What are the other Names for this Test? (Equivalent Terms)
- Mantoux Screening Test
- Pirquet Test
- PPD (Purified Protein Derivative) Test for Tuberculosis
What is Tuberculin Skin Test for Tuberculosis? (Background Information)
- The Tuberculin Skin Test for Tuberculosis is used to check, if an individual is infected with tuberculosis bacteria, which may either be due to active tuberculosis (TB) infection, or a latent tuberculosis infection (in the past). This test for tuberculosis, is a type of delayed hypersensitivity reaction (DHR) to the tuberculin antigen (which is a purified protein derivative (PPD) tuberculin)
- Latent tuberculosis infection is a non-communicable form of tubercular infection, where the patient is asymptomatic.In latent tuberculosis, the TB infection persists for a long period of time (it may last for years). When an individual’s immune system decreases, due to a variety of reasons, the latent infection may then become active, leading to an active TB disease
- The Tuberculin Skin Test is an in vivo screening test that measures an immune response of an individual to the tuberculin antigen (purified protein derivative tuberculin)
- The immune response that is measured is a cell-mediated immune reactivity to mycobacterium tuberculosis antigen. The principle behind the test is the response of T-lymphocyte that has been sensitized to mycobacterium tuberculosis. Individuals who have past infection with TB have circulating T lymphocytes in the blood that are sensitized to mycobacterial antigens.Hence during the skin test, these lymphocytes will cause a skin reaction at the site of Tuberculin Skin Test
It is important to follow a positive Tuberculin Skin Test with further testing, to rule out an active tuberculosis infection. Further diagnostic intervention includes, but is not limited to:
- Medical history including ‘a travel history'
- Physical examination
- Examination of sputum for acid fast bacilli smear
- Culture for acid fast bacilli in the microbiology lab
- Routine chest X-ray (also called chest radiograph)
What are the Clinical Indications for performing the Tuberculin Skin Test for Tuberculosis?
Tuberculin Skin Testing is used as part of a screening process of an individual, for any exposure to tuberculosis infection. Individuals who are at high risk of getting tuberculosis are screened. These include:
- Healthcare workers who come in contact with individuals having active tuberculosis infection
- Individuals diagnosed with HIV/AIDS
- Those who have a weakened immune system, due to chronic steroid therapy, use of immunosuppressive medications
- Individuals inhabiting confined living conditions, such as in refugee camps, correctional facilities, homeless shelters
- Those living/working in nursing homes, working at schools
- Individuals who are on illicit drugs, and such other substances
- Individuals from endemic areas for tuberculosis
- As part of a routine screening check of a new employee (job orientation process)
The Tuberculin Skin Test was used before the availability of the blood test, known as QuantiFERON test, to diagnose latent tuberculosis infection. The Tuberculin Skin Test has a drawback, because individuals who have been vaccinated with Bacillus Calmette-Guerin (BCG) vaccine can test positive with the Tuberculin Skin Test. However, such vaccinated individuals test negative with QuantiFERON blood test. Hence, QuantiFERON test is superior to the Tuberculin Skin Test for detecting latent TB infections, in individuals who have received BCG vaccination.
How is the Specimen Collected for Tuberculin Skin Test for Tuberculosis?
Sample required: None
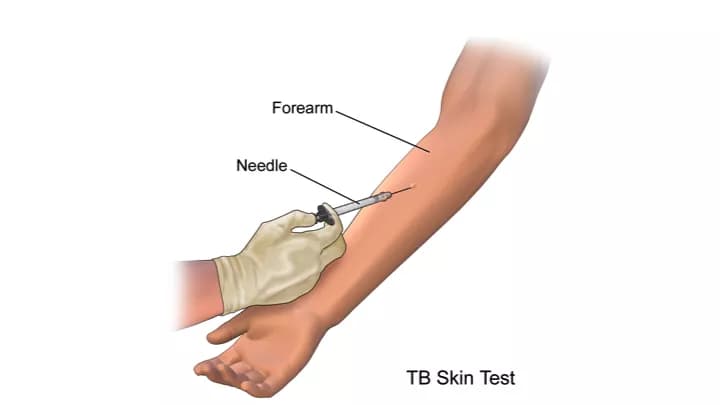
Process: In this test a small dose of purified protein derivative tuberculin is injected into the forearm. The body’s reaction to the antigen is measured after 48-72 hours by a healthcare professional. The reaction to be measured is the induration (raised firm area) and not the erythema (redness).
Preparation required: None
What is the Significance of the Tuberculin Skin Test for Tuberculosis Result?
Positivity of Tuberculin Skin Testresult depends on, the size of the elevated, hard area, or swelling. The reaction is measured by the diameter of palpable raised, hardened area at area of testing, in the forearm. The raised induration is measured in millimeters. If there is no raised area or induration noted, then the result should be interpreted as "0 mm"(negative).
Sometimes, an area of redness (erythema) accompanies the indurated area. The redness should not be measured as area of the reaction; measuring it may result in a false positive reaction interpretation.
The Tuberculin Skin Test results may be positive, negative, or indeterminate.The positivity of the skin test depends on the risk factors an individual may have.
A 5 mm induration is considered positive in the following category of individuals:
- Individuals diagnosed with HIV/AIDS
- Any individual, who has been in contact with an active TB patient. E.g. A healthcare worker who comes in contact with individuals affected by active TB infection
- Patients with recent organ transplants, bone marrow transplant
- Individuals whose chest X-ray is consistent with a prior TB infection, such as scarring or nodule
- Individuals who have weakened immune system, such as those on chronic steroid therapy, immunosuppressive medications
A 10 mm induration is considered positive in the following category of individuals:
- Individuals who take illicit drugs
- Individuals from endemic areas for tuberculosis
- Those who live in confined living conditions, such as refugee camps, correctional facilities, homeless shelters, etc.
- Those living/working in nursing homes, working at schools
- Diabetics
- Laboratory workers performing testing on TB samples
A 15 mm induration is considered positive in the following category of individuals:
- Individuals who are healthy and do not have any of the risk factors mentioned previously (above)
A positive test may indicate a prior exposure to tuberculosis infection resulting in either a latent infection, or an active TB infection.
Rarely, the Tuberculin Skin Test may be false positive. False positive test results can occur with individuals who have infection with other types of mycobacterial infection, such as mycobacterium szulgai, mycobacterium kansasii, and mycobacterium marinum. Individuals who have been vaccinated with BCG vaccination will also test false positive. In such individuals, a positive test does not mean a prior infection. This is a major limitation of the Tuberculin Skin Test.
A negative test result usually indicates a non-exposure to TB infection in the past. Rarely,it may be false negative. A negative Tuberculin Skin Test also does not rule out an active tuberculosis infection, because certain patients, who have a very severe active TB infection, may have a negative Tuberculin Skin Test.
Intermediate results means further testing needs to be performed to rule out an active TB infection. A healthcare provider determines the extent of further testing required.
The disadvantages and limitations of Tuberculin Skin Test include:
- The test requires multiple visits by the individual. During the patient’s first visit, the skin test is administered. During the second visit the body’s reaction to the skin test is measured. On the other hand, a QuantiFERON blood test requires a single visit. During the visit of the individual, a blood sample is drawn via phlebotomy
- The test may require up to 72 hours to be performed
- Each time a skin test is administered, the immune system response is bolstered by subsequent tests.So, it is not ideal to repeat a Tuberculin Skin Test
- Tuberculin skin test requires an individual to measure the site of tuberculin skin test for positivity. The individual, who is measuring the hard area(induration), determines the positivity. Different healthcare providers may measure the areas of induration differently, which may result in a reader bias
- The test is affected by individuals who have previously received a BCG vaccine
Additional and Relevant Useful Information:
Currently, QuantiFERON blood test is the preferred method for testing an individual for prior exposure to tuberculosis infection. The QuantiFERON test, not only has many advantages, but a few disadvantages too.
The advantages of the QuantiFERONtest include:
- The test requires a single visit. During the visit of the individual, a blood sample is drawn via phlebotomy
- The test results are usually available within 24-hours, unlike a Tuberculin Skin Test which may require up to 72-hours to be performed
- Unlike the Tuberculin Skin Test, where the immune system response is bolstered by subsequent tests, a QuantiFERON Test does not have a bolstered immune response, during subsequent testing
- Tuberculin Skin Test requires an individual to measure the site of Tuberculin Skin Test for positivity. A QuantiFERON Test does not require one to measure individually, whether the patient is positive or not. The positivity is determined by a standardized assay and hence, there is no reader bias involved
- Unlike the Tuberculin Skin Test, which is affected in cases, where individuals have received prior BCG vaccination, a QuantiFERON test is not affected by a prior BCG vaccination
The disadvantages and limitations of QuantiFERON test include:
- The specimen has to be processed within 12-hours after collection, because QuantiFERON Test requires well-functioning white blood cells to determine the functionality of the assay. A specimen that is older than 12-hours, results in the white cells becoming less active, or dysfunctional, which may lead to a false negative report
- QuantiFERON testing in children, younger than 17 years age, is being debated. There is limited data available and hence, current guidelines indicate that a QuantiFERON Test should not be used in individuals, less than 17 years old
- Use of the QuantiFERON Test is limited in individuals, who have been recently exposed to mycobacterium tuberculosis bacteria. It may give rise to false negative results
- It also has a limited diagnostic value in immune-compromised individuals, such as those who have genetic immune-compromised disorders, individuals who have active HIV infection, and those who have acquired immunodeficiency syndrome. The test may result in false negative results
- There are other immune-compromised individuals, where the test could be of a limited diagnostic value. These include leukemias, lymphomas, and patients on chemotherapy, individuals with severe diabetes, those who have had recent transplants, and also individuals suffering from chronic renal failure. In such cases, the results may be false negative
It is important to note that a QuantiFERON test does not help one distinguish between a latent infection and an active tuberculosis infection.
- To diagnose an active TB infection, one must have other tests performed, which indicate the presence of acid-fast organisms in sputum, or cultures that test positive for mycobacterium tuberculosis in the clinical laboratory
- It is also important to note that a positive QuantiFERON test may not mean that the individual is having an active TB infection
- A negative QuantiFERON test also does not rule out an active TB infection, because certain patients, who have very severe active TB infections, may have a negative QuantiFERON test
The laboratory test results are NOT to be interpreted as results of a "stand-alone" test. The test results have to be interpreted after correlating with suitable clinical findings and additional supplemental tests/information. Your healthcare providers will explain the meaning of your tests results, based on the overall clinical scenario.
Certain medications that you may be currently taking may influence the outcome of the test. Hence, it is important to inform your healthcare provider, the complete list of medications (including any herbal supplements) you are currently taking. This will help the healthcare provider interpret your test results more accurately and avoid unnecessary chances of a misdiagnosis.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.