What are the other Names for this Condition? (Also known as/Synonyms)
- Breast Cancer Tumor
- Cancer of Breast
- Carcinoma of Breast
What is Breast Cancer? (Definition/Background Information)
- Breast Cancer is the most common type of cancer diagnosed in women and is believed to be the second-most leading cause of death in women
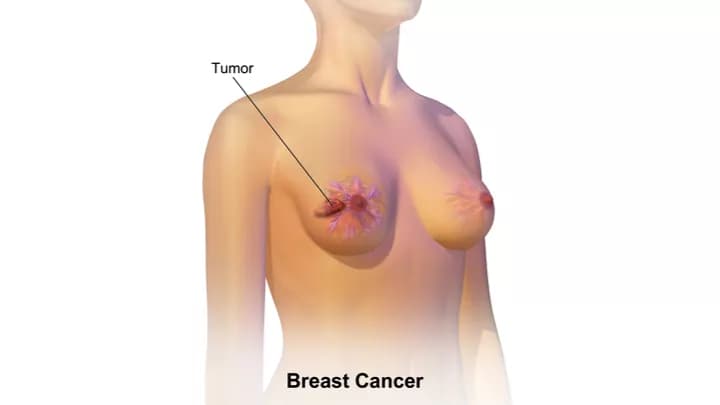
- It is a type of cancer in which certain cells in the breast become abnormal, grow uncontrollably, and form a malignant mass (tumor)
- Breast Cancer cells can also break away from the initial tumor, invade nearby tissues, and spread or metastasize to other regions of the body
There are various types of Breast Cancer:
Ductal carcinoma: It is a type of Breast Cancer that begins in the cells of the milk ducts. Milk ducts are tubes in the breasts that carry milk from the site of production to the nipples.
- Ductal Carcinoma in Situ (DCIS): The cancerous cells are found exclusively in the lining of the milk ducts, and have not spread to other breast tissues (non-invasive Breast Cancer)
- Invasive Ductal Carcinoma: The cancerous cells that originated in the milk ducts, have spread to other tissues in the breast, and are able to metastasize to other parts of the body (invasive Breast Cancer)
Lobular carcinoma: Breast Cancer that begins in the milk lobules (part of the breast which produces milk)
- Lobular Carcinoma in Situ: The cancerous cells are found exclusively in the lobules of the breast, and have not spread to other tissues within the breast
- Invasive Lobular Carcinoma: The cancerous cells have spread from the milk lobules into surrounding tissues within the breast. They are also able to metastasize to other parts of the body
According to the World Health Organization (WHO) Classification of Tumors (5th Edition), Breast Tumors include the following types:
Epithelial tumors of the breast:
- Benign epithelial proliferations and precursors
- Adenosis and benign sclerosing lesions
- Adenomas
- Epithelial-myoepithelial tumors
- Papillary neoplasms
- Non-invasive lobular neoplasia
- Ductal carcinoma in situ
- Invasive breast carcinoma
- Rare and salivary gland-type tumors
- Neuroendocrine neoplasms
Fibroepithelial tumors and hamartomas of the breast:
- Fibroepithelial tumors and hamartomas of the breast
- Fibro-epithelial tumors
Tumors of the nipple:
- Tumors of the nipple
- Epithelial tumors
Mesenchymal tumors of the breast:
- Mesenchymal tumors of the breast
- Vascular tumors
- Fibroblastic and myofibroblastic tumors
- Peripheral nerve sheath tumors
- Smooth muscle tumors
- Adipocytic tumors
- Other mesenchymal tumors and tumor-like conditions
Hematolymphoid tumors of the breast:
- Hematolymphoid tumors of the breast
- Lymphoma
- Extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma)
- Follicular lymphoma
- Diffuse large B-cell lymphoma
- Burkitt lymphoma
- Breast implant-associated anaplastic large cell lymphoma
Tumors of the male breast:
- Tumors of the male breast
- Epithelial tumors
- Gynaecomastia
- Carcinoma in situ
- Invasive carcinoma
Metastases to the breast:
- Metastases to the breast
Genetic tumor syndromes of the breast:
- Genetic tumor syndromes of the breast
- Syndromes
Who gets Breast Cancer? (Age and Sex Distribution)
- Although both women and men are capable of developing Breast Cancer, the condition is much more common in women
- Older women (over the age of 55 years) have a greater risk than younger women
- All racial and ethnic groups are affected by Breast Cancer
What are the Risk Factors for Breast Cancer? (Predisposing Factors)
The risk factors for Breast Cancer may include:
- Being a woman: Women have a much greater chance of developing Breast Cancer than men
- Age: The risk increases for women over the age of 55 years
- Personal history: Having cancer in one breast, puts a woman at risk for having cancer in the other breast as well
- Family history: Women with a mother, sister, or daughter diagnosed with Breast Cancer are at a higher risk for developing the condition
- Inherited gene mutations: Mutations in certain genes (BRCA1 or BRCA2) can lead to a much higher risk
- Radiation therapy: Receiving radiation therapy to the chest or breast area can also increase the risk for Breast Cancer. It is noted that the risk for developing Breast Cancer later in life is the greatest for radiation therapy administered during puberty
- Obesity: Being overweight or obese elevates the risk after menopause
- Alcohol use: Consuming alcohol more than one drink per day; the more the alcohol consumed, the greater is the risk
- Menstrual cycle: Women who got their period before the age of 12 years, and those who reached menopause after age 55 have a higher risk
- Postmenopausal hormone therapy: Women taking hormone replacement therapy medications containing both estrogen and progesterone for menopause have a higher risk of developing Breast Cancer
- Reproductive history: Having your first child after the age of 35, or never having children
- Physical inactivity: A lack of physical exercise (leading a sedentary life), can increase your risk
- Breastfeeding: Not breastfeeding one's child can increase the risk for developing the condition
Factors that do not affect a woman’s risk for Breast Cancer include the use of antiperspirants, deodorants, having breast implants, or wearing underwired bras.
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Breast Cancer? (Etiology)
The exact cause of Breast Cancer formation is currently not clearly known.
- As with other cancer types, Breast Cancer begins when normal, healthy cells transform into abnormal ones, which then begin growing and multiplying uncontrollably
- These cells can lead to the formation of masses or tumors that may even spread (metastasize) outside the breast (such as to the lymph nodes)
- Having certain risk factors may increase a woman’s chances of developing Breast Cancer; however, it does not necessarily mean that an individual will develop the condition
- On the contrary, some women with no known risk factors develop Breast Cancer for unknown reasons
What are the Signs and Symptoms of Breast Cancer?
The signs and symptoms of Breast Cancer may include:
- A lump in the breast, or underarm area
- Thickening or swelling of part of the breast; change in the size or shape of the breast
- Inversion of the nipple (pulling-in of nipple into the breast)
- Bloody discharge from the nipple
- Changes to the skin covering the breast or nipple area, including dimpling, irritation, redness, scaling, peeling, or puckering
- Pain in the breast; this is an uncommon symptom
How is Breast Cancer Diagnosed?
Breast Cancer is diagnosed as follows:
- Breast exam: The physician will check for any lumps or unusual signs in the breasts
- Mammogram: A mammogram uses X-rays to provide images of the breast. Screening mammograms are commonly used to detect possible signs of Breast Cancer in women with no apparent symptoms. Diagnostic mammograms give more detailed images of areas in the breast after abnormalities have been detected using a screening mammogram
- Breast ultrasound: Using high-frequency sound waves to produce images of the breast, an ultrasound can identify whether a lump is a fluid-filled cyst (non-cancerous) or a solid mass (which may be cancerous or benign)
- Magnetic resonance imaging (MRI) scan: An MRI scan involves the use of radio waves and magnets to provide a series of detailed images of the breast area
- Breast biopsy: A biopsy is a procedure involving the removal of a sample of breast tissue for further examination by microscopy.
Biopsies are the only methods used to determine whether an abnormality is cancerous or not. These are performed by inserting a needle into a breast mass and removing cells or tissues for further examination. There are different types of biopsies:
- Fine needle aspiration biopsy: In this method, a very thin needle is used to remove a small amount of tissue
- Core needle biopsy: A wider needle is used to withdraw a small cylinder of tissue from an abnormal area of the breast
- Surgical biopsy: A surgical procedure used less often than needle biopsies, it is used to remove a part of or all of the breast lump for analysis
The following additional tests may also be required:
- Blood tests
- Computerized tomography (CT) scan
- Positron emission tomography (PET) scan
- Bone scan
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Breast Cancer?
- The possible complications include various side effects from Breast Cancer treatment
- Spread of cancer to other regions of the body
- Lymphedema, or the swelling of an arm, may occur after surgery or radiation therapy, due to restriction of flow of lymph fluid; therefore causing the build-up of lymph. A lymphedema can form anywhere from weeks to years after a Breast Cancer treatment that involves, removes, or targets radiation therapy to the axillary lymph nodes
How is Breast Cancer Treated?
Treatment options available for individuals with Breast Cancer are dependent upon the following:
- Type of cancer
- The staging of the cancer
- Whether the cancer cells are sensitive to certain particular hormones, and
- Personal preferences
Surgery: Surgery is the most common form of Breast Cancer treatment involving the removal of the tumor. Various types of surgery, to remove the cancer include:
- Lumpectomy: Breast-sparing surgery (least invasive breast cancer surgery) in which the tumor, as well as a small portion of surrounding tissue, is removed
- Mastectomy: Surgery to remove all of the breast tissue; it may be simple (removal of the breast, nipple, areola, sentinel lymph nodes) or radical mastectomy (removal of the breast, nipple, areola, all axillary lymph nodes, and underlying muscle of the chest wall)
- Sentinel node biopsy: Procedure done to examine the “sentinel lymph node,” or lymph node(s) closest to the tumor, as this is the most likely location, where cancer cells may have spread to. This lymph node is removed and tested for cancerous cells
- Axillary node dissection: This procedure is performed to remove some axillary lymph nodes in the underarm area, to allow dissection and examination. This helps in establishing whether the cancer has spread to more than one lymph node
Chemotherapy:
- Using the help of drugs, chemotherapy either kills the cancer cells or shrinks the tumor
- Chemotherapy may be recommended after surgery, for a tumor with a high probability of returning or metastasizing (spreading) in what is termed as adjuvant chemotherapy. The procedure kills any remaining cancer cells, following a surgery for the cancer
- Chemotherapy may also be suggested before surgery, for women with large cancers to reduce the size of the tumor. This allows for easier removal during surgery and is termed neoadjuvant chemotherapy
- The use of chemotherapy is also an option for women with advanced breast cancer, which that has already spread outside the breast
- Side effects of the therapy may include nausea, vomiting, hair loss, decreased appetite, mouth sores, fatigue, low blood cell counts, and a higher chance of developing infections
Radiation therapy:
- Using high-energy beams, including x-rays, radiation therapy aims to kill cancerous cells
- Radiation therapy can be done externally (external beam radiation) using a large machine, to target rays at the cancerous area
- It may also be administered internally (internal beam radiation) using a radioactive substance that collects at the site, where the cancer originated
- Commonly recommended after a lumpectomy, for women with Breast Cancer still in its early stages
- Side effects include a sunburn-like rash, where radiation was targeted; red or dry skin; heaviness of the breasts; or general fatigue
Hormone therapy:
- Hormone therapy is typically recommended for estrogen receptor positive (ER positive) or progesterone receptor positive (PR positive) Breast Cancers. The cells of these cancers are receptive to hormones, which help stimulate cancer growth
- Hormone therapy drugs act as inhibitors or blockers, preventing cancer cells from receiving the hormones needed to promote their development
- Tamoxifen, the most common hormone therapy drug, works by blocking estrogen from binding to the estrogen receptors on cancer cells. It thus prevents cancer cells, from receiving signals to grow and multiply. Side effects may include hot flashes, night sweats, or vaginal discharge. More serious risks include blood clots, stroke, or uterine cancer
- Aromatase inhibitors stop the production of estrogen in postmenopausal women. Thus, lower levels of estrogen are available to promote cancer cell growth. Examples of these inhibitors include anastrozole, letrozole, and exemestane. Possible side effects may include joint or muscle pain and a higher risk for osteoporosis
- In premenopausal women, surgery to remove the ovaries is an option to prevent estrogen production as the ovaries are the main source of estrogen before menopause
Targeted therapy:
- Targeted therapy drugs attack cancer cells in a specific manner
- Trastuzumab (Herceptin) is a drug that targets human growth factor receptor 2 (HER2), a protein that is made by some Breast Cancer cells to stimulate their growth, blocking HER2 causes cancer cells to die off. Side effects may include heart damage, headaches, nausea, vomiting, skin rashes, and breathing problems
- Lapatinib (Tykerb) is a targeted therapy drug that targets HER2 proteins, to help slow the growth of cancer cells. Lapatinib is usually recommended after other treatment options have been attempted, but have been found ineffective in slowing the cancer progress. Side effects may include nausea, vomiting, diarrhea, mouth sores, fatigue, pain in the hands and feet, and skin rashes
- Bevacizumab (Avastin) works by preventing Breast Cancer tumors from creating new blood vessels that could nourish the tumor, cutting off the supply of nutrients to cancer cells. Potential side effects may include high blood pressure, fatigue, headaches, heart or kidney damage, slow healing of wounds, mouth sores, and blood clots
How can Breast Cancer be Prevented?
The following measures may help in reducing one's risk for Breast Cancer:
General lifestyle changes:
- Maintain a healthy weight and exercise regularly
- Implement and follow a well-balanced diet
- Drink alcohol in moderation; limit to one or (maximum) two drinks a day
- Limit combination hormone therapy used to treat symptoms of menopause. Consult your physician about the benefits and risks of hormone therapy
- Cancer screenings can help detect any Breast Cancer in its early stages
- Learn to do ‘breast self-exams’ in order to help identify any unusual lumps or signs in your breasts
In women with a high risk for developing Breast Cancer, other options may be suggested by their physicians. These may include:
- Preventative medications: The medications tamoxifen and raloxifene (Evista) are estrogen-blocking drugs that can help prevent the onset of Breast Cancer in women at high risk. Both drugs have potential side effects including being at a higher risk for blood clots
- Preventative mastectomy: Prophylactic mastectomy, a procedure to surgically remove healthy breasts, is another possible preventative option for women at a high risk for Breast Cancer
What is the Prognosis of Breast Cancer? (Outcomes/Resolutions)
Currently, new and improved treatments are helping to increase the longevity of individuals with Breast Cancer. Nevertheless, the cancer can return or spread to other areas of the body, even with proper treatment.
Various factors are used to determine each individual’s prognosis. These include:
- Staging of the cancer
- Location, size, and shape of the tumor
- Type of breast cancer
- Hormone-receptor status of Breast Cancer
- Presence of tumor indicators such as HER2 proteins (growth-promoting proteins)
- Cell growth rate
- Likelihood of cancer returning
- Age
- Menopausal status
Breast Cancer stages range from 0 to IV. 0 may indicate a small and non-invasive cancer, while IV indicates that the cancer has spread to other areas of the body. Briefly, as per National Cancer Institute (at the National Institutes of Health), Breast Cancer is staged as follows:
- Stage 0 (carcinoma in situ): The abnormal cancer cells are confined to their site of origin (the breast duct linings, lobules, or nipples)
- Stage I: The tumor is 2 centimeters in diameter or less, and has not spread outside the breast
- Stage II: The tumor may be up to 5 centimeters in diameter and may have spread to lymph nodes. Another criteria is that the tumor may be larger than 5 centimeters in diameter, but has not spread to surrounding lymph nodes
- Stage III: The tumor may be more than 5 centimeters in diameter and may have spread to several axillary lymph nodes, or to the lymph nodes near the breastbone. The cancer may also have spread to the breast skin/chest wall, causing ulcer-like sores, or a swelling
- Stage IV: The tumor has spread outside the breast and to other organs, such as the bones, liver, lungs, or brain, regardless of its size
If Breast Cancer is diagnosed, staging helps determine whether it has spread and which treatment options are best for the patient.
Additional and Relevant Useful Information for Breast Cancer:
- It is estimated that 1 in 8 women shall be diagnosed with Breast Cancer, during their lifetime. This means that approximately 220,000 women (in the U.S.) will be diagnosed with the disease, and the number of fatalities may be around 40,000
- Women in European and American countries have a higher incidence of the cancer than women in African and Asian countries
- The risk for a man with Breast Cancer formation is about 1 in 1,000
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.