What are the other Names for this Condition? (Also known as/Synonyms)
- Atrophic Arthritis
- Chronic Rheumatic Arthritis
- Proliferative Arthritis
What is Rheumatoid Arthritis? (Definition/Background Information)
- Rheumatoid Arthritis (RA) is a chronic autoimmune systemic inflammatory disorder that affects the lining of the joints (chiefly of the hands and feet), surrounding tissues, and organs of the body. The disorder is generally noted in middle-aged adults
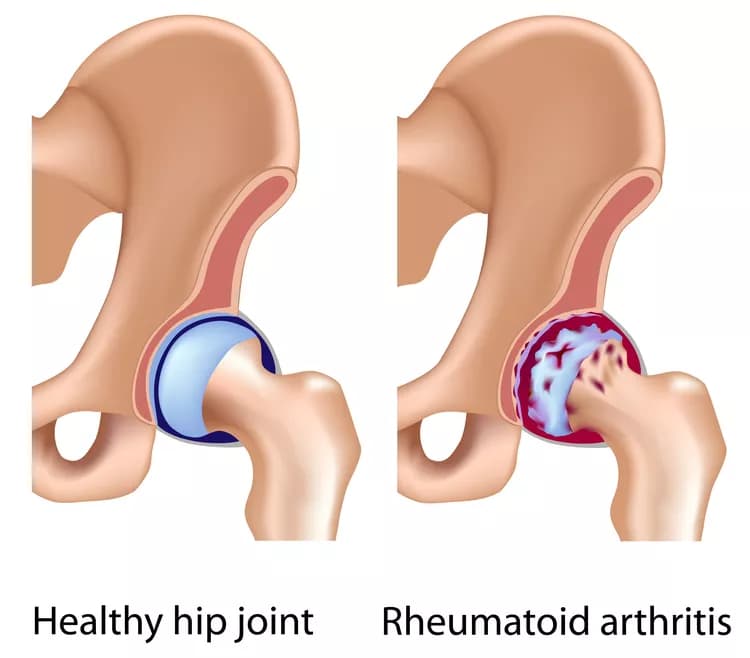
- Unlike the degeneration of cartilage associated with osteoarthritis, Rheumatoid Arthritis affects the lining of the joints. This causes excessive pain and swelling, resulting in bone erosion and joint deformity
- Individuals, who develop Rheumatoid Arthritis often experience fatigue, stiffness, and joint pain. A progression of the condition and a lack of treatment can result in complications such as breathing difficulties, heart diseases, and irreversible joint disabilities
- Following a diagnosis of Rheumatoid Arthritis, the treatment of the condition may involve the use of assistive devices, medications to control symptoms, physical therapy, and invasive procedures, if needed
- The prognosis of individuals with Rheumatoid Arthritis depends on the severity of the condition. An early recognition and adequate (aggressive) management of RA can help achieve optimal outcomes
Who gets Rheumatoid Arthritis? (Age and Sex Distribution)
- Individuals of all ages, gender, and race/ethnic groups may develop Rheumatoid Arthritis
- The signs and symptoms of this joint disorder usually begin to show between the ages of 40 and 60 years
- Middle-aged women are known to develop this progressive disorder at a much higher rate than men. The female-male ratio in this age group is between 2:1 to 3:1
What are the Risk Factors for Rheumatoid Arthritis? (Predisposing Factors)
Common risk factors associated with Rheumatoid Arthritis (RA) include:
- Adult women have an increased risk of developing this disorder
- Individuals in the 40-60 years’ age group
- Studies have indicated that Rheumatoid Arthritis is more common in individuals with a certain genetic make-up. Individuals having an immediate family member/relative with a history of RA, also have an increased risk of developing the disorder
- Various studies have found that smoking is a key contributing factor for the development of the disorder
- Women who have never given birth to any children may have a higher risk for RA. On the contrary, women who have breastfed their children have a decreased risk
- Obesity
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one's chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Rheumatoid Arthritis? (Etiology)
- Rheumatoid Arthritis (RA) occurs when the body immune system attacks the synovial membranes that surround the joints. The resulting inflammation that occurs due an abnormal immune response, causes thickening of the synovial membranes (joint linings)
- Prolonged inflammation may cause damage to the cartilages and bones of the joint. Due to this, the surrounding tendons and ligaments that hold the joint in place are weakened and stretched, slowly causing the joint to lose its alignment and structure
- Some individuals are more prone to infections than others. Research has shown that this may be due to the presence of certain types of genes in them. Infections with certain viruses and bacteria may trigger the development of Rheumatoid Arthritis
- Hence, it has been suggested, that individuals with such genes may have a higher risk of developing RA. Research is currently being undertaken to understand better the genetic risks involved in this autoimmune disorder
What are the Signs and Symptoms of Rheumatoid Arthritis?
- Noticeable swelling and tenderness of the joints
- Pain in the joints that may be severe
- Decreased range of motion of the joints
- Feeling of weakness; a sense of feeling sick
- Loss of weight
- Prolonged stiffness of the joints, especially observed in the mornings (that may improve during the day from use of the limbs)
- Lack of balance and unsteadiness from the joints being affected
- Joint deformity
- Firm lumps beneath the skin
- Elevated body temperatures
- Common locations of Rheumatoid Arthritis manifestation include the small joints of the feet and hands that are affected during early disease stage
- As the condition progresses, the larger joints, such as the elbows, knees, hips, shoulders, and ankles, are also affected
- Often, both the joints (at the elbows, feet, or wrists) are affected, indicating a symmetrical pattern of the condition
- Other body organs that may be affected include the skin, lungs, eye, heart, and blood vessels
How is Rheumatoid Arthritis Diagnosed?
Early-stage diagnosis of Rheumatoid Arthritis (RA) can sometimes be difficult, often due to the symptoms resembling other conditions. There are a variety of diagnostic tests that a physician may use to diagnose RA, which include:
- Physical examination: The physician will perform a thorough physical examination to determine, if the individual has RA. In addition to this, a complete medical history may aid in arriving at a definitive diagnosis. The physician will also check the joints for swelling, redness, tenderness, its reflexes and muscle strength
- X-rays: X-rays use radiation to produce images of the joints. This can help your physician rule out other possible causes of joint discomfort
- Blood test: During the blood test, a needle is used to obtain blood samples from an artery or vein, which are then sent to a laboratory for analysis
- Joint fluid analysis: Occasionally, fluid may accumulate around a joint resulting in pain and disability. Analysis of such joints may provide evidence regarding the cause of joint fluid accumulation. A needle is inserted into the joint space and the fluid aspirated with a syringe. The aspirated fluid is sent for a laboratory analysis. The tests a laboratory may perform include:
- Analyzing what cells are present in the joint fluid
- Chemical composition of the fluid
- Examinations of the fluid under a microscope for the presence of crystals
- If an infection is suspected as the cause for fluid accumulation, then a joint fluid culture may be performed to remove fluid from the joint
- General ultrasound imaging: Ultrasounds are high-frequency sound waves that generate a more detailed image of the joint
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Rheumatoid Arthritis?
The complications of Rheumatoid Arthritis may include:
- Degenerative joint disease such as osteoporosis
- Carpal tunnel syndrome: A gradual, progressive and painful condition that affects the hands and arms, which results when the nerves within the wrist are pinched ()
- Heart disorders due to hardened and obstructed arteries and inflammation of the synovial membranes of the heart
- Breathing difficulties due to abnormal inflammation and scarring of the lung tissue
- Hoarse voice due to the vocal cords being affected
- Some Rheumatoid Arthritis cases may cause permanent disability
- Overall quality of life and work may be severely affected
How is Rheumatoid Arthritis Treated?
Currently, the exact underlying cause of Rheumatoid Arthritis (RA) is unknown. However, conservative treatments may be used to help to reduce pain and improve range of motion within the joint. These include:
- Use of specific assistive devices, such as a cane or walker, is recommended. This may help individuals perform some of their basic everyday activities
- Immunosuppressant drugs may be prescribed to control an active immune system
- Tumor necrosis factor-alpha (TNF-alpha) drugs may be used to block the proteins responsible for inflammation. These medications can help reduce pain, stiffness in the morning, and tenderness or swelling within the joints
- Several other drugs that may be used to treat RA include anakinra, abatacept, rituximab, and tocilizumab
- Disease-modifying anti-rheumatic drugs (DMARDs) may be administered to decrease the magnitude of joint damage that could occur
- Any physical therapy exercises that could aid in strengthening and improving the flexibility of the joints, and also help reduce discomfort. These are generally used only after the signs and symptoms have been controlled or decreased
- Non-steroidal anti-inflammatory oral medications, such as ibuprofen and naproxen, may be used to treat Rheumatoid Arthritis. These medications may help decrease the pain and joint swelling
- Corticosteroid injections help provide temporary relief of symptoms and in improving the range of motion of the joints. It is important to note that corticosteroid injections only give temporary relief. Prolonged episodes of such injections may injure the joints in the long-run
Surgical treatment measures could include:
- Arthroscopic chondroplasty: Arthroscopic chondroplasty is a surgical intervention technique that involves repairing the damaged cartilage within the joint, thus allowing for the growth of healthy tissue in its place. This surgical procedure is performed using an orthopedic device, called an arthroscope, and is useful in treating mild to moderate Rheumatoid Arthritis
- Arthroscopic synovectomy: Arthroscopic synovectomy is a minimally invasive surgical procedure that involves a partial or complete removal of the synovial membrane within the joint
- Bone graft: A bone graft is used to replace damaged or missing bones associated with complex bone fractures
- Total arthroplasty: Total arthroplasty involves the complete removal of cartilage within a joint. The joint is then removed and replaced by a metal and plastic prosthetic implant. A physician will recommend this surgical procedure, if the inflammatory disorder affects the entire joint
- Joint fusion: Joint fusion is a surgical technique that involves the removal of the arthritic part within the affected joint and fusing the surrounding bones together. The purpose of this procedure is to relieve pain, stabilize the joint, and regain some range of motion within the joint
The following self-management measures may be considered the individual:
- Being physically active
- Avoid or stop smoking
- Leading a healthy lifestyle to avoid obesity
- Self-education - in order to understand the nature of the disorder and take steps to control the symptoms, where possible
How can Rheumatoid Arthritis be Prevented?
- Currently, there are no preventable measures associated with Rheumatoid Arthritis
- If early, aggressive and adequate treatment of this inflammatory disorder is undertaken, then the progression of this disabling condition may be slowed or decreased
What is the Prognosis of Rheumatoid Arthritis? (Outcomes/Resolutions)
- The long-term prognosis of Rheumatoid Arthritis depends on the severity of this inflammatory disorder
- If during the early stages, proper and aggressive treatment of Rheumatoid Arthritis is undertaken, then the condition may show an improvement in some patients, without there arising any serious complications
- Other factors that determine the course of outcome of the condition include, whether the disorder is in a flared-up state, in an arthritic remission period, or whether it was correctly controlled with treatment
- A high percentage of individuals who develop Rheumatoid Arthritis, may experience a lifetime of gradual inflammation associated with this debilitating disorder
Additional and Relevant Useful Information for Rheumatoid Arthritis:
Juvenile Rheumatoid Arthritis is an auto-immune inflammatory disorder that predominantly affects the hands and feet of children and adolescents, typically 16 years and younger.
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.