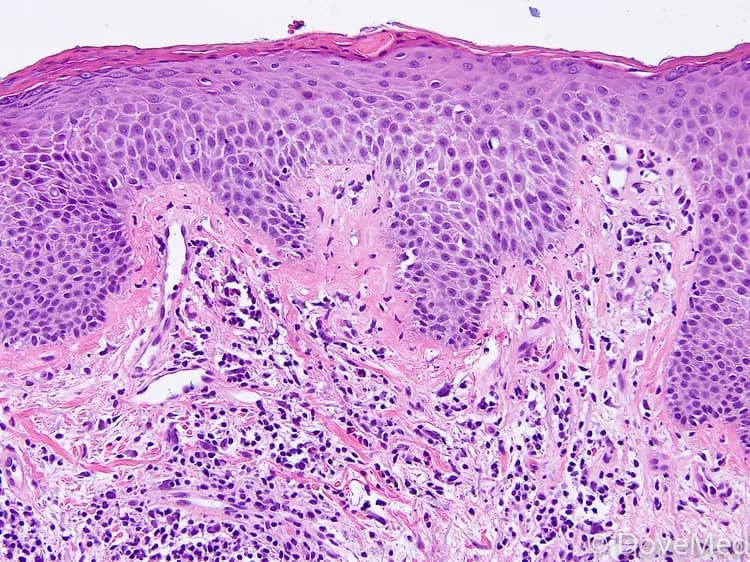
Contact Dermatitis
What are the other Names for this Condition? (Also known as/Synonyms)
- Contact Eczema
- Contact Hypersensitivity of Skin
- Dermatitis Venenata
What is Contact Dermatitis? (Definition/Background Information)
- Contact Dermatitis is a medical disorder characterized by inflammation of the skin that occurs when the skin comes in direct contact with substances that cause irritation or allergy to the skin
- Some common allergens and irritants that can trigger the condition include the metal nickel, trees and plants (such as oak and poison ivy), cashew nut shell, fragrances, strong soaps and detergents, and many other such substances
- Contact Dermatitis affects women more often than men. Any part of the body may be affected, but the most frequently affected region is the hand
- Some of the common signs and symptoms include red rashes and bumps on the skin; dry, cracked, red patches that resemble skin burns; and the presence of blisters that drain fluid. A superimposed bacterial infection is a common complication of Contact Dermatitis
- The treatment of Contact Dermatitis involves a complete avoidance of the causative agent and the use of medications that include corticosteroids and antihistamines. The condition typically resolves within 2 to 3 weeks, usually without any complications
- Identification of substances that are skin allergens and irritants is the first and foremost preventive measure
There are various types of Contact Dermatitis and these include:
- Irritant Contact Dermatitis
- Allergic Contact Dermatitis
- Photo-Allergic Contact Dermatitis
- Phototoxic Contact Dermatitis
Who gets Contact Dermatitis? (Age and Sex Distribution)
- Contact Dermatitis can affect any individual, at any age
- Generally, women are more affected by this condition than men
- No racial, ethnic, or geographical predominance is observed
What are the Risk Factors for Contact Dermatitis? (Predisposing Factors)
Individuals in the following profession are at an increased risk of Contact Dermatitis:
- Cooks and chefs
- Welders
- Glass blowers
- Farmers
- Factory workers
- Hair stylist
- Constructions workers
- Healthcare workers
- Lifeguards
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Contact Dermatitis? (Etiology)
Contact Dermatitis is of several types and each of them may be caused by different factors.
Irritant Contact Dermatitis:
- It is the most common type of Contact Dermatitis
- The condition occurs when the skin gets damaged due to exposure to substances that irritate the outer protective layer of the skin
- Some of the commonly used chemicals that are irritants include:
- Harsh soaps
- Chemical solvents
- Cosmetics
- Skin products
- Deodorants
- Acids and bases (lye)
Allergic Contact Dermatitis:
- It occurs when an allergic substance activates an immune reaction in the skin
- Frequently used substances that are allergens may include:
- Natural rubber
- Metals such as nickel
- Costume jewelry
- Perfumes and cosmetics
- Hair dyes
- Plants such as poison ivy
Photo-Allergic Contact Dermatitis:
- This occurs when a substance has been applied on skin and is exposed to sunlight
- The reaction to exposure may be observed in a few days (may be after 1-2 days)
- Some of the commonly used substances that can trigger this condition include:
- Sunscreen lotions
- Ointments containing non-steroidal and anti-inflammatory drugs
- Certain oral drugs, such as hydrochlorothiazide, which is used as a diuretic in the treatment of high blood pressure
- Some insecticide sprays
Phototoxic Contact Dermatitis:
- In this condition, the sunlight activates certain substances (photo-sensitive allergens or irritants) on exposure
- Such substances include perfumes containing psoralen, coal tar, and certain drugs
- Following exposure, reaction (such as skin color change) is observed immediately (within a few minutes to hours)
Some common allergens and irritants that can trigger Contact Dermatitis may include:
- Nickel and other metals
- Plants and trees such as poison ivy, oak, and sumac that contains a strong allergic oil called urushiol
- Cashew nut shells; these too contain allergic substances, such as urushiol, in them. Cashews are seldom shipped before burning off the outer covering the allergen
- Antibiotics, antihistamines, and antiseptics, which are applied on the skin in the form of creams, ointments, and lotions
- Certain fragrances
- Strong detergents and harsh soaps
- Skin cleansers
What are the Signs and Symptoms of Contact Dermatitis?
The common signs and symptoms observed with Contact Dermatitis include:
- Red rashes and bumps on the skin
- Dry and cracked red patches that resemble burns on the skin
- Blisters on the skin that drain or ooze fluid
- The skin rashes are generally confined to a particular area
- Pain and tenderness in the affected area
How is Contact Dermatitis Diagnosed?
A diagnosis of Contact Dermatitis would include:
- A complete evaluation of one’s medical history to learn about the causative agent, the source of the condition
- A thorough physical examination of the patient to check for signs and symptoms with respect to Contact Dermatitis. In these conditions, the location of the rash can be one of the most important clues to the correct diagnosis. For example, the rash may be seen only on skin exposed to sunlight
- Patch test:
- In this test, small quantities of substances (believed to be allergens) are applied on the skin in small patches
- The application is left for a couple of days, after which the responses are observed
- If the individual develops bumps or rashes in the patchy area where the substances/allergens were applied, it may be confirmed that the patient is allergic to that particular substance
- Photopatch test:
- In this test, the suspected substances are applied to two different areas of the skin
- One site is exposed to artificial light, the other is not. Both areas are checked for reactions
Skin biopsy: A skin biopsy is performed and sent to the laboratory for pathological examination. The pathologist examines the biopsy under a microscope for a definitive diagnosis
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Contact Dermatitis?
Contact Dermatitis could lead to the following complications namely:
- Neuro-dermatitis: It involves chronic itching and scaling of the skin that causes the skin to become thick, discolored, and leathery
- Bacterial and fungal infection: Continuous itching and scaling of the skin will create skin moistness, providing a suitable environment for bacteria and fungi to grow and thrive
How is Contact Dermatitis Treated?
Treatment strategies that may be adopted in the management of Contact Dermatitis include:
- Avoiding exposure or contact with substances that are (known) irritants and allergens
- Application of anti-itch, over-the-counter creams that contain hydrocortisone can provide relief from pain and itching sensation
- Oral medications: The physician may prescribe oral corticosteroids to reduce inflammation or antihistamines to provide relief from severe itching sensation
A few self-care tips and home remedies for Contact Dermatitis may include:
- Scratching the affected areas must be completely avoided
- A comfortable, cool bath may help soothe the skin
- Wearing smooth cotton clothes
- Use of mild perfumes, soaps, and detergents
How can Contact Dermatitis be Prevented?
The following measures may be adopted to prevent or reduce the risk of acquiring Contact Dermatitis:
- Identification of substances that are skin allergens and irritants is the first and foremost preventive step. Avoiding substances identified as allergens and irritants will help protect from Contact Dermatitis
- In case of contact with the allergic substance, wash the affected area immediately with water
- Wearing protective gloves while doing household work will protect the skin from coming into contact with allergic substances and irritants
- Always choose soaps with mild detergents both for bathing and washing clothes
- A protective cream may be applied over the skin for protection. The use of a moisturizer can help protect the topmost layer of the skin
- To help protect from metal allergies, measures such as covering the metal fasteners on the jeans that come into contact with skin may help
What is the Prognosis of Contact Dermatitis? (Outcomes/Resolutions)
- Contact Dermatitis usually resolves within 2-3 weeks, generally without any complications
- If the condition is recurrent, it may be because the exact cause is not yet identified
- If Contact Dermatitis is due to an occupational exposure, then the occupation or job-related tasks or habits may have to be changed/modified
Additional and Relevant Useful Information for Contact Dermatitis:
The following DoveMed website link is a useful resource for additional information:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.