What are the other Names for this Condition? (Also known as/Synonyms)
- Köhlmeier-Degos Disease
- Malignant Atrophic Papulosis (MAP)
- Papulosis Atrophicans Maligna
What is Degos Disease? (Definition/Background Information)
- Degos Disease (DD) is a rare disorder of the blood vessels, wherein there is abnormal blockage of small and medium-sized arteries and veins. This blockage results in cutting-off of the blood supply to various tissues and organs in the body, leading to significant damage of the tissues/organs. The condition is also known as Malignant Atrophic Papulosis (MAP)
- The cause of the condition is unknown; however, 10% of the individuals with Degos Disease are known to have a positive family history of the same. Degos Disease can affect both children and adults
- There are 2 forms of Degos Disease and they include:
- Cutaneous form, when only the skin is involved. It is a milder form of DD
- Systemic form, when the skin and other important organs of the body (such as the gastrointestinal tract, central nervous system, etc.) are involved. It is a severe form of DD
- When the skin is affected, it results in the formation of skin lesions that can bleed, ulcerate, and slowly heal with resultant scar formation. The signs and symptoms of the systemic form of Degos Disease depend on the organs involved. When the GI tract is involved, it can result in abdominal pain, diarrhea, weight loss, and even intestinal perforation
- Degos Disease is a complex and progressive condition that has no cure. The healthcare provider undertakes symptomatic treatment and attempts to reduce the risk of major complications, which include stroke and pericarditis
- The prognosis of Degos Disease is based on the specific form of Degos Disease that is manifested. Individuals with milder (skin form) conditions have a relatively better prognosis in comparison to those with systemic forms
Who gets Degos Disease? (Age and Sex Distribution)
- Degos Disease is an extremely rare disorder with lesser than 200 cases currently recorded in the medical literature
- It is manifested in a wide age range of individuals including children and adults. It is even known to affect infants. The average age of individuals with the condition is 35 years (young adults)
- The condition affects both males and females with a male predominance being noticed (3:1 male-female ratio). However, study reports indicate that the cutaneous form of Degos Disease affects females more than males (1:3 male-female ratio)
- The condition can occur worldwide and no geographical preference is seen. Individuals of all racial and ethnic background may be affected
What are the Risk Factors for Degos Disease? (Predisposing Factors)
- The specific risk factors for Degos Disease (DD) are generally unknown
- 1 in 10 individuals with DD have a family history of the condition
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases ones chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Degos Disease? (Etiology)
The exact cause of development of Degos Disease is presently unknown. The signs and symptoms of DD are observed when blood supply to various organs/tissues in the body are cut-off, leading to significant damage and tissue death (necrosis).
Many possible causes have been put forward by the research community, although no definitive causes have been established. Some of these are outlined below:
- Some studies indicate that there may be a genetic influence, since Degos Disease can run in families. In such cases it has been suggested (but not proven yet) that DD may be an autosomal dominant disorder
- Some researchers believe that it occurs due to abnormal inflammation causing vasculitis (inflammation of the blood vessels)
- It may develop due to a defect in the complement system of the body
- DD could be an autoimmune disorder
Contrary to some reports, Degos Disease is not triggered by a viral infection. The condition is not contagious and does not spread from one individual to another.
What are the Signs and Symptoms of Degos Disease?
The signs and symptoms of Degos Disease depend upon the subtype of the condition and the organs that are involved. In case skin involvement is seen, then it may result in the following:
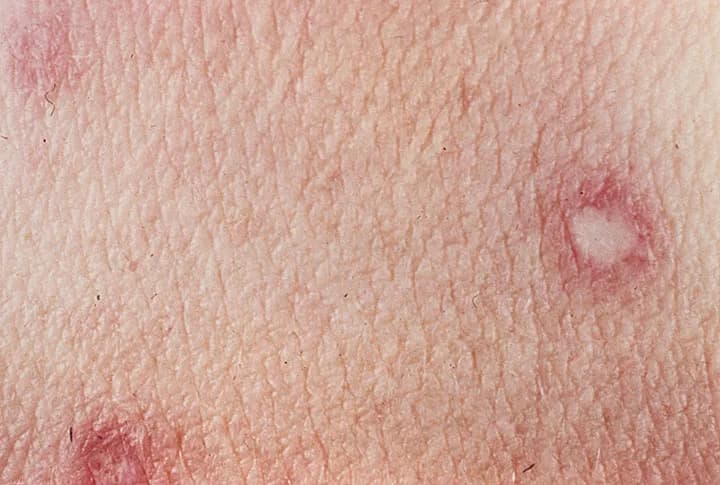
- The presence of raised red papules on skin with white centers
- The skin lesions may or may not be itchy
- Skin necrosis
- The skin lesions are noted on the chest, back, and arms of the affected individual
- Cutaneous signs and symptoms may be present either before or after development of systemic signs and symptoms
In case of systemic involvement, it may result in the following additional conditions (apart from skin manifestations):
- Involvement of the digestive (GI) tract causing:
- Abdominal pain
- Nausea and vomiting
- Diarrhea, constipation
- Weight loss
- Fatigue
- Ischemic colitis, which is injury to the colon due to inadequate blood supply
- Blood in vomit
- Blood in diarrhea
- 1 in 5 individuals show neurological signs and symptoms including headache and dizziness
- Chest pain and shortness of breath
How is Degos Disease Diagnosed?
There are no specific diagnostic tests and methods to identify Degos Disease. The healthcare provider performs a variety of exams and procedures which is then correlated with the clinical signs and symptoms and assessment of medical (family) history background.
The following diagnostic measures may be employed:
- A thorough physical examination and a complete medical history are very crucial
- Dermoscopy: Dermoscopy is a diagnostic tool where a dermatologist examines the skin using a special magnified lens
- Blood test
- Complement testing, antiphospholipid antibody testing, and other tests for lupus erythematosus
- Analysis of the cerebrospinal fluid (CSF)
- Imaging studies, such as CT and MRI scans, of the brain, abdomen, and other regions
- GI endoscopy
- Electrocardiogram for chest pain
- Nerve conduction studies for neurological signs and symptoms
- Skin biopsy of the lesion
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Degos Disease?
The complications of Degos Disease (DD) may include:
- Intestinal perforation due to ischemic bowel; nearly half of the affected individuals develop perforation in the digestive tract. It is a major cause of death in individuals with DD
- The skin lesions can heal with scars and cause cosmetic issues
- Constrictive pericarditis
- Pleural effusion or fluid in the lung
- Stroke, if the brain is involved
How is Degos Disease Treated?
Presently, Degos Disease is incurable; it is also difficult to treat the condition. There are no specific or standardized treatments available for Degos Disease. Individuals often require aggressive therapy to treat the associated symptoms and complications that develop.
- Medications to decrease inflammation of the blood vessels can help decrease the chances of clot formation within the circulatory system
- Medications that alter complement levels in the body have shown promising results; the complement system is part of the body’s inflammatory response
- Pain and anti-inflammatory medications may be used to alleviate the symptoms
- Surgery for intestinal perforation
How can Degos Disease be Prevented?
Currently, there are no specific methods or guidelines available to prevent Degos Disease.
What is the Prognosis of Degos Disease? (Outcomes/Resolutions)
- The prognosis of Degos Disease depends upon the severity of the condition and whether involvement of the whole body is seen (systemic condition)
- Individuals having only skin signs and symptoms have a relatively milder condition; the prognosis in such individuals is generally better and the condition is non-fatal
- A majority of the individuals have systemic signs and symptoms with skin involvement. The survival period following diagnosis is stated to be between 2-3 years
- Stroke, intestinal perforation, and heart abnormalities may be fatal at an early age
Additional and Relevant Useful Information for Degos Disease:
- There is no evidence to prove that oily foods and chocolate-based products have an influence on Degos Disease
- Cleaning the skin too hard with strong chemicals or soaps may aggravate the skin condition. Care must be taken avoid strong soaps and chemicals that could potentially worsen the condition
One should not confuse Degos Disease (DD) with systemic lupus erythematosus (SLE or lupus). SLE is an autoimmune disorder that may affect any area of the body. The differences between DD and SLE are as follows:
- Unlike lupus, DD does not involve the face
- Steroid therapy does not help in DD; but, it can be helpful in lupus
- Unlike lupus, sun exposure does not worsen the symptoms in DD
- There is a high incidence of fatalities involved with severe cases of DD unlike lupus
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals


0 Comments
Please log in to post a comment.