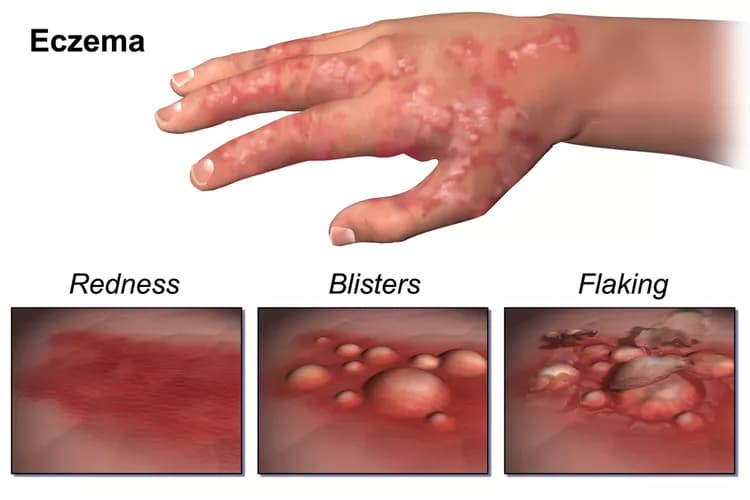
Eczema In Children Has Unique Immune Profile, Offering New Targets For Treatment
Atopic dermatitis, or eczema, is a common skin disorder that usually starts by 5 years of age, but virtually all of the studies that have defined the immune changes underlying eczema and are directing new treatment options have been done in adult skin. A study just published in the Journal of Allergy and Clinical Immunology characterizes immune changes for the first time in the skin of young children with eczema.
"Our findings offer new directions for targeted therapies for children with eczema," says Amy Paller, MD, co-senior author and dermatologist at Ann & Robert H. Lurie Children's Hospital of Chicago, as well as Chair of Dermatology and Professor of Pediatrics at Northwestern University Feinberg School of Medicine. "While some characteristics of eczema in children are the same as in adults, our study showed substantial differences that are important for understanding eczema in children and developing tailored treatments that maximize effectiveness and minimize potential side effects."
Currently, there are no targeted therapies for affected children, who are usually treated with topical steroids and, in severe disease, with immunosuppressant drugs. This new study evaluated both affected and unaffected skin in children within the first 6 months of their eczema, and compared the immune profiles to those in skin from healthy children and also to the affected and unaffected skin of adults with eczema.
The study verified the central and early role of the immune pathway that drives allergy (Th2), which helps explain the association of eczema, asthma, and allergies in kids. In a previous study, Paller and her associates found evidence of activation of this Th2 immune pathway in the blood as well. This pathway is currently the focus of development of targeted therapy for moderate-to-severe eczema, suggesting that these same agents being tested in adults could also be useful in young children. The observed increase in the biomarker for itch (IL-31) in skin points to another useful therapeutic target for children.
In studies of blood samples from children with and without eczema during the first years of the life, the eczema group showed suppressed development of an immune pathway that handles infections (Th1). This observation may help to explain why children with more severe eczema have more widespread infections of herpes and molluscum viruses.
Several differences in the skin of children with eczema raise doubts about findings in adults that are now considered central to understanding eczema. Adult eczema skin is deficient in the naturally produced agents that fight staph infections and certain viruses, and this deficiency has been thought to be an important reason for the high risk of these infections in eczema at all ages. But the levels of these antimicrobial factors in the skin of young children with eczema are very high, suggesting that deficiency does not play a role in the frequent skin infections at early ages.
A characteristic trait of eczema at any age is a poor skin barrier, which leads to dryness and easier entry of triggers of the immune system, such as bacteria, irritating substances and allergens. Filaggrin, a key protein in skin barrier function, is deficient in adults. This has been attributed to both genetic deficiency and immune cell products that prevent production of filaggrin. The deficit of filaggrin has been blamed for the poor skin barrier in eczema. In contrast to adults, however, the skin of young children with eczema was found to have plenty of filaggrin, despite its poor barrier function and skin thickening that is comparable to skin of adults with eczema. This unexpected finding suggests that the filaggrin deficit may not be the driving force for barrier issues and that treatments targeting this protein might not be as beneficial for children with eczema as for adults.
A panel of findings was generated from the blood and skin samples of each participating child affected by eczema. "Our study is the first step toward personalized medicine for children with eczema," says Paller. "We need to collect much more data to start matching targeted treatments to an individual's specific disease characteristics."
Materials provided by Ann & Robert H. Lurie Children's Hospital of Chicago. Note: Content may be edited for style and length.
Disclaimer: DoveMed is not responsible for the adapted accuracy of news releases posted to DoveMed by contributing universities and institutions.
Primary Resource:
Esaki, H., Brunner, P. M., Renert-Yuval, Y., Czarnowicki, T., Huynh, T., Tran, G., ... & Bauer, B. (2016). Early-onset pediatric atopic dermatitis is T H 2 but also T H 17 polarized in skin. Journal of Allergy and Clinical Immunology.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.