Specific Molecular Events That Could Explain Allergic Reactions To Air Pollution
Scientists at the Immunology Frontier Research Center (IFReC) at Osaka University, Japan have pinpointed a specific molecular events that could explain allergic reactions to air pollution. These findings provide a new therapeutic candidate to treat asthma and related respiratory diseases.
Photos of cities darkened by pollution are becoming evermore common. These same cities are seeing a rise in cases of asthma and other respiratory ailments, marking a relationship between pollution and health costs. Nanoscopic particulates polluting the air enter the lungs to cause the allergic reactions. Which immune-related events in the lung lead to this response, however, are unclear.
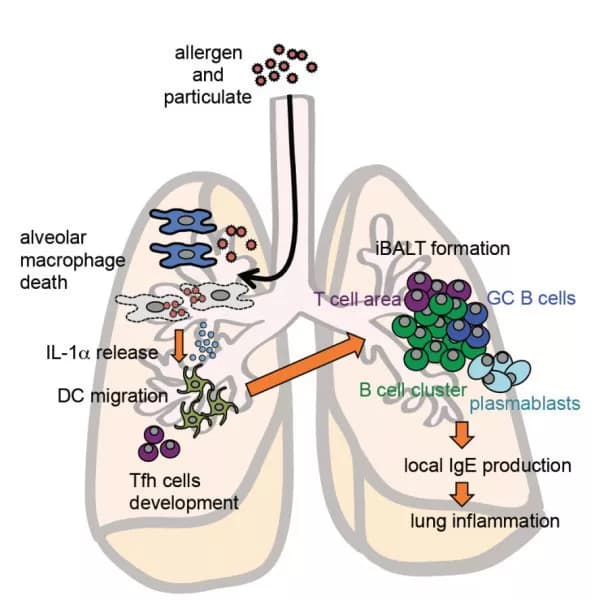
"We found that particulates kill macrophages, which then go on to release interleukin-1a (IL-1α)," explains Etsushi Kuroda, who first-authored a new study in Immunity that indicates IL-1α triggers a series of events that causes respiratory illnesses. The release of IL-1α in mice primed the lungs for inflammation when the mice were later exposed to an allergen. Kuroda added, "Particulates that did not kill macrophages did not cause an allergic reaction."
However, the vulnerability of macrophages to particulates remains unclear, which is why understanding the events following IL-1α secretion may be key to prevention and treatment.
"IL-1α secretion was followed by the formation of iBALTs. iBALTs are frequently found in infected or inflamed lungs and in patients with asthma," said Osaka University Professor Ken J. Ishii, who led the study. The increase in iBALTs led to an increase in IgE antibodies, which intensified the immune response. On the other hand, mutant mice that were insensitive to IL-1α did not produce iBALTs and reduced IgE responses.
The presence of iBALTs would suggest that a human population could remain susceptible to high levels of asthma attacks even on clear days, as the iBALTs could form on days of high pollution, but the patient could then be exposed to the allergen much later.
This finding suggested that iBALTs could prime the lungs to an allergic reaction, which is why Ishii believes that iBALTs could make a promising therapeutic target to combat the rise of respiratory illnesses associated with air pollution. But first, he said, "we must identify the molecular signals and key chemicals that form these iBALTs."
Materials provided by Osaka University. Note: Content may be edited for style and length.
Disclaimer: DoveMed is not responsible for the accuracy of the adapted version of news releases posted to DoveMed by contributing universities and institutions.
Primary Resource:
Kuroda, E., Ozasa, K., Temizoz, B., Ohata, K., Koo, C. X., Kanuma, T., ... & Nakajima, S. (2016). Inhaled Fine Particles Induce Alveolar Macrophage Death and Interleukin-1α Release to Promote Inducible Bronchus-Associated Lymphoid Tissue Formation. Immunity, 45(6), 1299-1310. DOI: 10.1016/j.immuni.2016.11.010
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.