What are the other Names for this Condition? (Also known as/Synonyms)
- Acoustic Neurilemoma
- Acoustic Neuroma
- Acoustic Schwannoma
What is Vestibular Schwannoma? (Definition/Background Information)
- Schwannomas are benign tumors that arise from the Schwann cells around the nerves; these tumors are nerve sheath tumors. In a majority of cases, these tumors are solitary. The tumors can occur in the peripheral nerves (arms and legs) and the spinal nerves; intracranial tumors occur in the head
- In the head and neck region, schwannomas typically involve the 8th cranial nerve (specifically the vestibular division of the 8th cranial nerve). Vestibular Schwannomas can affect either one (unilateral) or both (bilateral) sides of the vestibular cranial nerve. When bilateral, it often indicates the presence of neurofibromatosis type 2 (NF2)
- Currently, no causative factors have been identified for Vestibular Schwannoma. The risk factors for the tumor include the presence of NF2 and a positive family history of schwannoma
- Vestibular Schwannomas may be symptomatic or asymptomatic. However, these tumors can cause a host of symptoms including hearing loss and ringing within the ears. Since the tumors affect the ears and their function, these tumors are also known as Acoustic Neuromas
- In rare cases, schwannomas are known to develop into malignant tumors. The tumors can also compress the nerve on which it lies and cause nerve dysfunction
- In a majority of cases, a complete excision by surgery can be curative and the prognosis of Vestibular Schwannoma is excellent. However, the influencing factors include the type of the tumor (whether unilateral or bilateral) and the presence of NF2
Who gets Vestibular Schwannoma? (Age and Sex Distribution)
- Vestibular Schwannoma is typically observed between the age ranges of 30-60 years. It is observed in young, middle-aged adults, and slightly older adults
- It is observed with a higher incidence in females, when compared to males, against the background of neurofibromatosis type 2 (NF2). However, in the absence of NF2, both males and females are equally affected
- Schwannomas have no known geographical, racial, or ethnic preference; they are seen worldwide
What are the Risk Factors for Vestibular Schwannoma? (Predisposing Factors)
The risk factors for Vestibular Schwannoma include:
- A family history of the tumor
- In some rare cases, the presence of neurofibromatosis type 2, a genetic condition that is characterized by the formation of non-cancerous tumors that affect the nervous system
- Schwannomatosis: It is a genetic condition that is a usually seen in adults and manifests as multiple Schwannomas
- Gorlin-Koutlas syndrome: A complex genetic disorder of multiple tumors in the body including multiple Schwannomas
Note: Usually the tumors are unilateral; but, if they are associated with NF2 or schwannomatosis, they can be bilateral. However, this is a very uncommon occurrence.
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Vestibular Schwannoma? (Etiology)
The exact cause and mechanism of Vestibular Schwannoma formation, in a majority of cases, is unknown; they are known to be the result of sporadic mutations. This implies that they do not have a preceding family history of the condition.
- Abnormalities in chromosome 22 is the most common finding
- Multiple schwannomas are known to occur in a background of genetic disorders, such as neurofibromatosis type 2 (NF2), Gorlin-Koutlas syndrome, or a positive family history
- In general, the tumor is believed to be caused by the overproduction of Schwann cells that wrap around the nerve
What are the Signs and Symptoms of Vestibular Schwannoma?
Vestibular Schwannoma may not present any signs and symptoms in some cases, and may be detected incidentally. In tumors with signs and symptoms, these may include:
- The tumors are mostly slow-growing and solitary; they may range in size from 2-10 cm and appear as a firm mass
- Vestibular tumors may cause ear-related signs and symptoms, such as dizziness, loss of balance, pain, hearing difficulties, and tinnitus (ringing in the ears)
- Facial drop and altered touch sensation on the face (facial parasthesia) may also be observed in individuals where the tumor compresses on the facial nerve
- The tumors may affect one ear (unilateral) or both ears (bilateral), when both the nerves responsible for hearing are affected
How is Vestibular Schwannoma Diagnosed?
A diagnosis of Vestibular Schwannoma is made using the following tools:
- Complete physical examination with thorough evaluation of the individual’s medical history (including family history of NF2 or schwannoma)
- Neurological exam of the entire body
- Radiological studies (CT, MRI scan) of the affected region
- Nerve conduction studies of the affected nerve
- Hearing and audiometric tests
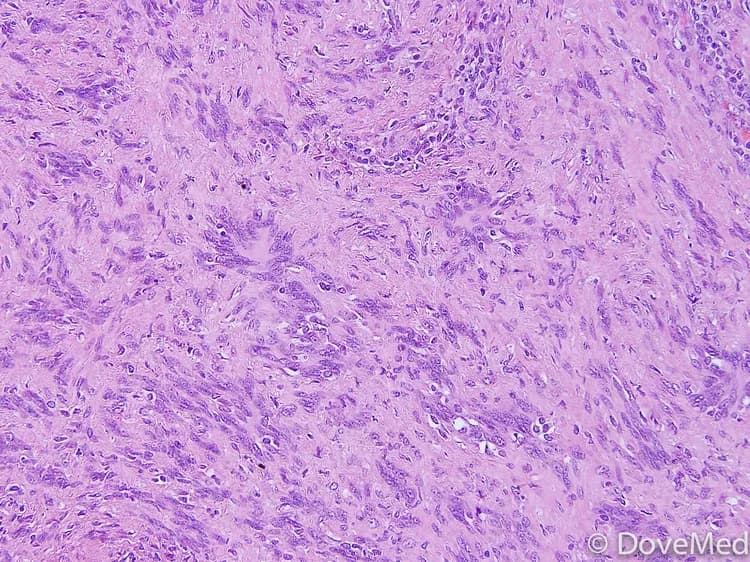
- Tissue biopsy: A tissue biopsy is performed and sent to a laboratory for a pathological examination, who examines the biopsy under a microscope. After putting together clinical findings, special studies on tissues (if needed) and with microscope findings, the pathologist arrives at a definitive diagnosis
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Vestibular Schwannoma?
The complications from Vestibular Schwannoma could include:
- Permanent damage to the nerve causing permanent hearing loss and facial drop
- Large tumors may compress the brain and can be life-threatening
- Damage to the nerve during surgery to remove the tumor. Sometimes, removing the tumor can worsen the signs and symptoms in some individuals
- Infrequently, recurrence of the tumor after surgery, if the tumor is incompletely removed
- Very rarely, Vestibular Schwannomas can become malignant (malignant transformation of schwannoma)
- In rare instances, angiosarcoma (malignant tumor of the blood vessels) is known to arise from a schwannoma
How is Vestibular Schwannoma Treated?
Treatment measures for Vestibular Schwannoma may depend upon the type and location of the tumor. In many cases, if the tumor is small-sized and there are no symptoms, no treatment may be necessary. Periodic observations can be maintained through regular check-ups.
Surgical excision and tumor removal is the usual mode of treatment of Vestibular Schwannoma. A very important criterion for surgery is to preserve nerve function that is affected by the tumor. Surgical treatment options may include the following:
- Microsurgery: The surgery is performed using microsurgical techniques, which can help minimize damage to the accompanying nerve. Since the tumor mostly affects the covering around the nerves, it can be completely removed without affecting the nerve in most cases. The following techniques may be employed:
- Subtotal removal; when the tumor is incompletely removed
- Near total removal; when most of the tumor is removed and there is very little tumor remnants
- Total tumor removal; when the tumor is removed completely
- Craniotomy: It is a surgical procedure wherein a tiny hole is created in the cranium to remove the tumor
- Stereotactic radiosurgery is a relatively new treatment method that can be helpful in some individuals. It is a radiation therapy technique and not an invasive surgical procedure. It can be administered using a Gamma Knife (Gamma Knife radiosurgery)
In case of malignancy, additional treatment options, such as chemotherapy and/or radiation therapy, may be considered.
- Chemotherapy may be used to destroy the tumor cells
- Radiation therapy may be useful in individuals who are not candidates for surgery. Such cases include:
- Individuals with overall poor health status
- The presence of bilateral Vestibular Schwannoma
- Individuals with minimal symptoms
- Treatment of the underlying neurofibromatosis type 2, if present
- Post-operative care is important: One must maintain minimum activity levels, until the surgical wound heals
- Follow-up care with regular screening and check-ups are important and encouraged
How can Vestibular Schwannoma be Prevented?
Current medical research has not established a way of preventing Vestibular Schwannoma.
What is the Prognosis of Vestibular Schwannoma? (Outcomes/Resolutions)
- The prognosis of Vestibular Schwannoma (benign tumor) is excellent, if the tumor can be removed without damaging the underlying nerve. However, bilateral tumors and the presence of neurofibromatosis type 2 can adversely influence the outcome
- Asymptomatic tumors may require no treatment; unless they cause discomfort, affect the quality of life, or affect functioning of the underlying nerve. In such cases, close monitoring of the Schwannoma is a treatment option
- If benign schwannomas transform to malignant tumors (in very rare occasions), then the prognosis may depend upon a set of several factors including the stage of the tumor, its location on the spine, overall health of the individual, and response to therapy
Additional and Relevant Useful Information for Vestibular Schwannoma:
Please visit our Cancer & Benign Tumor Health Center for more physician-approved health information:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.