What are the other Names for this Condition? (Also known as/Synonyms)
- Balantidium Coli Infection
- Ciliary Dysentery
- Human Balantidiasis
What is Balantidiasis? (Definition/Background Information)
- Balantidiasis is a treatable disease caused by ingesting the intestinal parasite, Balantidium coli, in food or water that has been contaminated by human or animal feces
- The infection is prevalent in regions with tropical climate and poor sanitation. No racial or gender bias is reported in its occurrence
- Poor hygiene in those living in areas of high incidence of Balantidiasis is a major risk factor for contracting the infection
- Individuals with this infection typically do not display any signs and symptoms, if it is mild. However, severe cases can result in symptoms including diarrhea, abdominal pain, and even perforation of the colon
- Balantidiasis can be treated using several antibiotics. With appropriate treatment, the prognosis is generally good
- Prevention of Balantidiasis can be achieved with improved hygienic practices, water sanitation, and proper disposal of fecal matter
Who gets Balantidiasis? (Age and Sex Distribution)
- Individuals of all ages, races and ethnic groups, as well as both genders, are susceptible to Balantidiasis
- The infection has the highest prevalence in regions with tropical weather and poor hygienic practices (mostly in developing countries such as Brazil, New Guinea, and southern Iran)
What are the Risk Factors for Balantidiasis? (Predisposing Factors)
The risk factors for Balantidiasis include the following:
- Poor hygienic practices
- Living in tropical regions with poor sanitation, especially in countries and regions such as Bolivia, Brazil, New Guinea, southern Iran, and Philippines
- Living in close contact with pigs: This infection occurs frequently in areas where pigs are raised (through their feces), as pigs are frequently infected by Balantidium coli
- Failing to wash hands with clean water and soap after working with pigs
- Malnutrition
- Individuals with compromised immunity resulting from HIV/AIDS infection, being on immunosuppressant medication following organ transplantation, and chemotherapy or radiation for treatment of cancer
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one’s chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Balantidiasis? (Etiology)
The cause of Balantidiasis is ingesting food or water that has been contaminated with fecal matter from humans or animals. The fecal matter can contaminate food or water with the protozoan Balantidium coli.
Individuals can become infected following:
- Eating food that has been contaminated with stool from infected humans or animals
- Drinking contaminated water
- Washing food with contaminated water
- Maintaining poor hygiene
- Failing to wash hands properly after direct contact with pig feces
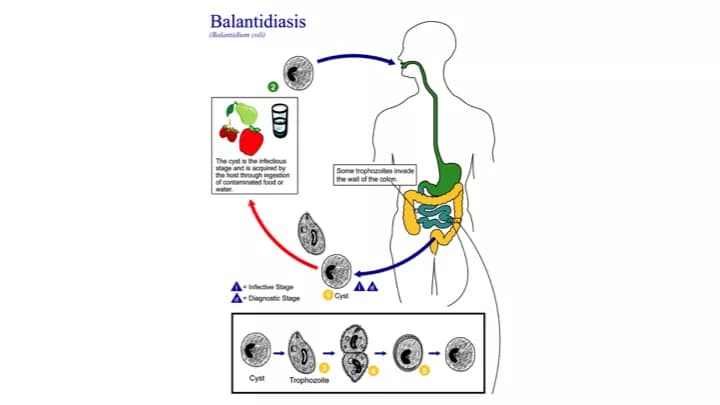
Once ingested, Balantidium coli invades the large intestine (colon), producing infective cysts that are then expelled in the feces. These cysts can then infect other individuals who come into contact with the contaminated feces.
What are the Signs and Symptoms of Balantidiasis?
The signs and symptoms of Balantidiasis may vary between infected individuals, and may be severe in individuals with compromised immunity, or those who are severely malnourished. Most individuals with Balantidiasis often display no symptoms. However, they are still capable of transmitting the infection.
If severe infection occurs, the following signs and symptoms may be observed:
- Chronic diarrhea
- Blood and mucus in the stool
- Abdominal pain
- Fever
- Weight loss
- Nausea and vomiting
- Dehydration
- Inflammation, ulceration, and possibly even perforation of the colon, if the condition is left untreated
- Impaired lung function ensuing from perforation, in rare cases
How is Balantidiasis Diagnosed?
The diagnosis of Balantidiasis may be difficult, as other conditions affecting the bowel may present with similar symptoms. The diagnosis of the infection is made by:
- A thorough physical examination and assessment of symptoms
- An evaluation of the affected individual’s medical and travel history
- Microscopic examination of stool samples to check specifically for Balantidium coli
- Surgical scraping (biopsy) of ulcers to examine the tissue for Balantidium coli
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Balantidiasis?
The potential complications of Balantidiasis include:
- Weight loss and dehydration as a result of symptoms of Balantidiasis (such as diarrhea, vomiting and dehydration)
- Hemorrhage that can lead to shock, resulting from persistent ulcers or perforations. This complication can be fatal
How is Balantidiasis Treated?
Balantidiasis can be treated with various antibiotics, such as tetracycline, metronidazole, and iodoquinol.
- The medications are typically administered orally, and they can effectively treat the infection
- Additionally, symptomatic treatment is provided
How can Balantidiasis be Prevented?
Balantidiasis can be prevented by adhering to the following practices:
- Washing hands with soap and clean water after using the bathroom, after changing diapers, or before handling food (especially when traveling to developing countries)
- Washing fresh produce (vegetables and fruits) with clean water before consumption
- Improving water sanitation
- Establishing suitable barriers between pigs and humans
- Properly disposing of fecal matter: Balantidiasis can only be transmitted through fecal matter; hence, it is important that stool from an infected individual be properly disposed, to prevent further spread of the infection
- Maintaining good hygienic practices after working with pigs
What is the Prognosis of Balantidiasis? (Outcomes/Resolutions)
The prognosis of Balantidiasis is typically good following treatment with approved antibiotics.
- While symptoms typically worsen without treatment, resulting in severe complications, the infection is known to clear spontaneously in many affected individuals as well
- Those with poor overall health (malnutrition, compromised immunity, alcoholism, or with other intestinal infections) are more likely to have severe symptoms and complications
Additional and Relevant Useful Information for Balantidiasis:
Washing the hands with soap and water is extremely important to avoid sickness and the spread of germs. Additional information about how to properly wash your hands to prevent infection is provided below:
- Wet your hands with clean, running water and apply soap
- Rub your hands together, lathering the backs of your hands, between your fingers, and under your nails
- Scrub your hands for a minimum of 20 seconds
- Rinse your hands under clean, running water, and dry your hands with a clean towel
- If soap and water are not available, alcohol-based sanitizers can be used to reduce the number of germs on your hands
Balantidiasis infection is generally uncommon in the United States.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.