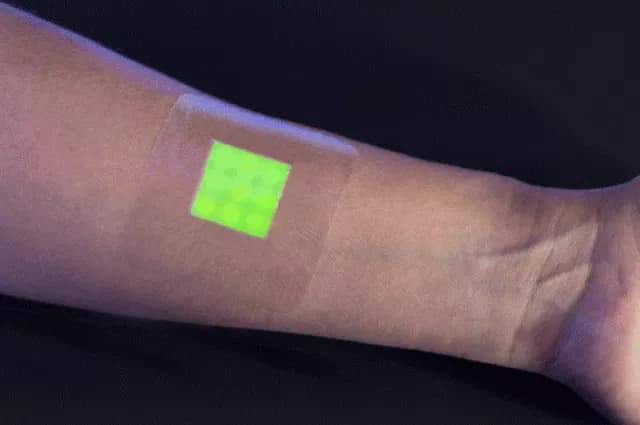
“Smart” Wound Dressing Could Catch Early Bacterial Infection In Wounds
Scientists from the United Kingdom have developed a prototype wound dressing that detects infection-causing bacteria in a fast and accurate manner. The dressing switches to a fluorescent color when pathogenic bacteria start multiplying in the wound, indicating an active infection.
When bacteria begin colonizing a wound, they could either be cleared by the body’s immune process, or they could overwhelm the immune system, causing an active infection. The pathogenic bacteria in wounds could exist as single, independent cells (called planktonic) or could form aggregates. When the bacteria form aggregates, they secrete a slimy substance, which consists of sugars, proteins, deoxyribonucleic acid (DNA), and other organic compounds. This slime is called a “biofilm.” It is believed that the “planktonic” forms of bacteria cause acute infections, whereas the more serious chronic infections occur as a result of bacterial pathogens in “biofilms.”
In the current study, these biofilms have been used as a marker for chronic infection. The researchers used hydrated agarose (generally extracted from seaweed) film in a hydrogel matrix as the dressing. The fluorescent dye containing vesicles mixed with agarose and dispersed within the hydrogel matrix are capable of detecting ingredients of a biofilm and turn a fluorescent color, thus indicating wound infection.
The following were some experiments performed with the prototype wound dressing and the results:
- Clinical strains of Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus and Enterococcus faecalis were established on a nanomembrane for 24, 48 and 72 hours. This produced a biofilm of pathogenic bacteria. When wound dressing was applied to the nanomembrane, a color response was observed within 4 hours of bacterial growth.
- The color change was observed only when the nanomembrane contained bacterial biofilm.
- When compared to planktonic bacterial growth type was tested against the biofilm type, the color response was stronger in the biofilm wound dressing, perhaps because of different rates of growth of the pathogens in planktonic and biofilm forms.
- The dressing was able to detect several pathogenic bacteria in a porcine skin model of burn infection.
The senior author of the study, Dr. Jenkins, says in the iflscience news, “The dressing detects changes in wound bacterial activity. All wounds have some bacteria in [them] – whilst they are kept in check by immune clearance this is not a problem, but when bacteria start to form biofilms and critically colonise the wound, pathogenic changes can result. Our dressing will measure this critical colonisation point,”
An early detection of infection is crucial to a successful clinical outcome. Dr. Jenkins adds, “If used appropriately, we believe it can be used for early diagnosis of post-surgical infection and hence (indirectly) in reducing incidences of sepsis,” added Dr. Jenkins.
However, the process of taking this wound dressing to the public is just beginning. In Dr. Jenkin’s words, “We are working on safety testing, working out a manufacturing pathway, and plan [on conducting] a clinical study in about three years.”
If successful, this “smart” wound dressing should prove to be a great asset in preventing occurrences of infections in post-operative and burn wounds. The probable shortened hospital stay and savings in healthcare costs is likely to be substantial.
Written by Mangala Sarkar, Ph.D.
Primary References
Thet, N., Alves, D., Bean, J., Booth, S., Nzakizwanayo, J., Young, A., . . . Jenkins, A. (2015). Prototype Development of the Intelligent Hydrogel Wound Dressing and Its Efficacy in the Detection of Model Pathogenic Wound Biofilms. ACS Applied Materials & Interfaces. doi:10.1021/acsami.5b07372
Intelligent Dressing Glows When Wounds Are Infected. (2015, October 24). Retrieved November 2, 2015, from http://www.iflscience.com/health-and-medicine/intelligent-dressing-detects-infections-wounds
Additional References
Bjarnsholt, T. (2013). The role of bacterial biofilms in chronic infections. APMIS Supplementum, 136, 1-51.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.