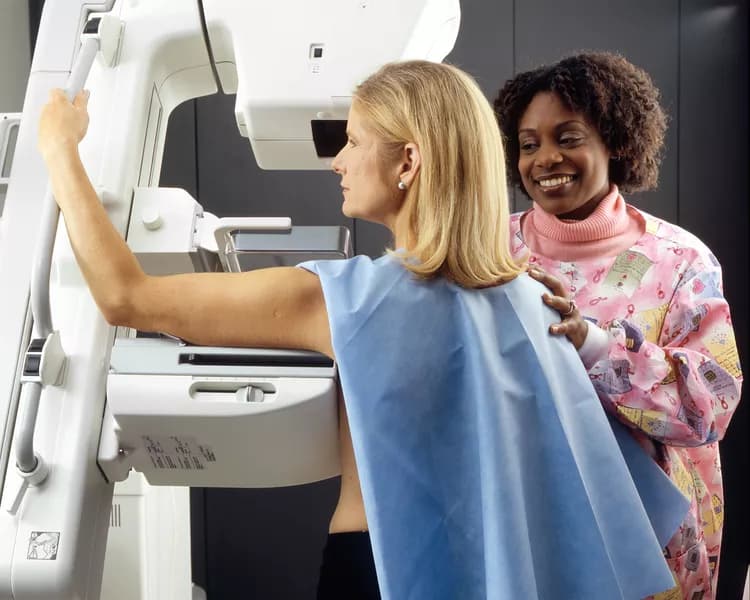
Study: Mammograms May Be Overused For Some Women With Breast Cancer
A new study, published in the journal of Annals of Internal Medicine, suggests no association between breast cancer screening and a reduced incidence of advanced cancer. Also, one in three women with breast cancer detected by a mammogram may be treated unnecessarily because of overdiagnosis (the detection of tumors that would not become clinically relevant). The study investigated an ongoing debate with the potential overuse of mammograms.
"Breast screening can have some very substantial harms," says Karsten Jorgensen, study leader and deputy director of the Nordic Cochrane Centre in Denmark. "And the most important one of those is the overdiagnosis of breast cancers that would never have developed into something life-threatening."
The researchers assessed the potential link between the frequency of breast cancer screening, the size of detected, and the estimated overdiagnosis of breast cancer women between the ages 35 to 84 years in Denmark from 1980 to 2010. First, they measured the occurrence of advanced (>20 mm) and nonadvanced (≤20 mm) breast cancer tumors in screened and unscreened women. Then, they estimated the amount of overdiagnosis using two approaches:
- By comparing the incidence of advanced and nonadvanced tumors among women aged 50 to 84 years in screening and nonscreening areas
- By comparing the rate of nonadvanced tumors among women the ages of 35 to 49, 50 to 69, and 70 to 84 years in screening and nonscreening areas.
The results showed that in the first method approach, 271 invasive breast cancer tumors and 179 ductal carcinoma in situ (DCIS) lesions were overdiagnosed in 2010 (an overdiagnosis rate of 24.4% [including DCIS] and 14.7% [excluding DCIS]). In the results of the second approach showed that 711 invasive tumors and 180 cases of DCIS were overdiagnosed in 2010 (overdiagnosis rate of 48.3% [including DCIS] and 38.6% [excluding DCIS]).
Along with stress and anxiety, a breast cancer diagnosis leads to possible surgery, radiation therapy, and chemotherapy with serious side effects, which is why an overdiagnosis can be detrimental to the patient.
Should women get mammograms?
The American Cancer Society ‘s guidelines recommend mammograms as an option for a woman starting at the age of 40, with annual mammograms starting at the age of 45. Then, the guidelines suggest a cutback in mammograms to once every two years starting at the age of 55.
Other groups, like Fran Visco, President of the National Breast Cancer Coalition, argue that think twice about mammograms, "Women should understand all of these issues and make their own decision if they want to have a mammogram. They should really think very carefully before getting a mammogram."
Dr. Otis Brawley, chief medical officer for the American Cancer Society and professor of hematology, oncology, medicine and epidemiology at Emory University in Atlanta, has a different interpretation of the study.
“This in my mind does not tell us that screening is ineffective,” Brawley told Forbes Magazine while noting that at least eight future randomized studies showed that screening saves lives. The study was not randomized. Also, regional differences of the patients complicated interpretation of the results, which the authors acknowledged.
Brawny acknowledges the limitations of mammography and emphasizes on when and how the screening is being conducted.
“Mammography does save lives, and we should use it, but I’d like us to start focusing on the fact that we need a better screening test,” Brawley said. “I actually think we need to get away from imaging the breast and look toward genomic tests.”
References:
- Jørgensen KJ, Gøtzsche PC, Kalager M, Zahl P. Breast Cancer Screening in Denmark: A Cohort Study of Tumor Size and Overdiagnosis. Ann Intern Med. [Epub ahead of print 10 January 2017] doi: 10.7326/M16-0270
- American Cancer Society recommendations for early breast cancer detection in women without breast symptoms. (n.d.). Retrieved January 11, 2017, from http://www.cancer.org/cancer/breastcancer/moreinformation/breastcancerearlydetection/breast-cancer-early-detection-acs-recs
- N. (n.d.). Frances M. Visco: Breast Cancer Deadline 2020. Retrieved January 11, 2017, from http://www.breastcancerdeadline2020.org/about-nbcc/leadership/frances-m-visco.html?referrer=https%3A%2F%2Fwww.google.com%2F%3Freferrer
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.