What are the other Names for this Condition? (Also known as/Synonyms)
- Benign Enlargement of Prostate (BEP)
- BPE (Benign Prostate Enlargement)
- BPH (Benign Prostatic Hyperplasia)
What is Benign Prostatic Hyperplasia? (Definition/Background Information)
- The prostate is a male reproductive gland whose main function is to produce fluid, to carry the sperms during ejaculation. This gland is located adjacent to the urethra, the tube that helps drain urine out of the body
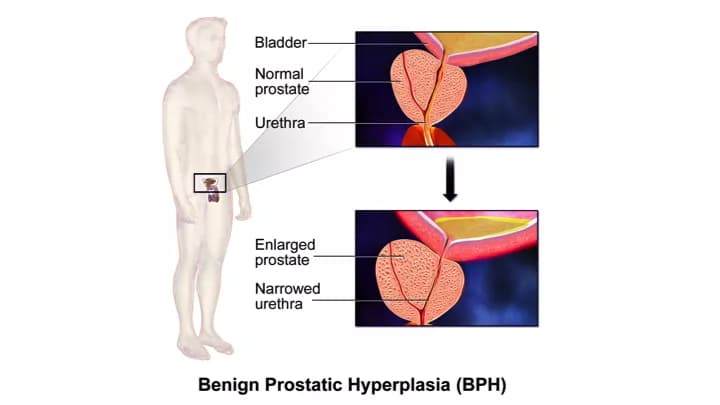
- Benign Prostatic Hyperplasia (BPH), sometimes called Enlarged Prostate, occurs when the prostate gland is swollen, with a resultant increase in its size. It is a relatively common condition in men over 50 years of age
- The symptoms of an enlarged prostate most often occur owing to the swollen gland pressing the urethra. This may result in frequent urination (including at night), urgency to urinate, pain during urination, incontinence, and changes in the color or smell of urine
- Advancing age, obesity, lack of physical activity, certain medical conditions, and abnormalities in testicular function, may increase the risk for Benign Prostatic Hyperplasia in men. Additionally, if there is a family history of the condition, the probability of being diagnosed with BPH is higher
- The exact cause of development of Benign Enlargement of Prostate is not known. However, scientists have put forward 2 theories for the development of this condition:
- The testosterone levels decrease as a function of age, with a resultant higher estrogen-testosterone ratio. The relative increase in estrogen levels promote growth of cells in the prostate gland, leading to its enlargement
- Although, the testosterone levels decrease with age, another male sex hormone, known as dihydrotestosterone, continues to accumulate in the prostate, promoting ongoing growth of the prostate gland
- The diagnosis of Benign Prostatic Hyperplasia is made by a physical and rectal examination, symptom assessment, urine tests and culture for infection, blood tests to rule out prostate cancer, and other tests to evaluate urine flow and retention
- Several complications can arise from Benign Prostatic Hyperplasia, including urinary tract infection, development of urinary bladder stones, as well as bladder and kidney damage
- The treatment for Benign Prostatic Hyperplasia is determined by the severity of the condition. Some of the treatment options include bringing about lifestyle changes, use of medications to relax the muscles (prostate gland bladder) and block dihydrotestosterone synthesis, minimally-invasive procedures to widen the urethra, and surgery to remove enlarged tissue from the prostate gland
- Presently, no guidelines or methods are available for the prevention of Benign Prostatic Hyperplasia. However, getting educated about the condition may help one in recognizing the symptoms and seek medical attention during the early stages itself, which can help avoid complications
- The prognosis of Benign Prostatic Hyperplasia varies between individuals, and is dictated by the individual’s age, severity, development of complications, and response to treatment. In most cases, the affected men find relief from symptoms following treatment by a medical professional
Who gets Benign Prostatic Hyperplasia? (Age and Sex Distribution)
- Benign Prostate Hyperplasia is a common condition that affects older men
- BPH is rarely diagnosed before the age of 40 years (seen in only about 8% of the men). In men aged 51-60 years, its occurrence increases to approximately 50%; and in those aged 80 years or older, to 90% (i.e., 9 in 10 men over 80 years may have BPH)
- The condition occurs globally, and individuals of Caucasian or African descent are more susceptible to BPH than Asian men
- Furthermore, men of African descent are known to develop the condition at a younger age, in comparison to Caucasians
What are the Risk Factors for Benign Prostatic Hyperplasia? (Predisposing Factors)
The following are the risk factors that contribute to the development of Benign Prostate Hyperplasia:
- Advancing age: It increases the risk for BPH; from 8% in men under 40years, to 90% in men over 80 years
- Family history: Individuals with a father or brother with the condition are more likely to be diagnosed with an Enlarged Prostate
- Race: Caucasians and men of African descent are more prone to the condition than Asians (belonging to China, India and Japan)
- Obesity
- Lack of physical activity
- Pre-existing conditions such as diabetes or heart disease
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one’s chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
What are the Causes of Benign Prostatic Hyperplasia? (Etiology)
The exact cause of Benign Prostatic Hyperplasia is not known. However, there is some evidence for the following:
- Changes in testicular function: In young men, specialized cells in the testes synthesize testosterone. A small amount of the female hormone estrogen is also synthesized. With advancing age, the synthesis of testosterone decreases, changing the ratio of testosterone to estrogen. There is thus a relative increase in estrogen levels, which promotes proliferation of cells in the prostate gland
- Along with testosterone, the male gonads also synthesize dihydrotestosterone hormone. Although testosterone levels decrease with advancing age, dihydrotestosterone continues to get synthesized and accumulates in the prostate gland. This hormone promotes continued growth of the gland
As the prostate gland increases in size, it exerts pressure on the urethra (the tube that carries urine out of the body), causing blockages to urine flow. When an individual passes urine, the obstruction to urine flow makes the bladder work harder to expel urine. Over time, the walls of the urinary bladder become thicker. Narrowing of the bladder and the subsequent weakening of its walls, causes an incomplete emptying of the bladder.
What are the Signs and Symptoms of Benign Prostatic Hyperplasia?
The type and severity of signs and symptoms of Benign Prostatic Hyperplasia may vary among the affected individuals. The common signs and symptoms of BPH include:
- Discomfort in the lower abdomen
- Problems with urination that may include:
- Low urine output
- Weak urine stream
- Difficulty in starting urination; having to strain to urinate
- Inability to empty the bladder completely
- Once urination is completed, urine may continue to drip; leaking of urine owing to inadequate emptying of bladder
- Inability to urinate
- Frequent urination
- Strong, sudden urge to urinate, accompanied by fever and chills
- Frequent urination at night-time, during sleeping hours
- Pain during urination
- Changes in color and/or smell of urine
- Blood in urine
- Pain after ejaculation
How is Benign Prostatic Hyperplasia Diagnosed?
The diagnosis of Benign Prostatic Hyperplasia is undertaken through the following tests and exams:
- Complete physical examination and assessment of symptoms
- A digital rectal examination
- Evaluation of personal and family medical history
- Test to measure urine flow rate
- Post-void residual urine test to check the volume of urine retained in the bladder after urination
- Pressure flow studies to check the pressure on the urinary bladder while/during urination
- Urinalysis and urine culture to test for infection
- PSA test: Prostate-specific antigen blood test to rule-out prostate cancer
- Cystoscopy: A procedure in which a tube-like instrument connected to a camera is inserted into the body, through the tip of the penis to view the bladder and urethra
- Trans-rectal ultrasound to check for abnormalities in the prostate gland
- Biopsy of prostate gland tissue, if warranted
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
What are the possible Complications of Benign Prostatic Hyperplasia?
Potential complications associated with Benign Prostatic Hyperplasia include:
- Urinary tract infections
- Acute urinary retention or a sudden failure to urinate (which may be caused by taking decongestant medicines for allergies and common cold)
- The obstruction to urine flow becoming chronic
- Bladder stones
- Damage to urinary bladder
- Kidney damage, owing to infections caused by urine retention in the bladder
How is Benign Prostatic Hyperplasia Treated?
The treatment for Benign Prostatic Hyperplasia may depend on the type and severity of symptoms. It may also depend on the presence of any pre-existing medical conditions. The following treatment measures may be considered:
- Bringing about certain lifestyle changes
- Urinating when an urge to urinate occurs
- Drinking water many times a day, rather than a large volume once or twice
- Avoiding alcohol, particularly after dinner
- Avoiding over-the-counter cold medications with antihistamines
- Routine physical activity
- Pelvic floor-strengthening exercises (Kegel exercises)
- Stress management
- Medications: A combination of medications may also be used
- Alpha blockers to relax the muscles of the neck of urinary bladder and those of the prostate gland, in order to facilitate flow of urine
- Phosphodiesterase-5 inhibitors, used to treat erectile dysfunction, also help relax the muscles of the lower urinary tract. This treatment is generally not recommended for long durations
- Drugs, known to block the synthesis of dihydrotestosterone, called 5-alpha reductase inhibitors may be prescribed
- Anti-muscarinics or drugs that block the activity of neurotransmitter receptors (such as acetylcholine), and relax the smooth muscles
- Antibiotics for inflammation, due to infection of the prostate gland (termed prostatitis)
- Minimally-invasive procedures such as:
- Trans-urethral microwave thermotherapy (TUMT); the use of microwaves to destroy targeted tissue using a catheter with an antenna
- Water-induced thermotherapy (WIT); the use of heated water through a catheter attached to a balloon, to destroy prostate tissue
- Trans-urethral electro-vaporization of the prostate (TUEVAP); the use of electric current delivered via a tube, to vaporize prostate tissue
- Trans-urethral needle ablation (TUNA); the use of a cystoscope to insert needles in the prostate, and destroy tissue through radiofrequency energy
- High-intensity focused ultrasound (HIFU); the insertion of an ultrasound probe into the rectum, and using ultrasound to destroy tissue
- Insertion of prostatic stent; the use of a stent through the urethra to the narrowed part, so that it prevents the swollen prostate from blocking the urethra
- Surgery for severe BPH affecting the quality of daily life
- Trans-urethral incision of the prostate (TUIP); widening of the urethra by making small cuts in the prostrate and neck of the urinary bladder (done using a cystoscope and other special instruments)
- Open prostatectomy; the prostate is exposed by making an incision on skin, and the damaged or enlarged parts excised
- Trans-urethral resection of the prostate (TURP); where an instrument, called the resectoscope, is inserted through the urethra into the prostate gland, and enlarged tissue is snipped and flushed
- Laser surgery: Using a cystoscope, a high-energy laser beam is directed at the enlarged tissue and destroyed
How can Benign Prostatic Hyperplasia be Prevented?
Currently, there are no guidelines or methods available for the prevention of Benign Prostatic Hyperplasia.
- If there is a family history of BPH, then being informed about the condition may help recognize early symptoms, so that prompt medical help may be sought
- Managing certain pre-existing medical conditions may help avoid severe BPH symptoms
- Drinking water or fluids in small quantities intermittently may help reduce sudden urination urge
- Avoiding consumption of excess fluids before bedtime may help reduce the frequency of urination during sleeping hours
What is the Prognosis of Benign Prostatic Hyperplasia? (Outcomes/Resolutions)
- The prognosis of Benign Prostatic Hyperplasia varies from individual to individual. It is determined by one’s age, severity of symptoms, and response to treatment
- In a majority of cases, a proper diagnosis and prompt treatment can lead to relief from the symptoms
- However, if complications develop, there may be permanent damage to the prostate, urethral, or bladder tissues
Additional and Relevant Useful Information for Benign Prostatic Hyperplasia:
Please visit our Men’s Health Center for more physician-approved health information:
Related Articles
Test Your Knowledge
Asked by users
Related Centers
Related Specialties
Related Physicians
Related Procedures
Related Resources
Join DoveHubs
and connect with fellow professionals

0 Comments
Please log in to post a comment.