What are the other Names for this Condition? (Also known as/Synonyms)
- Anaerobic Vaginosis (AV)
- Nonspecific Vaginitis
- Vaginal Bacteriosis
What is Bacterial Vaginosis? (Definition/Background Information)
- Bacterial Vaginosis (BV) is a frequently-occurring and usually mild bacterial infection, particularly in women, who are in their active reproductive or childbearing phase
- Although Bacterial Vaginosis is harmless and self-limiting in most cases, it has the potential to increase an individual’s susceptibility to other sex-related disorders and cause medical complications
- Foul-smelling, watery, milk white vaginal discharge, with itching and burning sensation around the vaginal region, are a few of the symptoms. These are caused, when there is a bacterial imbalance within the vagina
- Many factors are said to contribute to this condition, such as having multiple sex partners, having unprotected sex, douching, etc.
- Antibiotic treatment is the therapy of choice, which can result in a complete cure
Who gets Bacterial Vaginosis? (Age and Sex Distribution)
- Women in the childbearing age group and pregnant women have the highest risk for this bacterial infection
- As per a CDC (US, Centers for Disease Control and Prevention) study, over 80% of women with Bacterial Vaginosis are asymptomatic
- African-American and Hispanic American women are more vulnerable than Caucasian women (especially the US)
What are the Risk Factors for Bacterial Vaginosis? (Predisposing Factors)
All factors that are responsible for upsetting the natural balance of bacteria (that exist between the good and bad bacteria) in the vaginal tract are potential risk factors for Bacterial Vaginosis. These include:
- Having a new sex, same sex partner(s), and/or multiple sex partners. These may include individuals with sexually-transmitted diseases
- Vaginal douching
- Use of intrauterine devices for contraception
- Reduced incidence of sexual activity (intercourse), or a complete absence of sex life
- Post-menopausal women
- Recent antibiotic use, for an unrelated condition
- Other factors that increase the risk include: Cigarette smoking, anemia, and the use of thongs
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Bacterial Vaginosis? (Etiology)
- There exists a normal balance between the good bacteria (like lactobacilli) and the few harmful ones (the anaerobes), which helps maintain a certain pH value, within the reproductive tract
- When good bacteria level gets reduced and the bad bacteria grow and proliferate, under certain conditions, it leads to Bacterial Vaginosis. Hence, it is also called Anaerobic Vaginosis
- Any factor that causes an imbalance between the two bacteria kinds creates conditions for BV. This imbalance is responsible for disturbing the natural pH balance in the vagina
What are the Signs and Symptoms of Bacterial Vaginosis?
Only a few women experience signs and symptoms of Bacterial Vaginosis, while a majority of them do not. In women, who experience signs and symptoms, these include:
- Smelly (fish-odor), off-white or grayish-white vaginal discharge, which may be watery thin. These signs increase after sexual intercourse
- Difficulty while having an intercourse, due to a lack of natural lubrication, causing pain, irritation/discomfort, slight bleeding from the vagina
- Occasionally burning sensation on urination, feeling of itchiness may be observed
- There may be an infection around the vaginal or urogenital area
How is Bacterial Vaginosis Diagnosed?
Given the fact that many of the clinical indications of Bacterial Vaginosis are characteristics of other infections or medical issues, the patient medical history is considered with a differential diagnosis to eliminate these factors. Diagnostic tests that are performed for Bacterial Vaginosis include:
- A physical examination of the vagina, vaginal membrane lining, cervix
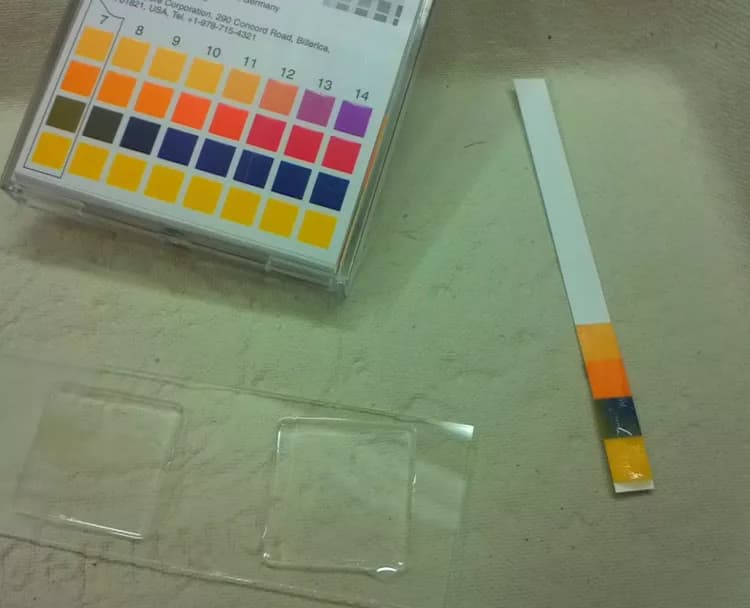
- pH value test of the vagina, by placing a strip of litmus paper
- Examination of vaginal discharge or fluids (wet prep test), to test for other infection types
- Whiff test, to test odor of the vaginal discharge
- Culture of vaginal discharge
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Bacterial Vaginosis?
Due to a lack of treatment of the condition, or due to Bacterial Vaginosis affecting pregnant women, there could be certain serious complications. These include:
- Higher chances of contracting (or the spread of) sexually-transmitted diseases, such as gonorrhea, herpes simplex, and HIV
- Increased susceptibility to other (yeast and bacteria) infections. Increased incidence of pelvic inflammatory disease, endometritis, or cervicitis, occurring in the vagina, uterus, or other adjoining organs, due to changed pH levels, may be seen
- Pelvic inflammatory disease due to Bacterial Vaginosis, can cause infertility issues or damage the fallopian tube. This damage to fallopian tube can lead to life-threatening complications, if the fertilized egg grows outside the uterus (termed as ectopic pregnancy)
- Pregnant women may deliver preterm, low weight babies
- Women with the bacterial condition have a higher risk of post-surgical infection, after any gynecological surgery is performed
- Recurrent BV infection: Many women might experience recurrent symptoms
- Side effects, due to some of the prescribed drugs can be bothersome
How is Bacterial Vaginosis Treated?
There are many causal factors for Bacterial Vaginosis. Hence, it is advisable to consult your physician and get an evaluation of the symptoms presented, before attempting any treatment methods, including any self-care measures. The physician-recommended treatment could include:
- Antibiotics (oral pills) may be administered. The dosage depends on the severity of Bacterial Vaginosis infection, and whether the individual is pregnant or not
- Application of vaginal creams and gels (such as clindamycin), to bring relief from the symptoms and to provide a measure of comfort
- Pregnant women and women, who are scheduled to have any surgical procedures performed on their vagina or other reproductive organs, should be treated for BV, in order to prevent any future complications from occurring
- There are many home remedies and alternative medicines available for Bacterial Vaginosis. However, it is best to consult one’s healthcare provider, before planning to employ such measures
- Male partners are not required to be treated, unless they have other sex-related diseases
How can Bacterial Vaginosis be Prevented?
Medical researchers are still trying to understand Bacterial Vaginosis, and how it is exactly caused. It may not be preventable, but some of the risk factors may be avoided or controlled: These include:
- Avoid multiple sex partners, practice safe sex
- After bowel movement, clean or wipe from front to back and avoid spread of bacteria from the rectum to vagina
- Maintain the outside part of the vagina, clean and dry
- Douching upsets the pH value inside the vaginal tract, and this is not advisable. It is always recommended to preserve the pH value and normal balance within the vagina
- Complete the course of medicines prescribed, even if the signs and symptoms have lessened, or are absent
- Hygiene, perfumed sprays, soaps or tampons should be avoided, unless they are recommended by a healthcare provider
- Avoid tightfitting dress that trap moisture between the legs
- Recognizing the specific medical illness and getting it correctly diagnosed, following treatment methods and maintaining proper self-care, are beneficial to early recovery
What is the Prognosis of Bacterial Vaginosis? (Outcomes/Resolutions)
- Bacterial Vaginosis can be treated completely. A proper management of the condition and completion of the full course of prescribed medication, leads to full recovery from the symptoms. Hence, in a majority of the women, the prognosis of Bacterial Vaginosis is excellent
- A large proportion of the women, who are affected by BV do not require any treatment, if no signs and symptoms are present. However, it is recommended that sexually-active women undergo periodic tests, to assess their sexual health, especially if they fall in the high-risk group
- Pregnant women and those in the high-risk group should seek suitable and prompt treatment, to avoid any serious complications
Additional and Relevant Useful Information for Bacterial Vaginosis:
Bacterial Vaginosis is a common medical issue; but, it is not caused by toilet seats, community swimming pools, sharing items (clothes, bed), etc.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.