flare-ups and symptom-free periods (remission)
- There is no clear evidence regarding the factors which cause flare-ups and remission
- However, the affected individuals can lead relatively normal lives with prompt treatment of flare-ups and frequent follow-ups with the healthcare provider
Additional and Relevant Useful Information for Crohn’s Disease:
Crohn’s Disease is named after Dr. Burrill Crohn, an American gastroenterologist, who first described the condition.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.